Will Sleep Vitamins Get You a Better Night’s Rest?
When, Why and How to Use Sleep Vitamins and Supplements
- Key Sleep Vitamins and Supplements|
- Other Sleep Vitamins|
- Importance of Sleep|
- The Sleep-Gut Connection|
- Steps for a Better Night’s Sleep|
- Obstructive Sleep Apnea?|
When sleep doesn’t come easily, your health and wellbeing can really suffer. Often, something obvious like aches, pain, or mental stress initially triggers insomnia. Other times, the cause is harder to pinpoint, or can be due to imbalances in your gut. Whatever is underlying your symptoms, sleep vitamins and supplements like melatonin are an option worth exploring, together with changes to diet and lifestyle.
In this article, we’ll look at ways you can sleep better, and which sleep vitamins and over-the-counter natural sleep aids may be helpful as part of an overall good health approach.

Key Sleep Vitamins and Supplements
We’ll look at some of the diet and lifestyle basics that can underpin a good night’s sleep further down this article. But if you’re struggling with sleep issues right now, a sleep supplement might have a more immediate effect.
The efficacy of different sleep vitamins varies, and everybody’s experience may be quite different. But sleep vitamins and supplements are less likely to be addictive than sleeping pills, and also less likely to have side effects or to cause daytime drowsiness.
Below are some of the sleep supplements you can try and the evidence behind them, starting with the two that are potentially most useful: melatonin and probiotics.
Melatonin
A key sleep vitamin that many people with sleep issues can benefit from, melatonin is a serotonin-derived hormone secreted by the pineal gland (a tiny organ close to the center of the brain). It signals to your body that it’s time to prepare for sleep, increasing drowsiness. When everything is working well, melatonin is released in a daily rhythm, with levels going up when it gets dark.
However, sometimes you may not be naturally producing enough melatonin, or may be producing it out of sync.
Jet lag, exposure to bright artificial light in the late evening, poor diet, stress, and gut dysbiosis (not enough good gut bacteria) can all disrupt the normal production of melatonin [1, 2, 3].
This is where a melatonin supplement can come in — of all the sleep vitamins, it’s the most well researched. Several systematic reviews of clinical trials suggest melatonin supplements can [4, 5, 6]:
- Help to decrease the time it takes to fall asleep,
- Improve sleep duration and quality
- Regulate the sleep-wake cycle
That said, melatonin didn’t improve sleep in trials involving menopausal women and older people with dementia [7, 8].
Correct Melatonin Dosage
Melatonin supplements come in a variety of strengths, anywhere between 0.1 mg to 10 mg, given up to two hours before bedtime [9].
Anecdotally, and from the feedback we’ve received from patients, higher doses don’t necessarily produce a bigger benefit. Research hasn’t explored this yet, but some people seem to find that higher dosages actually start to become counterproductive, interfering with sleep rather than improving it.
That’s why, for most people, I’d recommend starting with a lower dosage. Around 3 mg of melatonin at bedtime seems to be the sweet spot that produces the best results in my clinical experience, but the ideal dosage varies from person to person.
If the current dose of melatonin you are taking doesn’t work for you, you may want to experiment with decreasing (rather than increasing intake) to see how you respond. As with anything else, listen to your body.
Probiotics
Clinical trials have shown that taking probiotics can work as a sleep aid, improving sleep quality and reducing sleep disruptions for healthy individuals and those with depression, insomnia, and work-related stress [10, 11, 12, 13].
This is likely to be because probiotics can help to improve gut dysbiosis and inflammation, which then positively affects sleep quality via the brain-gut-microbiome axis [14].
Other Sleep Vitamins and Supplements

Beyond melatonin and probiotics, there’s a burgeoning range of other sleep vitamins purported to help you get a more restful night. Some of these may indeed be helpful, while for others the evidence is much more “sketchy.” The table below splits sleep vitamins and supplements into high, mixed and low standards of evidence for easy reference.
