Sleep Effects EVERYTHING – Crucial Info for Children & Adults
Special retainer can improve breathing & sleep with Dr. Kevin Boyd.
Without high-quality sleep, we are susceptible to a wide array of health problems. Pediatric dentist Dr. Kevin Boyd is on a mission to improve sleep and breathing in children, by using dentistry and orthodontia to treat their teeth and jaws as early as possible. In our conversation, you’ll hear why and how to intervene if you suspect issues for your child, and some options to explore for adults.
Episode Intro
Dr. Michael Ruscio, DC: Hi everyone. Welcome to Dr. Ruscio Radio. This is Dr. Ruscio. Today, I’m here with Dr. Kevin Boyd and we are going to be talking about, the importance of the development of your children’s teeth and their jaw and a different way that we could approach treating some of these imbalances that may be addressed by conventional dentistry and braces and the like. So, Kevin, welcome to the show and thank you for being here today.
[Continue reading below]
Signs for Children
- Parents or family members have signs
- Behavioral
- Snoring
- Excessive movement
- Sweating
- Grinding teeth
- Sleeping with mouth open
- Physical
- Dental facial respiratory
- Narrow jaw or too far back, cross bite, underbite
- Tongue tie, Lip tie
- Birth history
- Premature
- Low birth weight
- Second hand or primary smoke
Signs for Adults
- Molars removed
- Headgear as child
- Sleep apnea
- Snoring
- Headaches, Migraines, TMJ
Where to go to get help
- About 10 doctors throughout the country that are well equipped to treat these issues
- For adults: Dr. Jeffrey Rouse DDS – General Dentist, San Antonio TX
- For children: Dr. Kevin Boyd – Board-Certified Pediatric Dentist, Chicago
- Email: kbo569@gmail.com
- Premier Sleep – Steve Carstensen, DDS, Seattle
- Face Focused – Dr. William M. Hang, DDS, Los Angeles
- RCIO: Raphael Center for Integrative Orthodontics
Treatment
- Simple, retainer like, device
More from you
- Medium article – Our Skulls Are Out-Evolving Us
- Dr. Kevin’s email: kbo569@gmail.com phone:312-988-9855
Where to learn more:
References and Resources
- The Relief of Nasal Obstruction
- Enlargement of Nasal Sinuses in Young Children
- Orthodontia in its Relation To Rhinology
- Persistent Mouth Breathing Following Adenoidectomies
- Rhinology and its Relation to Orthodontia
- The Relations of The Dental Arches to Pathologic Affections of the Nasopharynx and Adjacent Parts
- Malocclusion and its Far Reaching Effects
- Randomized Controlled Trials vs. Observational Studies – Why Not Just Live Together
- Some Points of Common Interest to The Rhinologist and The Orthodontist
- The Mutual Development of Upper Air Tract Jaws Teeth and Face and Their Economic Importance to the Human Race
In this episode…
Episode Intro … 00:00:40
Orthodontic Expansion … 00:02:26
Signs & Symptoms … 00:8:50
Where to Find Help … 00:18:57
Episode Wrap-up … 00:28:49
Download this Episode (right click link and ‘Save As’)
Dr. Kevin Boyd: Great. I’m happy to be here and share this message with you.

