Everything You Need to Know About Probiotics, Part 1
A new and comprehensive guide to probiotics.
When used correctly, probiotics are a powerful therapy with a surprisingly long list of health benefits. But for many health care consumers, the results of probiotic therapy can be suboptimal due to lack of information or poor probiotic quality.
I’ve recently published a comprehensive, 43-page guide to getting the most out of your probiotic supplements on my website. I’ve also developed this podcast series to highlight some of the key takeaways that you need to know about probiotic therapy. This episode is part 1 in a 3-part podcast series.
Imbalances of the gut microbiota are becoming increasingly common and can cause distressing digestive symptoms and an array of seemingly unrelated symptoms and conditions. These include mood, energy, skin, joint health, metabolism, sleep, immune function, hormone balance, and thyroid health. Thankfully, probiotics can help to correct these imbalances and relieve symptoms. Hundreds of research studies provide evidence for these benefits.
[Continue reading below]
Probiotic Series Intro … 00:00:40
Episode Intro … 00:03:40
Summary of Topics … 00:06:48
Why Probiotics are Important … 00:12:12
Proper Immune System Dev … 00:16:23
An Endless Cycle … 00:19:59
How Can Probiotics Help … 00:22:50
Probiotics from Food … 00:30:22
3 Categories of Probiotic … 00:33:47
The Research … 00:40:18
Episode Wrap Up …00:49:55
Download this Episode (right click link and ‘Save As’)
Dr. Michael Ruscio: Hi everyone. In today’s episode, I am essentially doing a select narration of a comprehensive probiotic article that we are publishing on our website. I’ll have to break this down into two, maybe even three reads, but for those that really don’t like reading and prefer audio, I wanted to give you an audio iteration of the article. I would highly recommend you do check out the article because as you’ll hear in the body of today’s episode, there are many visual aids we created to help make these concepts even easier to understand or to see. So that’s what we will be jumping into today. I also want to mention, and I kind of plug the three probiotics that I’ve created in our line. Our lacto-bifido blend probiotic, our Saccharomyces boulardii probiotic and our soil-based probiotic. Now those are the three tools and understanding how to use those tools, you can do quite a bit to improve the health of your gut.
I think as you either listen or read through this comprehensive probiotic article today, you’ll start to understand why I use these three probiotics and how you can apply them effectively or the 3 for BALANCE Probiotic Protocol that I use in the clinic and recommended in Healthy Gut, Healthy You. We’ve even drawn up in published case studies on our website people who have gone from doctor to doctor and/or been on different diets, been on different probiotics and have never seen complete resolution of their symptoms. Only when they used the 3 for BALANCE Probiotic Protocol, did they achieve the results that they wanted. So the action here is simple. It’s understanding the rationale that is a bit more complicated. It takes quite a precise degree of understanding to give someone what looks like a few simple steps.
[bctt tweet=”Find out the three best probiotics and how to use them effectively. This episode is a narration of the first section of the probiotic article that we are releasing. Perfect for audio learners who might not get around to reading the article.”]It’s the road up to the rationale, the research behind that simple recommendation that is oftentimes maybe an arduous road of either clinical experience or abrogation of references to get there. But then if we do things right, the end result, hopefully, will be somewhat simple. I believe that’s a pseudo paraphrase from Einstein, that if you can’t simply describe the problem, you don’t understand it well enough. So with that, we’ll now transition into what will be a two or maybe even three-part read of the comprehensive probiotic article that is now live on our website. Of course, we’ll have the links for that in the summary on your podcast players.
Episode Intro
DrMR: Hi everyone, and welcome back to another episode of Dr. Ruscio Radio. This is Dr. Ruscio and I am excited today to dig into the comprehensive, behemoth of an article that I spent quite a bit of time putting together about probiotics. As you can probably imagine, I’ve got a lot to say about probiotics, and so I am really excited about this article. Likely you’ve heard my positions on a range of topics regarding probiotics and SIBO, all the way to probiotics and something like joint pain or even brain fog. Or maybe even you’ve heard my criticism that some fairly well-revered conventional gastroenterologists seem to have an overly cautious, unjustifiably cautious, stance on probiotics even in spite of the evidence that doesn’t seem to be require that level of caution.
So, what I wanted to do was take everything I felt to be relevant regarding probiotics and put it in one article so you have everything in one place. When I say everything, what I just outlined gives you a pretty broad range. In addition to that, we’ll include things like quality assurance practices, comparison of the probiotic content of foods as compared to supplements, are probiotics safe for infants, how to use probiotics, and really give you a review of all these topics in detail with the supporting references. No spin, no supplement company influence, no hidden marketing agenda, but rather what is the most effective way to look at probiotics so you can use them to get healthy. Also, on the countervailing perspective here, not being overly optimistic and having a healthy respect for what probiotics can’t do, a really balanced narrative.
Just to clarify, this is an article appearing on our website, so I would highly recommend checking out the article. It may be changed because right now we’re still in the final editing phases, but the article title is Three Best Probiotics of 2020 and How to Use Them Effectively.

So what I’ll do here is read some select passages and kind of toggle in between the narration, and then also give you some asides in my thoughts extemporaneously.
Probiotics Summary
So at a glance, kind of giving you the summary here, imbalances in gut bacteria, or the microbiota, are becoming increasingly common. Part of the driving force behind this is a litany of early life factors such as antibiotic use or lack of breastfeeding, just as two examples. This creates a poorly attuned immune system which then leads to a host of inflammatory conditions. These conditions include but aren’t necessarily limited to gas, bloating, constipation, diarrhea, abdominal pain, reflux. Also, non-digestive symptoms, fatigue, depression, joint pain, skin issues or even thyroid challenges. And I use the word thyroid challenges very intentionally, and we’ll elaborate on that more in a moment. I don’t think we can claim that a lack of intestinal health causes hypothyroidism. It certainly may be a contributing factor, but I want to be cautious there not to oversell the case.