Remember that dietary supplements, including sleep supplements, are not controlled or regulated by the FDA (Food and Drug Administration), so it’s always worth doing your homework to choose a reputable brand. Also, check for any side effects or contraindications that may mean a particular product is not suitable for you.
Strongest Evidence of Benefit
| Sleep Supplement | What the Research Says | Citations |
| Passionflower | Shown to help treat adult insomnia (the effects of passionflower appear similar to zolpidem, a pharmaceutical sedative) | [15, 16] |
| Lemon balm (Melissa officinalis) | May safely improve sleep quality, duration, and efficiency | [17, 18] |
| Tryptophan | High doses (1000 mg+) of this amino acid may improve sleep quality, efficiency, and duration. Tryptophan (with help from vitamin B6), helps make serotonin, and, in turn, melatonin. | [19, 20] |
| L-theanine | Shown to moderately improve sleep in children with ADHD and adults with mild insomnia | [21, 22, 23] |
| Carbocysteine and N-acetylcysteine | These antioxidants may modestly improve sleep for some sleep apnea patients | [24, 25] |
Mixed Evidence of Benefit
| Sleep Supplement | What the Research Says | Citations |
| Vitamin D | In one study, high vitamin D supplements improved sleep parameters in 20-50 year olds with sleep disorders. However, the opposite occurred in postmenopausal women with low circulating vitamin D. | [26, 27] |
| GABA | This may help people fall asleep but not stay asleep past the early sleep stages. | [28] |
| Valerian | Supplements containing whole valerian root may improve insomnia. However, valerian herbal extracts, due to inconsistencies in their active ingredients, may not be so effective. Side effects, such as diarrhea, or next day sleepiness, may occur. | [29, 30] |
| Multivitamins | Multivitamins improved sleep disorders in women with chronic fatigue syndrome. But high-dose, B complex supplements taken late in the day may disrupt sleep quality. | [31, 32] |
| Magnesium | Although clinical research of magnesium as a treatment for insomnia is fairly sparse, it shows a clear trend toward magnesium being helpful. Plus, it’s safe and inexpensive, so may be worth trying, especially given that mild magnesium deficiency is common. | [33, 34] |
Why Sleep Is So Important
Sleep should always be a high priority when working to improve your wellbeing. Sleep prepares your brain for the day ahead and is vital for:
- Mental functioning: Optimizing your ability to learn and assimilate information
- Emotional wellbeing: Helping with your ability to control anger and mood swings
- Physical safety: Ensuring you are alert enough to drive or operate machinery

If you are sleep deficient or have other sleep problems it can cause chronic health issues over the longer term. For example, it can increase the risk of [1]:
- Heart disease and stroke
- Kidney disease
- High blood pressure
- Diabetes
- Obesity
- Immune system dysfunction
The Connection Between Sleep and Your Gut
Restful sleep can often be more elusive because of what is happening in your gut. That’s because imbalances in your gut bacteria have far-reaching effects that can extend to disturbances in your sleep cycle.
Research indicates that the connection between your gut health and sleep works both ways. Gut dysbiosis (microbial imbalance) and inflammation can worsen sleep, while poor sleeping patterns can also worsen gut issues.
For example, in a healthy gut, the microbiota influence normal sleep patterns by helping create chemical messengers, such as serotonin and dopamine in the brain. When mice are given antibiotics that destroy their gut flora, the result is disrupted sleep [35].
There’s also evidence that when our circadian rhythm — the 24-hour biological cycle that plays a major role in healthy sleep — gets out of whack, levels of the sleep hormone melatonin fall, and this affects the ability of the intestinal wall to act as an effective barrier to bacteria and toxins (i.e. the gut becomes more “leaky”) [36].
This can all add up to significant sleep issues for people with gut issues. For example, one review found that sleep disorders occurred at the rate of 37.5% of irritable bowel syndrome (IBS) patients, which is higher than in the general population [37].
Steps for a Better Night’s Sleep
Good habits are key when it comes to getting your zzzs, and even more so if you have gut imbalances that could affect your sleep. Keeping a nightly routine that’s as consistent as possible is helpful, but should be underpinned with a healthy diet and lifestyle, and creating a sleep-friendly environment around you.