DrMR: Tell us a little bit about that message. Tell people what it is you do, and then we can go from there in terms of elaborating on why that’s important.
DrKB: About 10 – 12 years ago I was approached by Dr. Steven Sheldon, the chief of pediatric sleep medicine at Lurie Children’s Hospital in Chicago it was called Children’s Memorial back then, with a proposal. He knew that as a pediatric dentist who did mostly orthodontics on children under the age of seven, I was really in a good position to help him raise awareness about sleep apnea and those children who were sent to him for sleep studies and recommendations for surgery to take out their tonsils and adenoids, as well as using steroids to maybe shrink the tonsils.
Orthodontic Expansion
He had heard about the work that we do in terms of orthodontic expansion in kids as young as two and a half years old, and that as a result their sleep and breathing was improved. What he wanted to do is take me and some other dentists to the medical school at St. Louis University and train us intensely over the course of a three-day weekend on doing sleep and breathing disorders assessments in terms of how they teach it to medical students and how they teach it to pediatricians.
He thought that many of the risk factors, such as narrow and backward jaws that aren’t growing correctly in children as young as two, three and four years old, along with showing signs of crooked teeth and crossbites, would be identified by dentists. And knowing that those risk factors are coexistent with sleep and breathing problems, that maybe by fixing those things earlier than a typical orthodontist would, say at age 10 or 11, we could prevent a lot of breathing problems.
So, we put together a protocol and got Institutional Review Board (IRB) exemption. The evidence that we produced to the IRB Committee was so compelling, they said we didn’t need approval.
DrMR: Just for the audience. The IRB, they’re essentially the ethics board that approves any kind of interventional study in humans.
DrKB: That was almost unprecedented. We have been creating data over the course of almost 12 years now, which is currently being analyzed by three orthodontic residents from Boston University and a PhD candidate in anthropology from the University of Arkansas.
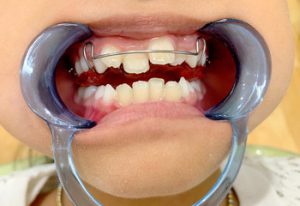
What we are finding is when you help a child have room for their tongue, meaning you make room for their tongue by using conventional orthodontic expanders, at earlier ages than is typical, it makes a world of difference. Occasionally you will see a younger child, while they still have their baby teeth, get a maxillary upper jaw expander if they have a crossbite. But if they don’t have a crossbite, typically orthodontists leave them alone until they’re 10 or 11.
And while we are waiting for that child to reach age 10 or 11, all kinds of problems can happen with their inability to have room to put their tongue up on the roof of the mouth so they can sleep and breathe through their nose. It really changed a lot of feeling about when a child should first get orthodontic evaluation and treatment when indicated.
DrMR: And so sorry. So the basic premise here it sounds like is when a child doesn’t have adequate room in their mouth and there’s crowding, and that includes crowding of the teeth and crowding of the tongue, you can intervene earlier opening up the dental arch and the airway and preemptively stop a child from having breathing problems. Is that a fair general summation?
DrKB: You can preempt it, or you can reverse it. We have a lot of kids coming to us that already have sleep and breathing problems. We want to intervene at the earliest age as is feasible. Now as a pediatric dentist, the earliest age that might be feasible could be as young as two years old. But if a kid moves to Chicago from Seattle and he’s 12 and I’m the first person to recognize that his malocclusion might be coincident with sleep and breathing problems, well then 12 is the earliest age that’s feasible.

This goes for adults as well. I’m an adult and I’m going to be getting treatment from an orthodontist in Arkansas, Dr. Richard Roblee, with something called SFOT (Surgically Facilitated Orthodontic Therapy) that will widen my jaw and bring things forward. I have sleep apnea as a result of my malocclusion, not weight. I had premolars extracted in the ’60s and I had to wear head gear. Again, I’m not overweight but I have apnea as if I weighed 400 pounds all as a result of the shape of my jaw. This could have been prevented when I was a kid, but they didn’t know that then. The orthodontic profession is just now starting to get curious about this.
DrMR: What are some of the signs? I’m if we have probably two different audiences thinking about this. The adults thinking about it for themselves and the adults thinking about this for their children.
For the non-dentists, what are some simple things that help to identify this issue? Of course, if there’s a diagnosed sleep apnea, that can give one indication, but what are some of the telltale signs that someone might want to get themselves to a professional to have a closer look at this?
DrKB: Well, first, what you said about the audience makeup. If you’re a dentist treating adults or if you’re a physician who mostly sees adults and if they have sleep and breathing problems, the adults, they also might have children, grandchildren, nieces or nephews that are predisposed genetically.
Signs and Symptoms
So right away, everyone has a stake in this. The signs to look for in children include behavioral signs, physical signs, and birth history signals that might suggest that a child is at risk for future airway disease or might already have the physical signs or what we call dental facial respiratory. That means that the jaws and teeth are intimately connected to the respiratory apparatus. We say the back of the face is the airway, the front of the airway is the face. So if a child has a narrow jaw or a jaw that’s too far back, upper and/or lower jaw, if they have what’s called crossbite, if they have underbites, as young as two, three years old where there is no space between their baby teeth, the palate, the roof of the mouth is high and narrow, if they have tongue tie, lip tie…
I won’t go through them all. These are all things that any dentist who sees children can recognize these factors, these physical factors. Then there’s behavioral factors such as snoring, which is never normal for a child. Excessive movement during sleep, not normal for a child. Sweating, grinding their teeth, sleeping with their mouth open, difficulty in waking up in the morning.
These are all factors that track with risk for future sleep apnea or existing disease.
The third component is birth history. If a child is born prematurely, low birth weight, or is around secondhand or primary smoke, meaning a mother either breathe in secondhand smoke or is smoking herself. These are all things that put a child at high risk for having sleep apnea when they’re in early childhood, infancy and toddlerhood, preschool age. The orthodontic profession has it all wrong and they don’t want to see your kid till age seven for their first evaluation. Age seven is a geriatric patient in my pediatric practice. I want to see these kids by age one. We can pick up signs that a kid might be at risk at that stage.
DrMR: I tend to agree with you.
Sponsored Resources
Hi, everyone. Let’s talk about probiotics, which helped to make this podcast possible. Functional Medicine Formulations contains a line of probiotics that I personally developed, and I’m super excited to be able to offer you the same probiotics that I’ve been using in the clinic for years and are a byproduct of an extensive review of the literature plus my own clinical experience.