And perhaps more importantly here, probiotics have been shown to lead to clinically meaningful improvements in a number of conditions. This is kind of my loose organization, but high-level scientific support and then limited scientific support for the use of probiotics with the following conditions. We’ll start with high-level scientific support. This usually means there’s at least a couple of clinical trials, if not a meta-analysis. IBS or irritable bowel syndrome (gas, bloating, diarrhea, constipation, abdominal pain), IBD or inflammatory bowel disease, Crohn’s and ulcerative colitis, mood, including depression and anxiety, gut microbiota imbalances (including SIBO), H. pylori, Candida fungus in various pathogens (more to follow on that a little later), and even leaky gut or gut damage, or said another way, intestinal permeability.
Now, regarding limited but encouraging scientific evidence, so this means there’s maybe only one study or the study was more observational, or there is no blinding or control so we can’t attribute too much value to that finding or those findings yet, but they’re certainly encouraging. Cognition, or brain fog, sleep, thyroid health, female hormones, autoimmune conditions, metabolism, blood pressure and cholesterol, although the effect size there is small, and again sleep. So not a bad litany of things that may be aided from probiotics.
It is important to understand that probiotics are also not a panacea. And you’ll hear me say this a number of times because what I see happen on the internet is when there’s evidence supporting a given therapy, you get all of the reasons why you should do that therapy and no reason why you should be bridled in your expectations.

What this leads to, in my opinion, is people who continue on a therapy pretty much forever without recognizing the limitations of that therapy. So we want to strike that correct balance here, which is why I will repeatedly say probiotics are not a panacea but definitely worth performing a trial on.
Also, and again this is kind of the summary here, it’s difficult to obtain a clinical dose of probiotics through foods. In the article, you can see a comparison table. This was actually pretty enlightening to look at, where we took a number of fermented foods and we listed the dose of probiotics side by side the dose contained in a typical probiotic supplement. And you’ll see that the foods are not anywhere near, I’m talking about one-tenth of one capsule of many probiotics. Not to say that foods don’t have a time and a place. I think foods are foundational, but to get a clinical or corrective dose we might need to go beyond foods.
I think one of the more clinically or application-based relevance points here, nearly every probiotic on the market can be organized into one of three categories. This greatly simplifies finding the right probiotic for your gut. I talk about this in Healthy Gut, Healthy You, and will expand upon that in the article and give you some tips for the three categories, how to use them and how to kind of personalize these to your gut.
Another point, try a quality formula from each category. Many will do best using all three together at once. A more comprehensive, tri-pronged support approach. Also, and this is a very important point, probiotics are not condition-specific. Rather we use probiotics to correct imbalances in the gut and then many different symptoms and conditions can improve. The final point here, probiotics are safe for moms and for infants. So that takes us through our summary. Now we’ll get into the elaboration on all these points.
Key Takeaways
What are probiotics?
- Live microorganisms that confer health benefits to the host when consumed
- They exert antibacterial, antifungal and antiparasitic peptides
- We can obtain these through foods like sauerkraut, kombucha, kimchi, or via probiotic supplements
- Are NOT condition specific
- Are safe for moms and for infants
Why Probiotics are Important
It’s probably not very surprising to hear that the microbiota or the balance of bacteria in your gut cannot only cause digestive symptoms but also an array of seemingly unrelated symptoms and conditions, mood, energy, skin, joint health, metabolism, sleep, immune function, hormone balance, and thyroid health. So these imbalances in the gut can lead to these problems. Thankfully, probiotics can help to balance or correct these imbalances. More importantly, this is not just theory, this is one of my pet peeves is when people look at a mechanism and then say, “Ah-ha, so if we can just correct this mechanism by X, then these things should improve.” They don’t tell you that there’s no evidence showing improvements when we actually intervene as such. Well, as we just outlined with the high-level evidence and the limited but encouraging evidence, we do have data supporting to a greater/lesser extent the ability of probiotics to improve this array of different symptoms or conditions. Again, it’s not a bulletproof case for everyone, but we’re not trying to position this as being a panacea.
Okay, so another image from the article, Why Probiotics are Important, we already kind of touched on this but if you’d like to have a nice image to kind of tie this all together, things that are not helping to develop a healthy gut microbiota and therefore detract from proper immune system development are as follows: Overuse of antibiotics, lack of or short-term duration of breastfeeding, Cesarean or C-section birth, reduced contact with animals, dirt and environmental bacteria, overuse of antibacterial soaps, unhealthy diets (low in fiber and high in processed foods and added sugar), sedentary lifestyle and poor sleep habits. Just to underscore this note here, yes, these things actually do affect your gut and microbiota health. It’s not just indiscriminately shoving fiber and probiotics into your gut expecting those to feed the bacteria. The health of the host is actually quite important in dictating the health of the bacteria that grow inside of the host.
So what this does is robs your intestines of the sources of healthy bacteria, reduces the foods needed to feed these healthy bacteria and reduces the proper development of your intestinal immune system, which regulates the immune tone globally.
But also, in kind of self-propagating cycle, if your gut immune system does not form properly, then your gut may not get along with your healthy bacteria and you can get caught in this vicious cycle where your immune system is overreacting to your healthy bacteria. This is one of the main things that I think is left out a lot in gut care, which is a look at the immune system. Because the microbiota is important but also the immune system that houses the microbiota.
Okay. So as we kind of move on here, just to define probiotics, probiotics are live microorganisms, not just bacteria. Note that term. It’s not live bacteria. Saccharomyces boulardii is actually a healthy fungus. So live microorganisms that confer health benefits to the host when consumed. We can obtain these through foods, sauerkraut, kombucha, kimchi, or via probiotic supplements.
Proper Immune System Development
So, moving on, I’m just kind of skimming down the article here to give you guys the most salient points. Let’s go into a little bit more about the proper immune system development which regulates bacteria. It’s important to keep in mind that because your immune system is a major, if not the primary source of inflammation in your body, if you don’t have proper formation of your intestinal microbiota, then you can have a maladaptation of your immune system. That can lead to this propensity toward inflammation. So when you lack the healthy bacteria to regulate your immune system, your immune system becomes overactive and attacks when it shouldn’t. This might be one of the fundamental reasons why gut health is so important because it does seem, to some extent anyway, that the degree to which you have healthy intestinal and intestinal bacteria function, you have a healthy immune system. And this is probably why we see reductions of inflammation, ostensibly inflammation in the brain, inflammation in the joints, once we improve someone’s gut health. As a result of the far-reaching inflammatory effects that are caused by the health of the gut. Remember that inflammation is the weapon that your immune system uses.