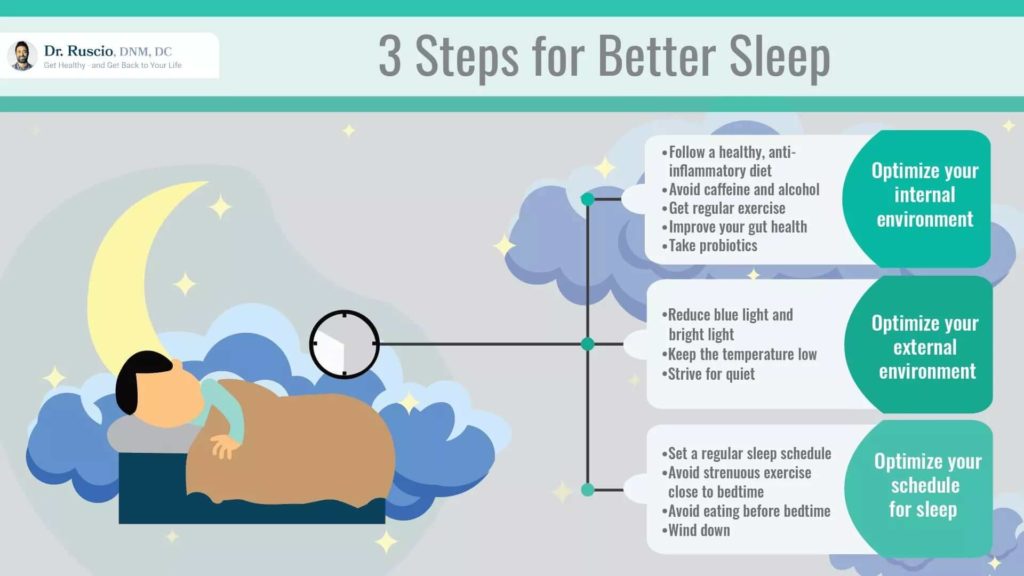
Adopt a Healthy Diet and Lifestyle
- Eat a nutrient-rich diet. Managing weight through healthy diet and exercise has been shown to help in sleep disorders including obstructive sleep apnea [38, 39]. A healthy diet, such as the Mediterranean diet, or a paleo-style diet, will also help improve imbalances associated with impaired sleep, such as inflammation, poor gut health, and hormonal disruptions.
- Ease up on caffeine and alcohol. Both of these can disrupt restful sleep and contribute to insomnia [40]. Aim to avoid caffeinated drinks beyond early afternoon and stick to no more than one small alcoholic drink a day.
- Be physically active. A systematic review of three meta-analyses found that regular exercise helps adults to sleep an average of 19% better overall [41].
Create a Sleep-Friendly Environment
- Power down screens before bed. When you’re exposed to blue light from tablets and cellphones at night, that blue light tricks your brain into thinking it’s daytime. As a result, production of the sleep hormone melatonin is suppressed and works to make you stay awake [42, 43]. Sleep masks and/or blackout curtains can help to keep your environment dark at night.
- Check the temperature of your bedroom. The best temperature for good sleep is around (19–21 C / 66–70 F) for most people [44]. However, you may need to experiment to find the perfect temperature for you. One clinical trial found that people with obstructive sleep apnea did better in warmer environments [45].
- Dial down the noise. A quiet environment avoids your sleep being disrupted [46]. If nighttime noise is unavoidable where you live, try using earplugs or a white noise generator.
Follow a Consistent Nightly Routine
- Set a regular sleep schedule. Try to go to bed and wake up at the same time every day. If you’re a shift worker, this won’t be possible, but you can help by keeping the lights bright while you work, taking naps, and trying to limit shift changes so your body clock can adjust [1].
- Have a calming pre-bed routine. Adopt relaxing rituals, such as reading or taking a warm bath in the half hour to an hour before sleep (and remember, no screens!). Also avoid eating or exercising immediately before bed [1, 47].
