From Bloating to Reflux: Resolving Gastrointestinal Symptoms
Treating Gastrointestinal Symptoms Can be Straightforward
- Common Gastrointestinal Symptoms|
- At a Glance|
- Common Gastrointestinal Disorders and Treatment|
- Gut Support Plan|
- Recommended Products|
If you have been experiencing gastrointestinal symptoms (GI symptoms) like bloating, constipation, diarrhea, or stomach pain, you know how confusing and overwhelming it can be to figure out exactly where your symptoms are coming from and how to resolve them.
Depending on symptoms, a Google search might make it look like you could have dozens of different possible digestive diseases, which can be overwhelming.
In this article, we will try to simplify things for you by providing an overview of common GI symptoms, some common causes, and interventions that can help, even if you do not know the exact cause of your symptoms right away.

Gastrointestinal Symptoms at a Glance
- GI symptoms can include abdominal pain, diarrhea, bloating, weight loss (or gain), heartburn, constipation, or intestinal cramping.
- There are also non-digestive symptoms of digestive illness such as brain fog, fatigue, and joint pain.
- While drastic changes in gastrointestinal symptoms should be checked by a gastroenterologist or other healthcare practitioner, many chronic digestive symptoms can be resolved with a holistic approach to gut healing.
- It is not always necessary to know exactly what is causing your GI symptoms in order to start resolving symptoms with an anti-inflammatory diet, probiotics, and herbal antimicrobials if needed.
We are going to approach this topic in two ways. First, by looking at the most common symptoms one by one, and then by looking at some of the most common reasons for multiple GI symptoms. Each section will include possible causes and the most effective treatment options.
At the end of the article we will review the three steps to supporting gut healing and resolving GI symptoms even if you do not have a diagnosis yet.
Common Gastrointestinal Symptoms and Their Treatments
Some of the most common GI symptoms are constipation, diarrhea, abdominal bloating, reflux, abdominal pain, and nausea. We will review these symptoms below and look at some of the most effective treatments for them.
If you have been experiencing just one symptom, it can be helpful to look at what some of the common causes are and effective treatments.
First let’s look at a quick overview of six of the most common GI symptoms:
1. Constipation
Constipation is a lack of or reduction in bowel movements, or pain or difficulty pooping, with no obvious cause [1]. You may also experience severe lower abdominal pain with constipation.
What causes constipation? Constipation can be caused by functional (due to abnormal functioning of the digestive tract) or non-functional (not caused by abnormal functioning) issues. For example, a functional issue would be if the muscles in your colon do not squeeze and relax like they should, so this slows the colon down causing constipation. A non-functional issue could be constipation due to food sensitivities.
Helpful treatments for constipation:
- Probiotics. Meta-analyses of studies show that multi-strain probiotics (particularly the Lactobacillus or Bifidobacterium strains) reduce intestinal transit time (meaning that the food does not take as long to go through the gastrointestinal tract) and increase frequency of bowel movements [2, 3, 4].
- Soluble fiber. Soluble fiber such as psyllium is often the first recommended intervention for constipation, and it has been shown to be extremely beneficial for some people who have constipation due to IBS [5, 6, 7]. At the same time, some people with IBS need to be careful with fiber, as it can cause bloating, gas, and abdominal pain [5].
- Digestive enzymes. In a double-blind clinical trial, digestive enzymes (enzymes made by the body to help digest specific foods, also available as supplements) were found to double bowel movement frequency, improve stool consistency, and reduce abdominal discomfort, without side effects [8].
2. Diarrhea
This is loose or watery stools. It can be acute (happening for two weeks or less) or chronic (happening for longer than four weeks.)
What causes diarrhea? It can be caused by viral infection or noninfectious conditions [9]. Acute diarrhea is usually caused by viral infection, such as Norovirus, which causes one-fifth of all infectious diarrhea worldwide [9].
Chronic diarrhea, on the other hand, may be caused by malabsorption, inflammatory bowel disease (Crohn’s or ulcerative colitis) [9], leaky gut [10, 11], food sensitivities/intolerances [9, 12], small intestinal bacterial overgrowth (SIBO) [13, 14], bacterial infection H. pylori, or side effects from medications [9].