So to kind of restate this as concisely as I can, if your intestinal bacteria colony, the microbiota, are skewed, that can irritate or agitate the immune system. The immune system becomes hyperreactive and it reacts with inflammation as the instrument it uses to clean things up. So this is where much inflammation likely comes back to in terms of the initiation point.
This can lead to a cycle. It starts with poor bacterial colonization which leads to poor immune system function which leads to excessive inflammation which leads to, finally, a litany of modern-day inflammatory conditions. These conditions include fatigue, depression and anxiety, brain fog, insomnia, acne or skin conditions, female hormone imbalances, male hormone imbalances, hypothyroidism, and immune system dysregulation and autoimmunity.
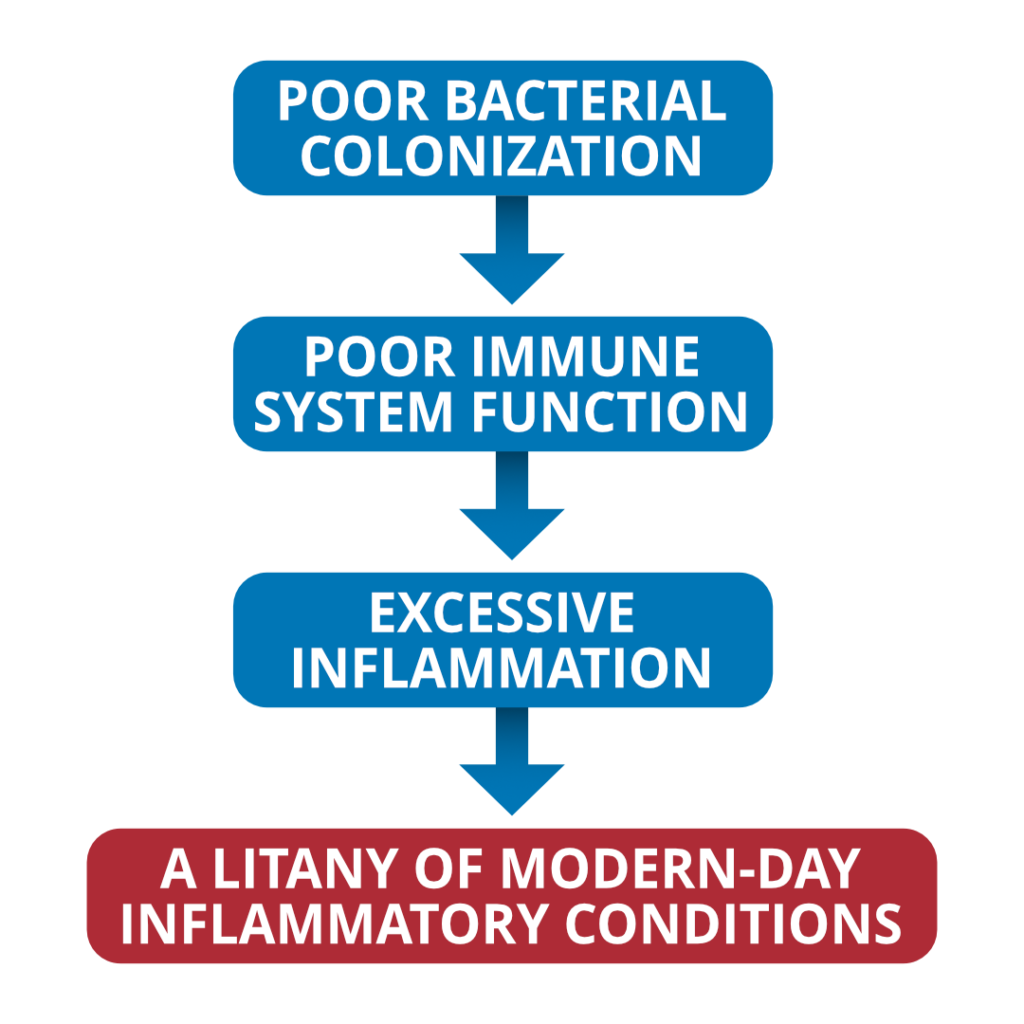
Again, there are varying levels of evidence for either the connection here from an association perspective or more importantly a causal connection, meaning that probiotics can actually remedy these imbalances. But we definitely have clinical trial-level evidence or better for depression and anxiety, for fatigue, one study in thyroid health for autoimmunity, definitely for IBS. So there is definitely a case to be made. To restate this, this fundamental premise, unhealthy gut bacteria equals inflammation. Inflammation equals symptoms. Unhealthy gut bacteria equals inflammation and inflammation equals symptoms. Or if we want to kind of boil this down to the most rudimentary sound bite, that would be one of the takeaways.
An Endless Cycle?