- Shoot for seven hours sleep. This is the consensus recommendation of the American Academy of Sleep Medicine and Sleep Research Society [48]. A sleep tracker, such as the Oura ring, can be very useful to help you track sleep-wake cycles and sleep stages and ultimately improve your sleep hygiene [49].
Could You Have Obstructive Sleep Apnea?
Some people have breathing difficulties that cause much diminished sleep quality.
Obstructive sleep apnea occurs when the upper airway becomes blocked repeatedly during sleep and is more common in people who are obese.
If you have sleep apnea, your sleep suffers because you frequently wake up for a few seconds to gasp for air. However, you may not actually be conscious of this [50]. A partner may comment that you’re snoring particularly loudly or notice that you stop breathing briefly before rousing during sleep [51].
Your healthcare provider may suggest sleep studies to diagnose sleep apnea, but another option to consider is an at-home sleep apnea test with a portable device like the WatchPAT. This technique is easier than clinical sleep studies and can help you to identify sleep issues from the comfort of your home.
A breathing device known as a continuous positive air pressure (CPAP) machine is the usual medical treatment for severe cases of sleep apnea. But there’s another much less invasive therapy called myofunctional therapy, which works for many patients.
Myofunctional Therapy and Sleep Quality
Myofunctional therapy is a set of physical therapy exercises of the mouth that improve bite, breathing, and facial posture and can also improve sleep quality in people with sleep apnea. For example:
- A 2020 systematic review of clinical trials concluded myofunctional therapy would likely reduce daytime sleepiness and increased sleep quality over the short term [52].
- Another systematic review and meta-analysis found that myofunctional therapy decreased obstructive apnea episodes by approximately 50% in adults. The therapy also improved low oxygen saturation, snoring, and sleepiness [53].
When working with patients who have obstructive sleep apnea and breathing disorders that affect sleep, I’ve found that referring them for myofunctional therapy can often be very helpful and allow people to avoid CPAP.
The Bottom Line on Sleep and Sleep Vitamins
Sleep is vitally important to every aspect of health and wellness. Sleep vitamins, in association with a gut-healthy diet, probiotics and good lifestyle habits, can help to get your sleep habits back on track.
Melatonin is among the best studied sleep supplements and can have a good effect on sleep quality. Other sleep vitamins, including herbals like lemon balm and passionflower may also be helpful.
My book, Healthy Gut, Healthy You, explains more about sleep and how it factors into your gut health and overall health. For more individualized guidance and support, including having an at-home sleep test, or being referred to a reputable myofunctional practitioner, request a consultation at my functional medicine center.
Dr. Michael Ruscio is a DC, natural health provider, researcher, and clinician. He serves as an Adjunct Professor at the University of Bridgeport and has published numerous papers in scientific journals as well as the book Healthy Gut, Healthy You. He also founded the Ruscio Institute of Functional Health, where he helps patients with a wide range of GI conditions and serves as the Head of Research.➕ References
- Sleep Deprivation and Deficiency | NHLBI, NIH [Internet]. [cited 2021 Sep 27]. Available from: https://www.nhlbi.nih.gov/health-topics/sleep-deprivation-and-deficiency
- Brown GM, Pandi-Perumal SR, Trakht I, Cardinali DP. Melatonin and its relevance to jet lag. Travel Med Infect Dis. 2009 Mar;7(2):69–81. DOI: 10.1016/j.tmaid.2008.09.004. PMID: 19237140.
- Anderson G, Maes M. Gut dysbiosis dysregulates central and systemic homeostasis via suboptimal mitochondrial function: assessment, treatment and classification implications. Curr Top Med Chem. 2020;20(7):524–39. DOI: 10.2174/1568026620666200131094445. PMID: 32003689.
- Ferracioli-Oda E, Qawasmi A, Bloch MH. Meta-analysis: melatonin for the treatment of primary sleep disorders. PLoS ONE. 2013 May 17;8(5):e63773. DOI: 10.1371/journal.pone.0063773. PMID: 23691095. PMCID: PMC3656905.