In this line, you will find my favorite three probiotics in all three of the main categories that work synergistically to help you fight dysbiosis, like SIBO, candida yeast, and H. pylori, help to eradicate parasites, help to reduce leaky gut and repair the gut barrier, and can improve gas, bloating, diarrhea, constipation, and may even improve mood, skin, sleep, and thyroid function because of the far-reaching impact of the gut. You can learn more about these at drruscio.com/probiotics.
DrMR: From what I know about this area, it does seem the most intelligent to intervene early and try to correct a problem that is due to a narrowed formation. Try to open rather than restrict. Just as you said, I’m sure there’s plenty of people listening to this who they had crowding of their teeth because the arch wasn’t developed widely enough and so what happened? Teeth were pulled out and then braces and headgear were used to close those teeth together.

That’s one approach. Sure. I guess it’s maybe better than nothing, although that’s arguable. It seems much more of an intelligent endeavor if we can do it, to open that cavity so that we don’t run the risk of these breathing issues that you’re outlining.
DrKB: Mic drop for you here. I can produce literature. I can produce the literature in the medical and dental literature that started shortly after the end of the civil war with physicians and dentists (there were no orthodontists yet) There were physicians doing orthodontics, expanding children’s jaws as young as two and a half years old to help them sleep and breathe better.
I’ve got a stack of literature from the Boston Journal of Medicine and Surgery, which was the precursor to the New England Journal of Medicine , from the Journal of the American Medical Association, from the American Journal of Orthodontics, all these that physicians and dentists were working together to help children breathe better by what they called spreading their arches. They put in these little expanders that were made from vulcanized rubber. It was before acrylic, before x-ray.
I’m going to send you some great articles and if you go online to MEDIUM, it’s an online journal, Medium and read Our Skulls Are Out-Evolving Us. I had an investigative reporter from the Atlantic Monthly follow me for almost a year and a half, with my research at the University of Pennsylvania and in my practice in Chicago, and she published this wonderful article that outlines everything about how this relates to my anthropology research and to my clinical application of it.
DrMR: Well, that’s fantastic. If you have some select articles you want to send over, please do. Our audience is dense with reference buffs and we’ll gladly include those.
Coming back to my comment before about adults. I think you probably hit a few common, historical pieces that adults will have. I myself had crowding, I had molars removed, I had braces, I had headgear. This is something I’m keenly trying to pay attention to. What else? I’m assuming with adults in terms of what other risk factors are there besides those. Of course, if there’s a diagnosed sleep problem or snoring, I’m assuming those same things apply to adults. But tell us a little bit more for the adults in the audience what should they be looking out for.
DrKB: Well, if adult have sleep and breathing problems, but also if they have chronic headaches, have migraines, TMJ, TMD disorder… those are all airway related problems. Worn teeth, periodontics, gum disease that’s related to excessive grinding and tooth wear. Those are all airway problems. The reason these things happen is that there is rhythmic movement of the jaws. There’s clenching and grinding that persists beyond childhood and manifests itself as TMJ disorder.