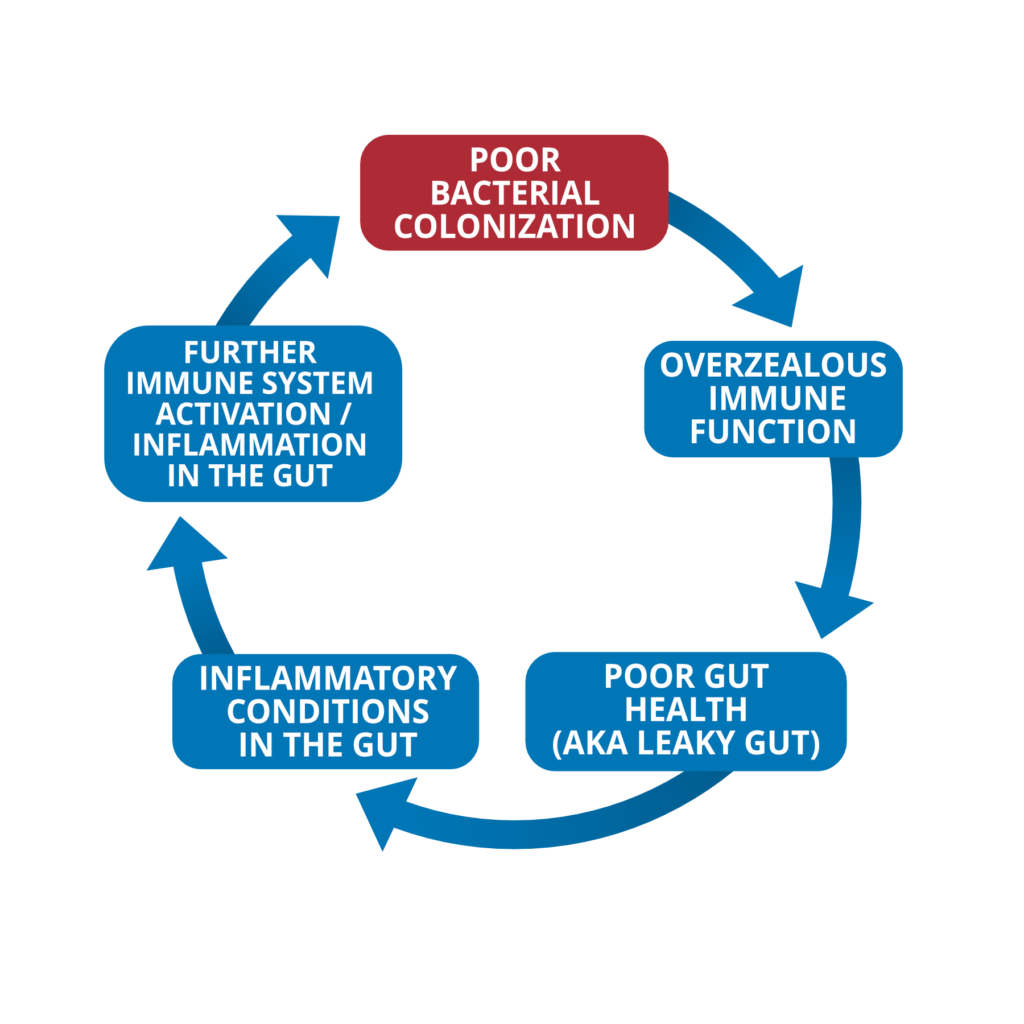
So this can lead to this really unfortunate self-feeding cycle. This is where I think people get stuck and they can’t get out of this situation where they have symptoms. They try a few things, they maybe see a little flicker of improvement, and then they relapse, and they have symptoms and they relapse. The cycle that I believe to occur starts with this poor bacterial colonization in the gut, or you could just say imbalances in the microbiota in the gut. That leads to an overzealous immune system. One of the things that happens is this leads to an even less healthy environment in the gut. So gut health becomes even less healthy, and this could also be described as leaky gut. As that happens, that exacerbates inflammatory conditions in the gut which then calls the immune system to clean up the mess, or makes the immune system even more irritated. All this leads to even poorer intestinal health, more immune activation, more inflammation, more leaky gut in this perpetuating cycle.
Now, the good news is there’s a lot we can do to clean this up. But there’s definitely a cycle here that people can get stuck in. The real travesty is when people chase down the symptoms, most namely as we harped on a few months ago, the droves of people who are told, “Oh, it’s your thyroid. Your fatigue and your insomnia and your depression are coming from your thyroid.” And we’ve published case studies of people who’ve worked with thyroid specialists, who’ve literally written books on this topic, and they have gotten nowhere for a year, a year and a half, only to find their way into our office. We look to their gut and that resolves their symptoms.
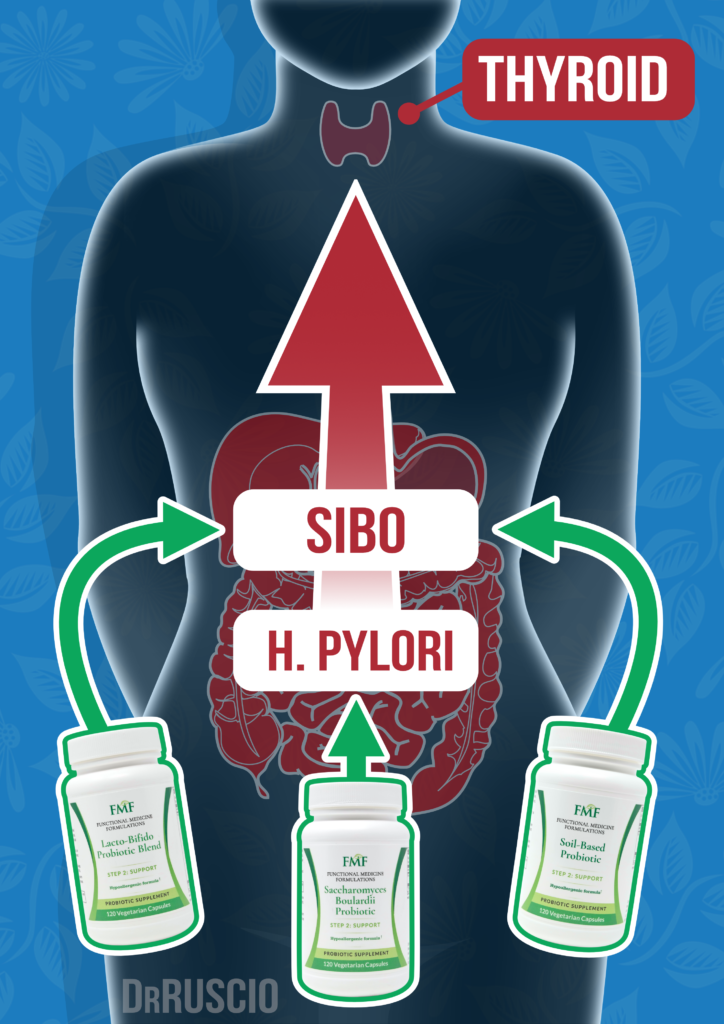
Better yet still, we’ve established external validation of this premise when Dr. Joe Mather and Dr. Robert Abbott have applied these concepts and have been able to help these patients who’ve been suffering needlessly because they’ve been floundering in thyroid world and not seeing any resolution because they were overlooking their gut health. So people definitely get stuck in this scenario. They don’t clean up the gut and they keep chasing down the symptoms they feel are coming from the thyroid, from toxicity, what have you. So, again, not to say everything is caused by a problem in the gut, but there are clearly way too many cases out there of people who are treating the symptoms and overlooking the cause being their gut.