Helpful treatments for diarrhea:
- Probiotics. A meta-analysis of 82 randomized control trials found that probiotics work to reduce antibiotic-associated diarrhea [15].
- L-glutamine. L-glutamine supplements normalize gut wall integrity in patients with leaky gut and diarrhea-predominant IBS [16].
- Low-FODMAP diet. A 2021 Romanian guidelines for non pharmacological treatment of IBS recommend trying a low FODMAP diet to improve abdominal pain, bloating, and/or diarrhea for a minimum of four weeks [17].
3. Abdominal bloating
This happens when gas accumulates in the intestines, causing a bloating sensation and/or when the abdomen expands. It tends to be uncomfortable and can produce gas [18].
What causes abdominal bloating? Causes are varied and usually associated [19] with a larger digestive disease or issue such as SIBO, IBS or IBD related to food sensitivities.
Helpful treatments for abdominal bloating:
- Probiotics. Probiotics have been shown to be effective in the treatment of IBS, which can cause gas and bloating. They have decreased abdominal bloating in menstruation associated bloating [20, 21].
- Digestive enzymes. These have been shown in multiple studies to significantly improve bloating, gas, and abdominal pain [22, 23].
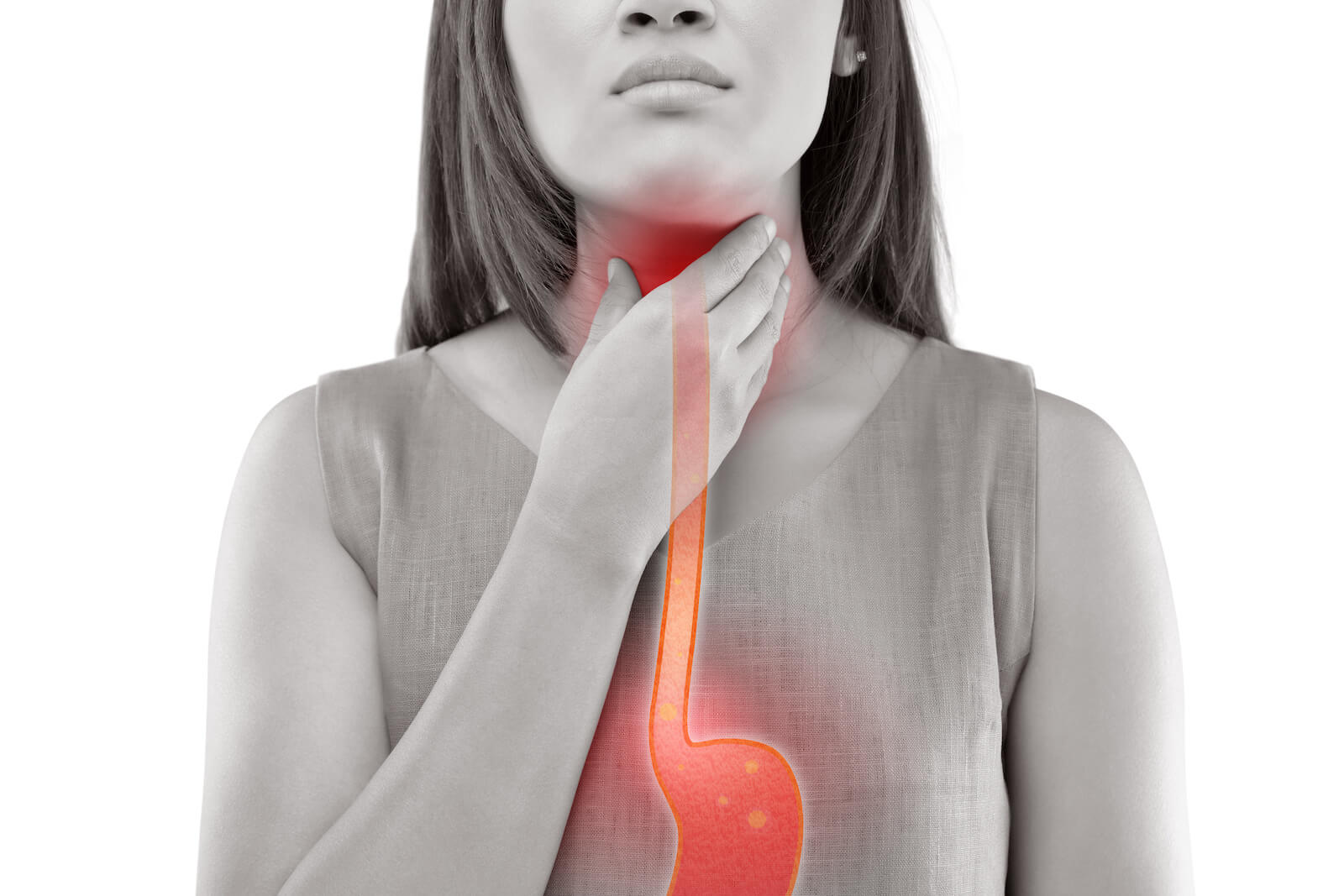
4. Heartburn and Reflux Symptoms
Reflux happens when contents of the stomach, including stomach acid, flow back up into the esophagus and sometimes the throat. Reflux symptoms typically include heartburn and may also include sore throat, coughing, or difficulty swallowing.