- Auld F, Maschauer EL, Morrison I, Skene DJ, Riha RL. Evidence for the efficacy of melatonin in the treatment of primary adult sleep disorders. Sleep Med Rev. 2017 Aug;34:10–22. DOI: 10.1016/j.smrv.2016.06.005. PMID: 28648359.
- McDonagh MS, Holmes R, Hsu F. Pharmacologic treatments for sleep disorders in children: A systematic review. J Child Neurol. 2019 Apr;34(5):237–47. DOI: 10.1177/0883073818821030. PMID: 30674203.
- Yi M, Wang S, Wu T, Zhang X, Jiang L, Fang X. Effects of exogenous melatonin on sleep quality and menopausal symptoms in menopausal women: a systematic review and meta-analysis of randomized controlled trials. Menopause. 2021 Mar 26;28(6):717–25. DOI: 10.1097/GME.0000000000001757. PMID: 33784263.
- McCleery, Sharpley J Ann L. Pharmacotherapies for sleep disturbances in dementia. Cochrane Database Syst Rev. 2020 Nov 15 [cited 2021 Sep 17];11(11). DOI: 10.1002/14651858.CD009178.pub4. PMID: 33189083. PMCID: PMC8094738.
- Savage RA, Miller J-MM. Melatonin. In: StatPearls. Treasure Island (FL): StatPearls Publishing; 2018. PMID: 30521244.
- Takada M, Nishida K, Gondo Y, Kikuchi-Hayakawa H, Ishikawa H, Suda K, et al. Beneficial effects of Lactobacillus casei strain Shirota on academic stress-induced sleep disturbance in healthy adults: a double-blind, randomised, placebo-controlled trial. Benef Microbes. 2017 Apr 26;8(2):153–62. DOI: 10.3920/BM2016.0150. PMID: 28443383.
- Marotta A, Sarno E, Del Casale A, Pane M, Mogna L, Amoruso A, et al. Effects of probiotics on cognitive reactivity, mood, and sleep quality. Front Psychiatry. 2019 Mar 27;10:164. DOI: 10.3389/fpsyt.2019.00164. PMID: 30971965. PMCID: PMC6445894.
- Romijn AR, Rucklidge JJ, Kuijer RG, Frampton C. A double-blind, randomized, placebo-controlled trial of Lactobacillus helveticus and Bifidobacterium longum for the symptoms of depression. Aust N Z J Psychiatry. 2017 Aug;51(8):810–21. DOI: 10.1177/0004867416686694. PMID: 28068788. PMCID: PMC5518919.
- Nakakita Y, Tsuchimoto N, Takata Y, Nakamura T. Effect of dietary heat-killed Lactobacillus brevis SBC8803 (SBL88TM) on sleep: a non-randomised, double blind, placebo-controlled, and crossover pilot study. Benef Microbes. 2016 Sep;7(4):501–9. DOI: 10.3920/BM2015.0118. PMID: 27013460.
- Smith RP, Easson C, Lyle SM, Kapoor R, Donnelly CP, Davidson EJ, et al. Gut microbiome diversity is associated with sleep physiology in humans. PLoS ONE. 2019 Oct 7;14(10):e0222394. DOI: 10.1371/journal.pone.0222394. PMID: 31589627. PMCID: PMC6779243.
- Lee J, Jung H-Y, Lee SI, Choi JH, Kim S-G. Effects of Passiflora incarnata Linnaeus on polysomnographic sleep parameters in subjects with insomnia disorder: a double-blind randomized placebo-controlled study. Int Clin Psychopharmacol. 2020 Jan;35(1):29–35. DOI: 10.1097/YIC.0000000000000291. PMID: 31714321.
- Maroo N, Hazra A, Das T. Efficacy and safety of a polyherbal sedative-hypnotic formulation NSF-3 in primary insomnia in comparison to zolpidem: a randomized controlled trial. Indian J Pharmacol. 2013 Feb;45(1):34–9. DOI: 10.4103/0253-7613.106432. PMID: 23543804. PMCID: PMC3608291.