That’s an airway problem. That is your brain trying to solve the problem by having your jaw shift forward and opening your airway. It might take decades before somebody recognizes it. If you have temporomandibular joint dysfunction, you have an airway problem. That is unequivocal at this point. I don’t really weigh in too much on adults other than the fact that if they’re a first or second order relative of the child, that please be aware that you may be the first person, whether you’re an adult seeing… you’re a dentist seeing adults or you’re a parent is that if you got problems, your kid, your grandkids, your niece or nephew may be predisposed.
Get them to somebody. Pediatric dentists, orthodontists who see kids and general dentists especially. I think general dentists are going to save the world here because pediatric dentists do a lot of great things for kids relative to cavities, but airway is only starting to be recognized as in the purview of a pediatric dentist. They don’t see airway as a component of oral health. General dentists are really stepping up to the plate on this. So, I want to do all I can to help as many general dentists. I invite anybody who’s listening to this. If they want to come and shadow me in Chicago, I will teach you something that is so simple to do and so incredibly impactful on children’s lives and welfare. It ain’t rocket science. It’s just not that difficult to do, but you can’t fear kids. You know, what if they won’t open? You know what? I can teach you that stuff.
I’m a pediatric dentist. I know how to do that. Orthodontists and GPs never have to demonstrate any competence in managing anxiety in children. That’s the big obstacle to why this has not been done the way it was a hundred years ago.
Where to Find Help?
DrMR: Where does someone go? I’m assuming several people in our audience have had their curiosity piqued. Is there a website, an association? Is there a certain training that you look for? They’re looking for a doctor, for a clinician. Where do they go?
DrKB: Well, for one thing, if you’re an adult and you have airway and PMD and malocclusion coexistent, I have people who are competent with adults. There’s about 10 people in the country from the East Coast to the West Coast to the South to the North and Midwest, whatever. Is that there’s people that I have learned they completely understand what’s going on but probably the person in the world, the country, if not the world, his name is Dr. Jeff Rouse. He is a general dentist in San Antonio, Texas. Over the course of about eight or nine years, I’ve come to see him as being probably the number one expert in the world on this in terms of adults and children. He’s a prosthodontist. He said, “The reason I went into prosthodontics, so I would never have to treat a child again.” But when his own kid started showing signs of comorbidity of malocclusion and airway disease, he fixed them because he did all the readings and he knows as much or more about pediatric airway diseases than I do, but he doesn’t treat kids. Before, he had local people he referred kids to Chicago from San Antonio to me. He’s really an expert in this area and he can tell you people he’s trained. In terms of children, I’m sort of becoming right up there with Jeff, but just for kids. Call me, email me. KBO569@gmail.com and I will try to get you matched with somebody in your area or somebody that will listen to me if I can help work your child up or one of your patients up.
This is how we teach. We really try to collaborate with local dentists. The American Dental Association has gotten behind pediatric airway. You may know about the symposia at the ADA, the third one that’s coming up in 2020. The House of Delegates just put thumbs up. They’re going to start funding research in this area. Lots of good things are happening. Dr. Steve Carstensen in Seattle is another veritable expert in pediatrics and adult airway disease. So those are a few really good resources. Also Dr. Bill Hang, an orthodontist in Los Angeles. I took his class and that’s when my life changed. He taught me that if you expanded and protract a four-year-old, you’re going to change their life, you’re going to minimize orthodontic problems down the road and you’re going to improve their airway. I would recommend anybody to do his mini residency. You will learn a ton. There’s other of course, Barry Raphael and Mark Cruz do an Airway Mini-Residency.
DrMR: We’ll make a list in the transcript associated with this post, and my aim will be we’ll list the name and their location so that our audience can look and try to find the doctor who’s closest to them.
View Dr. Ruscio’s Additional Resources
Can you give us a brief on what the treatment looks like? We don’t need to necessarily go into all the details, but I was picturing kind of like a reverse retainer almost. You put it in the arch of your mouth, and it pushes out. Is that kind of the gist?
What Treatment Looks Like
DrKB: It does both. It pushes to the side. The main problem is something called maxillary transverse deficiency. It’s been known about for decades. McNamara is the main academic orthodontist that really published on this back in the 1980s and ’90s, maxillary transverse deficiency, which unfortunately has become synonymous with posterior crossbite, which is nonsense.