What causes reflux? Possible causes of chronic reflux conditions including gastroesophageal reflux disease (GERD) and laryngopharyngeal reflux (LPR or “silent reflux”) include impaired esophageal motility, IBS or SIBO, or hiatal hernias (in which part of the stomach pushes up into the chest) [24, 25].
Helpful treatments for reflux:
- Melatonin. Melatonin is a hormone your body produces each night to stimulate sleep, and it may also help to protect the esophagus for people with GERD and heartburn. It may be as effective as proton pump inhibitors (PPI) for treating GERD [26]. Studies suggest melatonin may be as effective as a PPI for improving GERD [27, 28].
- Probiotics. A recent systematic review of 12 studies found that 79% of the studies reported positive outcomes when GERD was treated with probiotics. These included reduced regurgitation, improvements in reflux, heartburn, indigestion, nausea and gas-related symptoms like burping [29].
5. Abdominal Pain
This is pain in the stomach region or belly, anywhere between your chest and groin area. You may have generalized pain where you feel it in more than half of your abdomen, or localized pain where you feel it in only one spot.
What causes abdominal pain? When it is located in one spot, this is often associated with a problem with an organ like the appendix or gallbladder, cramp-like pain often from gas or diarrhea, or colicky pain, which is severe and comes in waves and more often happens with kidney stones and gallstones [30]. More chronic, generalized abdominal pain may be associated with various digestive disorders including IBS, IBD, and SIBO.
Helpful treatments for abdominal pain:
- Low-FODMAP diet. Two meta-analyses showed that a low-FODMAP diet reduced overall digestive symptoms and abdominal pain and increased quality of life [31, 32].
- Probiotics. These reduce bacterial overgrowth in SIBO, thus diminishing abdominal pain and bloating [33].
- Digestive enzymes. Digestive enzymes have been shown to decrease abdominal bloating and pain [22, 23].
6. Nausea
Nausea is when you feel sick to your stomach. It may or may not lead to vomiting.
What causes nausea? Both nausea and vomiting are defense mechanisms that help us avoid ingesting or digesting toxic substances. They may also be symptoms of a virus. Other chronic causes of nausea may be celiac disease, food sensitivities, gallbladder disease, or gastritis.
Helpful treatments for nausea:
- Intermittent fasting. This is commonly used in cases of nausea and vomiting for any cause. It allows the stomach time to calm and reset and can decrease disease severity. Particularly in IBS, a study with a 10-day fast and five days of re-feeding showed significant improvement in abdominal pain, bloating, diarrhea, nausea, and anxiety [34, 35].
- Probiotics. Probiotics have been shown to help reduce nausea in some cases, including when the nausea is related to GERD [29].
The table below will help you quickly find the symptom you are most interested in and get the information you need. While the list of causes for any one of these symptoms seems overwhelming, you will notice that there is a lot of overlap where one symptom is found in multiple GI disorders. Many of the treatments for the digestive disorders overlap as well. Because of this overlap, it is not always necessary to know exactly what digestive disorder you have in order to start healing your gut and getting relief of symptoms.