- Haybar H, Javid AZ, Haghighizadeh MH, Valizadeh E, Mohaghegh SM, Mohammadzadeh A. The effects of Melissa officinalis supplementation on depression, anxiety, stress, and sleep disorder in patients with chronic stable angina. Clin Nutr ESPEN. 2018 Aug;26:47–52. DOI: 10.1016/j.clnesp.2018.04.015. PMID: 29908682.
- Taavoni S, Nazem Ekbatani N, Haghani H. Valerian/lemon balm use for sleep disorders during menopause. Complement Ther Clin Pract. 2013 Nov;19(4):193–6. DOI: 10.1016/j.ctcp.2013.07.002. PMID: 24199972.
- van Dalfsen JH, Markus CR. Interaction between 5-HTTLPR genotype and cognitive stress vulnerability on sleep quality: effects of sub-chronic tryptophan administration. Int J Neuropsychopharmacol. 2015 Feb 2;18(3). DOI: 10.1093/ijnp/pyu057. PMID: 25644221. PMCID: PMC4360245.
- van Dalfsen JH, Markus CR. The serotonin transporter gene-linked polymorphic region (5-HTTLPR) and the sleep-promoting effects of tryptophan: A randomized placebo-controlled crossover study. J Psychopharmacol (Oxford). 2019 Aug;33(8):948–54. DOI: 10.1177/0269881119855978. PMID: 31237183. PMCID: PMC6628462.
- Lyon MR, Kapoor MP, Juneja LR. The effects of L-theanine (Suntheanine®) on objective sleep quality in boys with attention deficit hyperactivity disorder (ADHD): a randomized, double-blind, placebo-controlled clinical trial. Altern Med Rev. 2011 Dec;16(4):348–54. PMID: 22214254.
- Sarris J, Byrne GJ, Cribb L, Oliver G, Murphy J, Macdonald P, et al. L-theanine in the adjunctive treatment of generalized anxiety disorder: A double-blind, randomised, placebo-controlled trial. J Psychiatr Res. 2019 Mar;110:31–7. DOI: 10.1016/j.jpsychires.2018.12.014. PMID: 30580081.
- Hidese S, Ogawa S, Ota M, Ishida I, Yasukawa Z, Ozeki M, et al. Effects of L-Theanine Administration on Stress-Related Symptoms and Cognitive Functions in Healthy Adults: A Randomized Controlled Trial. Nutrients. 2019 Oct 3;11(10). DOI: 10.3390/nu11102362. PMID: 31623400. PMCID: PMC6836118.
- Wu K, Su X, Li G, Zhang N. Antioxidant carbocysteine treatment in obstructive sleep apnea syndrome: A randomized clinical trial. PLoS ONE. 2016 Feb 5;11(2):e0148519. DOI: 10.1371/journal.pone.0148519. PMID: 26849119. PMCID: PMC4743936.
- Sadasivam K, Patial K, Vijayan VK, Ravi K. Anti-oxidant treatment in obstructive sleep apnoea syndrome. Indian J Chest Dis Allied Sci. 2011 Sep;53(3):153–62. PMID: 21838198.
- Majid MS, Ahmad HS, Bizhan H, Hosein HZM, Mohammad A. The effect of vitamin D supplement on the score and quality of sleep in 20-50 year-old people with sleep disorders compared with control group. Nutr Neurosci. 2018 Sep;21(7):511–9. DOI: 10.1080/1028415X.2017.1317395. PMID: 28475473.
- Mason C, de Dieu Tapsoba J, Duggan C, Wang C-Y, Korde L, McTiernan A. Repletion of vitamin D associated with deterioration of sleep quality among postmenopausal women. Prev Med. 2016 Dec;93:166–70. DOI: 10.1016/j.ypmed.2016.09.035. PMID: 27687537. PMCID: PMC5118122.
- Hepsomali P, Groeger JA, Nishihira J, Scholey A. Effects of Oral Gamma-Aminobutyric Acid (GABA) Administration on Stress and Sleep in Humans: A Systematic Review. Front Neurosci. 2020 Sep 17;14:923. DOI: 10.3389/fnins.2020.00923. PMID: 33041752. PMCID: PMC7527439.