That’s like saying a person doesn’t have thinning hair unless he’s bald. It’s gradual. That’s what they’re teaching orthodontic residents and dental residents that a kid’s jaw is okay if they don’t have a crossbite. There are so many kids whose jaws are not right. And if your jaw isn’t right, your airway isn’t right. Virtually, 100% of the time if a three-year-old has something predictable that when he’s older he would benefit from conventional orthodontics and that you can predict it from childhood. A third-year dental student could look at a four-year-old and tell the parents, save up your money for braces. I say that’s like an ophthalmologist looking at a kid at four who has nearsightedness and say, well, you know what, save up your money for glasses because he’s going to need correction when he needs to drive a car at 16.
That’s really a good analogy because when a kid has subtle signs of malocclusion in early childhood, that means that they’re at risk for sleep, breathing and neurological problems now. So that’s why I’m saying it’s medically indefensible to look at a child who has predictable needs for orthodontia at traditional ages of 10, 11, and 12. That means that they’re at risk of sleep, breathing and neurological problems now, and that’s what they understood over a hundred years ago in medicine and dentistry. We’re producing data and the American Dental Association is behind our efforts.
DrMR: I couldn’t agree more. I went through a review of the sleep literature when writing Healthy Gut, Healthy You, and I was astonished at (a) how much literature we have in terms of high quality, large sample size reviews, meta-analyses. I mean pretty much everything I was looking at in terms of sleep disturbances, correlation with obesity, heart disease, Alzheimer’s disease. The data was rife with meta- analyses and they all agreed that anything that compromised sleep leads to increased mortality and morbidity. So yes, anything we can do to improve sleep is hugely important.
DrKB: Well, I’m really encouraged by what you’re seeing and what you’re doing. You know, I admit I just met you but you’re part of this movement in a big way. Do you know Jeff Rouse? Have you heard that name?
DrMR: I don’t, and I’m looking forward to digging a little deeper and trying to provide our audience with resources.
DrKB: Yeah. Look him up. Just get him on this podcast. He’s one of the most knowledgeable people on the planet about this.
Episode Wrap-Up
DrMR: Is there anywhere that you want to point people in terms of your website or any other materials online that you think would be valuable to direct people towards?
DrKB: Well, I think right now just look up that Medium article. It just came out. It’s spectacular. We’ve gotten hundreds of messages from people that want to bring their kids in just for an evaluation from all over the world now.
DrMR: And that title again was?
DrKB: Well, it’s called Our Skulls are Out-Evolving Us. I didn’t make that title up. I probably would’ve put a different title on it, but Katherine Lewis, the reporter from the Atlantic Monthly Magazine, was the person who followed me for over a year. She is a phenomenal reporter and published this online in an online magazine called Medium. It describes everything what we’re doing.
I’ve written three textbook chapters in medical textbooks about this that are, believe it or not, when I write to physicians and dentists in textbooks, I have to do it almost at a high school science level because this material about sleep and breathing and tying anthropology to it. We didn’t get any of this in our dental and medical school training. I’ve learned this over the course of about 12 years, how anthropologists have understood this for decades, what we’re doing. I’ve learned how to communicate that way so that it’s interesting and it’s useful when you read it.

Use my email address and we will make sure that people get this material. It’s KBO569@gmail.com and our office number is area code (312) 988-9855, and my office manager is Orla. She’s got a beautiful Irish accent because she’s from Ireland, and she will send people chapters. If you want to come and shadow us, there’s only one requirement. You must fill out a form that says this is what I want to learn when I come and follow Dr. Boyd. We don’t charge money for it.
And we want to follow up that we’ve met your learning objectives because we’re putting together a three-tiered series of courses through the Academy of Craniofacial Pain and Great Lakes Orthodontics to teach this all over the country and all over the world to get more people competent, at least assessing risk in kids under the age of seven, which is I say the age of seven because age seven is when the AAO, the American Association of Orthodontists says a child should first be seen for orthodontic, and then they don’t treat them till 12. That’s ridiculous. It’s medically indefensible. We just want to train more people to do this. I know you’re on board with this because the way you’re talking and what you’ve learned.
DrMR: I think this is the future and I love the passion. I fully appreciate what you’re doing. If I could go back in time and do my dentistry differently, this is exactly what I would want. I will be pinging my brother to make sure he has my niece and nephew checked out because there’s just, there’s no downside to this. Even if you want to look at it from an aesthetic perspective, your face will look better if you don’t shrink in the lower third.
DrKB: Absolutely. I told you a hundred years ago, they were doing this and one of the attributes that they say, look, if for no other reason, if you want your kids to be as good looking as possible, you must create architecture in their jaws and faces that is conducive to nose breathing. It’s all about nose breathing.

DrMR: For our audience, I mean this is something I’m going to be looking into because we know that oral health, archway health is so important for sleep and sleep is just massively important for your health. I would encourage everyone listening to this or reading this. If any of these things flag for you, reach out to one of the experts that we’ll put in the list associated with the transcript for this episode and get yourself checked out.
Kevin, thank you so much for taking the time. I love what you’re doing. Please keep me abreast of what you have going on and if you ever have an update that you feel worthwhile and you want to come back on, you have an open invitation to come back on whenever you’d like.
DrKB: That’s great. You’re doing a great thing. Come to Chicago. I’d love to meet you some time.
DrMR: Well, Kevin thank you again.
DrKB: Thanks. Good talking to you.
Dr. Michael Ruscio is a DC, natural health provider, researcher, and clinician. He serves as an Adjunct Professor at the University of Bridgeport and has published numerous papers in scientific journals as well as the book Healthy Gut, Healthy You. He also founded the Ruscio Institute of Functional Health, where he helps patients with a wide range of GI conditions and serves as the Head of Research.







Discussion
I care about answering your questions and sharing my knowledge with you. Leave a comment or connect with me on social media asking any health question you may have and I just might incorporate it into our next listener questions podcast episode just for you!