How Can Probiotics Help
Okay. Now let’s transition over to how probiotics help you, kind of the mechanism, what they do underneath the hood so to speak. For every one of these claims, there’s at least one reference I’ve linked to, if not several. You will find them all hyperlinked in this article. Increased bacterial diversity from using probiotics, that’s something that I think is important to mention. Interestingly, there does seem to be this ability of probiotics to not only fight pathogens, that’s the second bullet here, but they also help to increase the diversity and the health of the community. I don’t know if this has been fully bore out but there’s some discussion of this in the published literature. When you have imbalances or even pathogens present, those tend to be poisonous to the healthy bacteria. Once we get rid of those, it actually allows healthier bacterial populations to flourish.
One of the ways in which we allow healthier bacteria to flourish might also be due to reducing inflammation, another one of the bullets from this list. Inflammation does seem to favor the growth of unsavory players and not be hospitable to your good players. So by fighting pathogens and by reducing inflammation, we shift the tone of the ecosystem to be more favorable for healthy bacteria to grow. This might be why we see increased or improved bacterial diversity. Also, there’s this promotion of more rapid recovery from imbalances in your gut ecosystem, again, probably for the reasons we just outlined, and also a reduction of leaky gut. So there’s a lot of good that is conferred by the use of probiotics.
I just want to underscore that probiotics are antibacterial, antifungal and antiparasitic. You’ve likely heard me harp on the idea that patients who have SIBO being told they shouldn’t use probiotics is not only not an evidence-based claim, the majority of the evidence refutes that claim clearly. It also doesn’t seem to be a theoretically sound claim. Anyone who is using probiotics in their clinical practice, or writing about probiotics, should know enough to know they exert antibacterial, antifungal and antiparasitic peptides. So if they do that, you can’t then turn around and tell a patient, “Well, don’t take probiotics because you have SIBO, which means you already have too much bacteria. Therefore, giving more bacteria would be a bad idea.” Again, it’s probably well-intentioned. But it reflects a lack of understanding of the functional mechanism, and, more egregiously, a lack of understanding of what the clinical trial data says. We’ll come back to the studies proving that probiotics are very helpful against SIBO a little bit later.
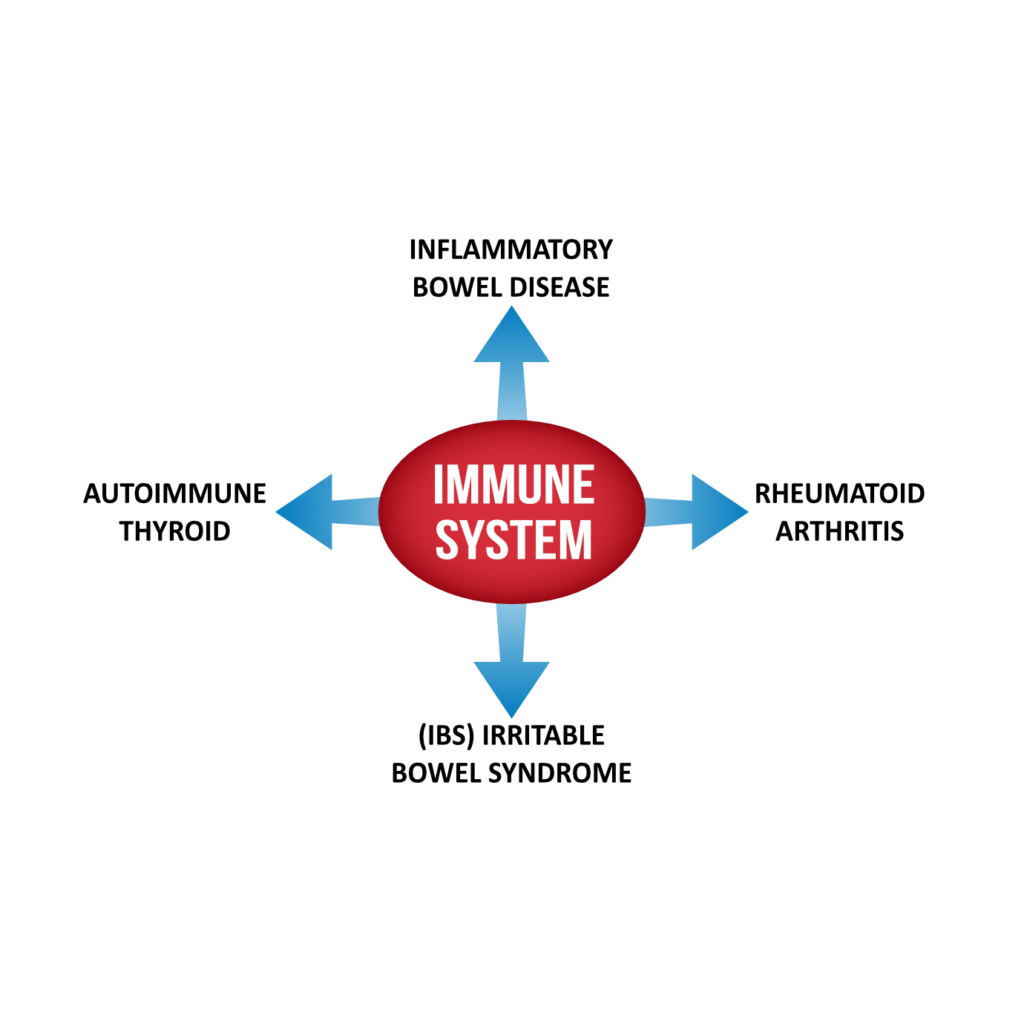


But there are three other components of the benefit of probiotics I want to touch on. These are the immune system, inflammation, and nutrient absorption. Kind of restating what we hashed before, but we broke down a few of these benefits into three images. One, the impact on the immune system. If we improve immune system health, we can see not an exhaustive list here but four things improve as a byproduct of that: Inflammatory bowel disease, rheumatoid arthritis, irritable bowel syndrome, and autoimmune thyroid.