- Shinjyo N, Waddell G, Green J. Valerian Root in Treating Sleep Problems and Associated Disorders-A Systematic Review and Meta-Analysis. J Evid Based Integr Med. 2020 Dec;25:2515690X20967323. DOI: 10.1177/2515690X20967323. PMID: 33086877. PMCID: PMC7585905.
- Leach MJ, Page AT. Herbal medicine for insomnia: A systematic review and meta-analysis. Sleep Med Rev. 2015 Dec;24:1–12. DOI: 10.1016/j.smrv.2014.12.003. PMID: 25644982.
- Maric D, Brkic S, Tomic S, Novakov Mikic A, Cebovic T, Turkulov V. Multivitamin mineral supplementation in patients with chronic fatigue syndrome. Med Sci Monit. 2014 Jan 14;20:47–53. DOI: 10.12659/MSM.889333. PMID: 24419360. PMCID: PMC3907507.
- Aspy DJ, Madden NA, Delfabbro P. Effects of vitamin B6 (pyridoxine) and a B complex preparation on dreaming and sleep. Percept Mot Skills. 2018 Jun;125(3):451–62. DOI: 10.1177/0031512518770326. PMID: 29665762.
- Mah J, Pitre T. Oral magnesium supplementation for insomnia in older adults: a Systematic Review & Meta-Analysis. BMC Complement Med Ther. 2021 Apr 17;21(1):125. DOI: 10.1186/s12906-021-03297-z. PMID: 33865376. PMCID: PMC8053283.
- Rosanoff A, Weaver CM, Rude RK. Suboptimal magnesium status in the United States: are the health consequences underestimated? Nutr Rev. 2012 Mar;70(3):153–64. DOI: 10.1111/j.1753-4887.2011.00465.x. PMID: 22364157.
- Ogawa Y, Miyoshi C, Obana N, Yajima K, Hotta-Hirashima N, Ikkyu A, et al. Gut microbiota depletion by chronic antibiotic treatment alters the sleep/wake architecture and sleep EEG power spectra in mice. Sci Rep. 2020 Nov 11;10(1):19554. DOI: 10.1038/s41598-020-76562-9. PMID: 33177599. PMCID: PMC7659342.
- Swanson GR, Gorenz A, Shaikh M, Desai V, Forsyth C, Fogg L, et al. Decreased melatonin secretion is associated with increased intestinal permeability and marker of endotoxemia in alcoholics. Am J Physiol Gastrointest Liver Physiol. 2015 Jun 15;308(12):G1004-11. DOI: 10.1152/ajpgi.00002.2015. PMID: 25907689. PMCID: PMC4469868.
- Wang B, Duan R, Duan L. Prevalence of sleep disorder in irritable bowel syndrome: A systematic review with meta-analysis. Saudi J Gastroenterol. 2018 Jun;24(3):141–50. DOI: 10.4103/sjg.SJG_603_17. PMID: 29652034. PMCID: PMC5985632.
- Carneiro-Barrera A, Díaz-Román A, Guillén-Riquelme A, Buela-Casal G. Weight loss and lifestyle interventions for obstructive sleep apnoea in adults: Systematic review and meta-analysis. Obes Rev. 2019 May;20(5):750–62. DOI: 10.1111/obr.12824. PMID: 30609450.
- Edwards BA, Bristow C, O’Driscoll DM, Wong A-M, Ghazi L, Davidson ZE, et al. Assessing the impact of diet, exercise and the combination of the two as a treatment for OSA: A systematic review and meta-analysis. Respirology. 2019 Aug;24(8):740–51. DOI: 10.1111/resp.13580. PMID: 31116901.
- Karna B, Gupta V. Sleep Disorder. In: StatPearls. Treasure Island (FL): StatPearls Publishing; 2021. PMID: 32809555.
- Kelley GA, Kelley KS. Exercise and sleep: a systematic review of previous meta-analyses. J Evid Based Med. 2017 Feb;10(1):26–36. DOI: 10.1111/jebm.12236. PMID: 28276627. PMCID: PMC5527334.
- Lockley SW, Brainard GC, Czeisler CA. High sensitivity of the human circadian melatonin rhythm to resetting by short wavelength light. J Clin Endocrinol Metab. 2003 Sep;88(9):4502–5. DOI: 10.1210/jc.2003-030570. PMID: 12970330.
- Burgess HJ, Molina TA. Home lighting before usual bedtime impacts circadian timing: a field study. Photochem Photobiol. 2014 Jun;90(3):723–6. DOI: 10.1111/php.12241. PMID: 24918238. PMCID: PMC4053688.
- Harding EC, Franks NP, Wisden W. The temperature dependence of sleep. Front Neurosci. 2019 Apr 24;13:336. DOI: 10.3389/fnins.2019.00336. PMID: 31105512. PMCID: PMC6491889.
- Valham F, Sahlin C, Stenlund H, Franklin KA. Ambient temperature and obstructive sleep apnea: effects on sleep, sleep apnea, and morning alertness. Sleep. 2012 Apr 1;35(4):513–7. DOI: 10.5665/sleep.1736. PMID: 22467989. PMCID: PMC3296793.
- Schmidt F, Kolle K, Kreuder K, Schnorbus B, Wild P, Hechtner M, et al. Nighttime aircraft noise impairs endothelial function and increases blood pressure in patients with or at high risk for coronary artery disease. Clin Res Cardiol. 2015 Jan;104(1):23–30. DOI: 10.1007/s00392-014-0751-x. PMID: 25145323. PMCID: PMC4300412.
- Stutz J, Eiholzer R, Spengler CM. Effects of Evening Exercise on Sleep in Healthy Participants: A Systematic Review and Meta-Analysis. Sports Med. 2019 Feb;49(2):269–87. DOI: 10.1007/s40279-018-1015-0. PMID: 30374942.
- Consensus Conference Panel, Watson NF, Badr MS, Belenky G, Bliwise DL, Buxton OM, et al. Recommended amount of sleep for a healthy adult: A joint consensus statement of the american academy of sleep medicine and sleep research society. J Clin Sleep Med. 2015 Jun 15;11(6):591–2. DOI: 10.5664/jcsm.4758. PMID: 25979105. PMCID: PMC4442216.
- de Zambotti M, Rosas L, Colrain IM, Baker FC. The sleep of the ring: comparison of the ŌURA sleep tracker against polysomnography. Behav Sleep Med. 2019 Apr;17(2):124–36. DOI: 10.1080/15402002.2017.1300587. PMID: 28323455. PMCID: PMC6095823.
- Sleep Apnea | NHLBI, NIH [Internet]. [cited 2021 Sep 28]. Available from: https://www.nhlbi.nih.gov/health-topics/sleep-apnea
- Sleep apnea – Symptoms and causes – Mayo Clinic [Internet]. [cited 2021 Sep 28]. Available from: https://www.mayoclinic.org/diseases-conditions/sleep-apnea/symptoms-causes/syc-20377631
- Rueda J-R, Mugueta-Aguinaga I, Vilaró J, Rueda-Etxebarria M. Myofunctional therapy (oropharyngeal exercises) for obstructive sleep apnoea. Cochrane Database Syst Rev. 2020 Nov 3;11:CD013449. DOI: 10.1002/14651858.CD013449.pub2. PMID: 33141943. PMCID: PMC8094400.
- Camacho M, Certal V, Abdullatif J, Zaghi S, Ruoff CM, Capasso R, et al. Myofunctional Therapy to Treat Obstructive Sleep Apnea: A Systematic Review and Meta-analysis. Sleep. 2015 May 1;38(5):669–75. DOI: 10.5665/sleep.4652. PMID: 25348130. PMCID: PMC4402674.
Discussion
I care about answering your questions and sharing my knowledge with you. Leave a comment or connect with me on social media asking any health question you may have and I just might incorporate it into our next listener questions podcast episode just for you!