Now in inflammation, another diagram here showing that if we reduce inflammation that will likely lead to improvements in mood, joint pain, brain fog, swelling, and insomnia. And then if we improve nutrient absorption, we can lead to better responsiveness to thyroid medication, we can lead to improvements in fatigue, we can lead to potentially better exercise tolerance, decreased aging, or attenuation of the aging process, and improvements in anemia. So just three images there that I think help to tie some of this together.
Sponsored Resources
I’d like to thank Transcend Labs for making this podcast possible. As per our last interview with Dr. Alex Capano, who has her PhD in cannabinoid research, the best evidence for CBD is regarding the treatment of pain, sleep, and mood conditions like anxiety. You have to be very wary of cure-all health claims. You also have to be cognizant of quality assurance, and this is why I’m happy to say that Transcend Labs pays close attention to this.
They use full-spectrum CBD across all of their products. In fact, they have pretty delicious gummies that I’ve sampled a number of times. They use third party analysis, verifying the safety and potency of all of their products. They use a minimal dosage of 25 milligrams per serving across all products, making it easy to switch from an edible to an oil.
You don’t have to do all these dosage conversions. You’re going to have consistency of dosage across products, and they only use the most effective CBD delivery systems, such as oil, edibles and topical creams.
And to another question here regarding toxins. I think it’s important to touch on the fact, and I’ll quote here, “Liver enzymes, total cholesterol, inflammation, and insulin resistance were all improved as found in a meta-analysis of four clinical trials.” So if we can improve liver enzyme function, it would be suggestive that we can improve someone’s “toxicity”, which is a very kind of vague term. But just to touch on that briefly.
Also, as we’ve talked about before, most probiotics, but not all, most do not colonize you. And I’ll quote here, “The gut microbiota generally shows colonization resistance in which the native microbiota prohibits harmful (or pathogenic) and potentially beneficial probiotic microbes from establishing.” So this is actually a good thing that the adult microbiota is somewhat impervious to colonization because it tells us that you are protected against pathogenic colonization.
Key Takeaways
3 Benefits of Probiotics
- Immune system improves therefore conditions like these improve
- Inflammatory bowel disease, rheumatoid arthritis, irritable bowel syndrome and autoimmune thyroid
- Nutrient absorption improves therefore these improve
- Mood, joint pain, brain fog, swelling and insomnia
- Inflammation improves therefore these improve
- Better responsiveness to thyroid medication, improvements in fatigue, potentially better exercise tolerance, decreased aging, or kind of attenuation of the aging process, and improvements in anemia
Probiotics from Food, It’s Not Enough
Okay. Now moving on to the table I previously mentioned, probiotics from food. This is one of the more insightful diagrams I’ve put together in quite some time. Looking at sauerkraut, sauerkraut contains four strains of different bacteria totaling three billion CFU.
Now that three billion CFU per cup of sauerkraut is equivalent to one-eighth of a capsule of our Lacto-Bifido Blend probiotic. So it’s something, but certainly hard to get to a clinical dose, especially when considering that the dose that we recommend of the Lacto-Bifido Blend probiotic is anywhere from maybe two capsules to eight capsules per day.
Yogurt, 2.5 billion CFU per cup, which is equal to one-tenth of our Lacto-Bifido Blend probiotic. The reason why I’m comparing this to the Lacto-Bifido Blend probiotic is because what you’re seeing in most of these probiotic foods is a mixture of various Lactobacillus strains. So the most proximal comparison would be to the Lacto-Bifido Blend, being the category one probiotic-containing mostly Lactobacillus and Bifidobacterium strains.
Lacto-fermented pickles, 1.3 billion CFU per pickle, which is equivalent to .05 capsule of Lacto-Bifido Blend. Kefir, 2.5 billion CFU per cup, one-tenth of a capsule of Lacto-Bifido Blend. Kimchi comes in as the winner at 11.5 billion CFU per half cup, and that’s equivalent to about one-half of a capsule of Lacto-Bifido Blend. So, yes, we see some notable probiotic amounts in these foods. But I’m hard-pressed to say someone’s going to get a clinical dose that might be able to move them kind of over a hump of imbalance. So I want to speak to those who have a tendency to drift toward absolutism. This doesn’t mean that I’m saying probiotic foods are useless. I would encourage people to incorporate these into their diet. But you may not be able to get a clinically sufficient dose, especially if you have significant inflammation, dysbiosis, imbalances, from the foods alone.
Okay. Now on to what I feel to be one of the most relevant aspects of this article, simplifying probiotics. And you’ve likely heard my spiel on this, but very important to mention and to clearly distinguish that nearly every probiotic product on the market can be classified into one of three categories. And I think a lack of understanding this is really part of the reason why people tend to flounder on the merry-go-round of various probiotics without ever really gaining enough clarity to say, “Okay, here’s the deal, here’s what I’m going to do. And then once I’m done with this experiment, I can then close the book on my probiotic experimentation.”
Three Categories of Probiotic
So when you understand this, you don’t have to jump from product to product to product to product. You can go through a comprehensive probiotic protocol, reevaluate, and then say, “Okay, I’m either totally devoid of symptoms and I’m done on my gut health healing journey or I need to layer in additional therapies.” This is exactly what I outline in Healthy Gut, Healthy You. It’s crucially important to understand because the amount of confusion I see with patients regarding probiotics is ridiculous. Phyllis’s case study beautifully illustrates this. She was on a low FODMAP diet for about a year and using various probiotics. She came into my office, we did nothing other than get her on all three categories of probiotics at the same time. So she used three different probiotics at once. And within two months all of her symptoms were gone.
It’s not to say that this is going to resolve all the problems for everyone. But you want to go through this protocol, ideally, go on all three probiotics, and then reevaluate. And if you have to do more, you maintain the three-probiotic protocol. Or, if you had a reaction to one of the three, you only use the two that you tolerated. And then you move onto to subsequent steps in the gut-healing algorithm.
So the way to think about this is if a probiotic helps support balance in the gut ecosystem, one probiotic formula is akin to a stool that you would sit on, like a chair with one leg. Now one leg of support for a stool does support balance, but it’s not robust support of balance. It can be a little bit wobbly. So using all three probiotics at the same time is akin to having three legs of support underneath your stool.

That’s much more conducive to achieving and maintaining balance. The three legs are really the three categories. The first category of probiotic is the Lactobacillus-Bifidobacterium Blend probiotic. There are about 500 clinical trials using this type of probiotic. If you look on the label, you’ll see predominantly Lactobacillus and Bifidobacterium strains on the ingredient list. So that’s your category one.
Category two, where there are just over 100 clinical trials is Saccharomyces boulardii. The Saccharomyces boulardii is actually a healthy fungus. So it may support the gut in a slightly different way. It may occupy a slightly different gut niche. And then category three, this type of probiotic is a non-lactic acid-forming probiotic, so it’s different than the Lactobacillus and Bifidobacterium category. This category three is also known as soil-based or spore-forming probiotics. And this contains various Bacillus strains. When we use all three of these together, that seems to be the most conducive to support imbalance in the gut.
Now, that statement is my only clinical observation. There’s nothing published to support that yet. I don’t think the researchers have had a chance to really see this in clinical practice. Because I don’t think most probiotic researchers are really experimenting with probiotics to the extent that I am. In fact, this is something that I just kind of stumbled across, where I used to try to individualize the probiotic to the individual. This is years ago before we had the wealth of research to pull from and we only had a handful of initial studies that suggested, “Oh, maybe people with diarrhea do better with Saccharomyces boulardii. Maybe people with brain fog do better with Lactobacillus, Bifidobacterium,” which is not true at all. I’ll outline that a little bit later in the article here.
But I would start with one formula and people would see some improvements. And then I would say, “Well, hmm, if they’re seeing some improvements from the one, what if I added a second or a third? Would that potentially be able to circumvent the need for antimicrobial therapy?” It turns out that happened, and it happened again and again and again and again and again where one probiotic was helpful, I established that initial finding, and then we added in a second or a third and patients often saw a full symptomatic resolution just from that and did not need antimicrobial therapy. So then I just started going right to the three at once and the results became even more striking. Phyllis’s case is a prime example. This is someone who’s been on the gut-healing journey for a couple of years and was on probiotics and low FODMAP prior, and her symptoms completely resolved in about two months after starting on the three-probiotic protocol. So there’s definitely something here. And, again, why this works so well is it seems that these three different categories are more comprehensive support to balancing and healing the gut.
So, again, and there’s a diagram in the article that essentially depicts a one-legged stool and a three-legged stool, just to try to help tie together this concept as concisely as possible. And also an image that gives you a graphic representation of the three different categories of probiotics, so your Lactobacillus and Bifidobacterium-predominated blends. So there might be anywhere from seven to 15 strains, and most of those will be Lactobacillus and/or Bifidobacterium. Category two, your Saccharomyces boulardii. And then category three, your soil-based or spore-forming using various Bacillus species.
Key Takeaways
Three Categories of Probiotics
The Research
Next in the article, I talk about the research with the Lactobacillus and Bifidobacterium probiotic blends, the category one. Again, there are a little over 500 trials assessing their validity, so pretty robustly studied. These have been shown to help with the reduction of inflammation, modulation of the immune system, production of healthy proteins like short-chain fatty acids and immunoglobulins, or substances, not necessarily all proteins, reducing factors that cause biofilm production And they’ve been shown to help with a litany of even non-gut related symptoms. I mean infant diarrhea would be gut but vaginal infections, urinary tract infections, tooth decay, diabetes, even lactose intolerance. So pretty good research for category one, the most well-studied category.
Category two, our Saccharomyces boulardii, a little over 100 studies here. Benefit has been shown for IBS, for diarrhea, for Clostridium difficile infections, for Crohn’s disease, also more broadly inflammatory bowel disease, the ability of Saccharomyces boulardii to fight imbalances including the ability to fight fungal infections, even Blastocystis hominis, and even one interesting study that found that Saccharomyces boulardii increased the effectiveness of antibiotics when co-administered. Probably the most exciting here is one study where S. boulardii was shown to be as effective, as effective, as antibiotic Metronidazole, or Flagyl, in the treatment of Blastocystis hominis.
People have asked me why I have such good results with Blasto. First of all, I don’t think I have such good results, I just think I do things in a logical sequence of steps, which that logical sequence of steps ends up allowing you to get great results across the board. So there’s not this magic Blasto protocol, but rather we start with diet and lifestyle, which encourages the healthiest ecosystem possible. Then we layer in probiotics, including Saccharomyces boulardii. Then the final step, or not the final but the next step, would be antimicrobial agents. Part of the reason why I seem to have better results potentially than others with Blasto, this is what patients have told me and just knowing that we seem to be able to clear Blasto most of the time while patients report an inability to ever clear Blasto, might be because we’re laying this healthy foundation, in part using Saccharomyces boulardii which was shown to be as effective as Metronidazole in treating Blasto. But then, if we need to, we layer on top of that antimicrobial therapy.
So then on to category three, your soil-based probiotic. In the article, we list about 14 clinical trials, although, with some slightly different strains that are available more so in Asia, there’s another 20 or so. Not nearly as many studies as the other categories of probiotics, but still some impressive research. What’s novel about these is that they may act to replace some of the missing exposure to bacteria we are lacking from reduced contact with animals and dirt and such.
Now, some of the findings from this category of probiotic: Improved IBS, essentially diarrhea, abdominal pain, bloating, stool consistency, reduced or a slight benefit for constipation, leaky gut, inflammation, respiratory infections, and the ability to be antimicrobial or to secrete antimicrobial peptides. So something I wish people could better understand is when you look at all of the probiotic research, you see a number of trials showing benefit using category one probiotics. They all differ slightly but they all fit within to the category one designation.

Then a number of trials showing benefit with category two probiotics. Now those are all pretty much the same because there’s only one strain, Saccharomyces boulardii, whereas the category one you have some nuanced differences in the exact strains. There might be seven, there might be 10, there might be 12, there might be 15. They may include Bifidobacterium infantis or Bifidobacterium longum, or they may not. But when you see, “Wow, here’s one study showing benefit with one formula, here’s a different formula showing the same benefit. Here’s a different formula, again showing the same benefit,” you get off of this probiotic merry-go-round where it’s, “Here’s the special probiotic and here’s our clinically-proven strains.” It’s all fine and good if a company wants to market the benefits of their probiotic, but if you don’t have I guess someone like me to give you this different vantage point from someone who’s looking at all the literature, then you’re only making your health care decisions based upon marketing claims which may be truthful but selectively citing their support and leads you into this kind of tunnel-visioned perspective on probiotics.
If we can step outside of that, if when you go and you visit a really attractive looking sales page for a probiotic that promises to cure the world, that may be really attractive looking but it may be an attractive tunnel vision into a narrowed perspective on probiotics that is not conducive to your mastery of how to use these and ability to overcome imbalances in your gut.
Again, it is important to understand that improving your health is not about the one special probiotic or the one strain or the one formula with the most studies behind it. Again, it’s not to say we want to turn a blind eye to science. Obviously we want to use the science, but I guess we could say a somewhat rudimentary understanding could get you to an attractive marketing claim for a probiotic, a highly expansive understanding could get you past that to a more freeing and empowering perspective that there’s no one magic formula but there are these three categories and these can be used together in this kind of three probiotics for balance protocol. That seems to be, at least in my clinical observation but it’s also informed by the literature here, the most effective way to use these probiotics.
Quality is also very important. So we can’t go to the cheapest probiotics necessarily on the shelf because, as we’ll detail later, quality assurance does matter. I cringe when I say that because I’ve heard so many supplement companies that use this as a way to market, even though they’re doing the same quality assurance practices as everyone else. So I’ll give it to you straight when we get to the section on quality assurance. There are clear quality assurance practices we need to hit. There are definitely documented shenanigans going on in probiotics. But it doesn’t mean that we can jack the price up and offer the most expensive probiotics as the savior to safeguard against these shenanigans. There’s a reasonable balance that can be struck and there are some pretty clear cut quality assurance practices that we want to make sure are hit.
Key Takeaways
High-level scientific evidence for the use of probiotics with the following conditions
- IBS (irritable bowel syndrome) – gas, bloating, diarrhea, constipation, abdominal pain
- IBD (inflammatory bowel disease)
- Crohn’s and ulcerative colitis
- Mood, including depression and anxiety
- Gut microbiota imbalances, including SIBO, H-Pylori, Candida fungus in various pathogens
- Intestinal permeability
Limited (but encouraging) scientific evidence for the use of probiotics with the following conditions
- Cognition, or brain fog
- Sleep
- Thyroid health
- Female hormones
- Autoimmune conditions
- Metabolism
- Blood pressure and cholesterol
Episode Wrap Up
In the next episode we’re going to go into is entitled Your Doctor Could be Wrong, Why a Science-Based Summary Matters. And I’m really going to go into, in a very concise fashion, the main details that combat the perspective that probiotics have no evidence behind them. In fact, if people want to go through a fun exercise, I did this a few months ago, I searched probiotics or best probiotics, or something like that, on YouTube. And the first couple of videos that came up, some of these videos were god awful. If I’m being totally honest, it was a bunch of platitudinous BS, “Well, probiotics are interesting but we don’t have enough research yet so make sure don’t skip the use of any proven treatments at the expense of probiotics,” and blah, blah.
I being really candid right now but it’s infuriating to me because some of these poser doctors on the internet, and when I say poser doctor I mean someone who’s clearly a doctor, I’m not suggesting they’re lying about their credentials but they’re holding themselves up as an expert and they’re hiding behind BS, vague claims, pretending like they know what they’re talking about and using these, “Well, they’re interesting but we want to be cautious because there’s not enough evidence yet” BS recommendations rather than doing the hard work and digging into the details and saying, “Holy cow, there are over 500 clinical trials here. There are even meta-analyses for,” let’s say, “IBS with category one probiotics, even meta-analyses that have consolidated to only the highest-quality clinical trials. And, yes, even when scrutinizing to that standard of evidence, the benefit still rings significant.”
So I don’t mean to be getting overly emotional here, but what bothers me is that these are some of the leading results you see, in this case on YouTube, and they are so ill-informed. And it irritates me when people are, in my opinion, putting out content because they’re trying to build a website or build a platform, but they’re not doing the hard work to support their “expert opinion”, and it hurts you, the consumer, because you are being given poor advice. So that is the next section we’ll pick up with, Why Your Doctor Could be Wrong, and Why a Science-Based Summary Matters. Not the argument from authority, “I’m Dr. Schmo-and-Schmo and I went to school 10 years ago. I haven’t been reading enough of the science but I’m still going to rest on my laurels.” So, yeah, probably good I take a minute here to cool off. But the reason why I get a little bit emotional here and worked up is because it harms patients. Now, we don’t want to be a zealot and make promises regarding probiotics that aren’t substantiated, but at the same time these vague dodges on the question of can probiotics help me and how do I use them really hurts people. So that is where we will pick up next time.
Dr. Michael Ruscio is a DC, natural health provider, researcher, and clinician. He serves as an Adjunct Professor at the University of Bridgeport and has published numerous papers in scientific journals as well as the book Healthy Gut, Healthy You. He also founded the Ruscio Institute of Functional Health, where he helps patients with a wide range of GI conditions and serves as the Head of Research.


Discussion
I care about answering your questions and sharing my knowledge with you. Leave a comment or connect with me on social media asking any health question you may have and I just might incorporate it into our next listener questions podcast episode just for you!