After the table, we’ll talk about simple ways to start feeling better.
| Symptom | Likely Causes | Effective Treatments |
| Constipation | Common functional gastrointestinal issues [1]: • Stenosis or strictures in the colon or anus that cause narrowing of the passageways. • Muscular or nerve abnormalities where the nerves that control the stomach and gut or the muscles of the digestive system are not working properly. Common non-functional gastrointestinal issues: • Irritable bowel syndrome (IBS) [36] • Premenstrual syndrome (PMS) [34] and menstruation [37] • Celiac disease and non-celiac gluten sensitivity [1, 12] • Histamine intolerance [38] • Food sensitivities and intolerances (including lactose or casein intolerance) [39] • Too little dietary fiber, not enough water, withholding bowel movements [1] • Metabolic disorders, such as hypothyroidism and type-2 diabetes [1] • Cystic fibrosis, inflammatory bowel disease (IBD), and scleroderma [1] |
Multi-strain probiotics In people with IBS, probiotics, fiber (for some,) and stress reduction (meditation and cognitive behavioral therapy) can be a powerful combination in healing [40, 41, 42]. Digestive enzymes |
| Diarrhea | • Viral infection, such as Norovirus [9] • Bacterial infection, such as Helicobacter pylori [9] • IBS (diarrhea or mixed types) [36] • Lactose intolerance and other food sensitivities/intolerances [43] • Celiac disease and gluten sensitivity [9, 12] • Leaky gut [10, 11] • Chronic pancreatitis and exocrine pancreatic insufficiency (EPI) [44, 45] • Inflammatory bowel disease [9] • Crohn’s and ulcerative colitis often include diarrhea [46, 47, 48] • Antibiotic use and Clostridium difficile [9] • Too much or too little thyroid hormone [49] • Menstruation [37] • Histamine intolerance [38] • Bile acid malabsorption (BAM) [50] • SIBO [13, 14] • Mold illness [51, 52] |
Low-FODMAP diet is helpful if diarrhea is caused by leaky gut and IBS [53, 54]. Probiotics for resolution of leaky gut as well as for use in H. pylori infection. Pancreatic enzyme replacement therapy (PERT) in people who have Exocrine Pancreatic Insufficiency (EPI). 5% of people over the age of 70 and 10% of people over the age of 80 have EPI, which may lead to maldigestion and malabsorption with fatty stools, diarrhea, abdominal pain, and/or weight loss [44, 55]. |
| Abdominal Gas/Bloating | • A bacterial overgrowth (such as SIBO) [18, 56] • Bowel obstruction, renal stones, overeating [18] • IBS and a high fiber diet in many people with IBS • Menstruation • Non-celiac gluten sensitivity, celiac disease [12] • Food sensitivity/intolerance such as lactose intolerance [43, 57, 58, 59, 60] • Atrophic/autoimmune gastritis [61, 62] • Exocrine pancreatic insufficiency (EPI) [44, 45] • (IBD) inflammatory bowel disease [9] |
Probiotics Low-FODMAP diet [53, 54] Digestive enzymes improve bloating, gas, and abdominal pain [22, 23]. |
| Reflux | • Low esophageal motility [25] • Low stomach acid, certain autoimmune diseases, or the long-term use of proton pump inhibitors (PPIs) [63] • Malfunctioning sphincters [25] • Atrophic gastritis [64] • Non-celiac gluten sensitivity [12] • H. pylori, especially in the case of LPR [65] |
Avoiding common trigger foods such as oily, spicy, acidic, and fried foods. Betaine HCl for low stomach acid. Melatonin Probiotics Because of the prevalence of H. pylori infection in LPR, test for and treat with herbal antimicrobials. |
| Abdominal Pain | • IBS, especially in those who do not do well with a high-fiber diet [5] • SIBO [33] • Constipation [30] • Non-celiac gluten sensitivity, celiac disease [12] • Food sensitivity/intolerance such as lactose intolerance [43, 57, 58, 59, 60] • Histamine intolerance [38] • Kidney stones, ulcers, diverticulitis, gallbladder inflammation, bowel obstruction, stomach or intestinal cancer [30] • Crohn’s: Pain is more often in the right lower quadrant of the abdomen and in the upper abdomen [66] • Ulcerative colitis: Pain is more often in the lower abdomen [47, 66] |
Probiotics Low-FODMAP diet Digestive enzymes |
| Nausea | • Intestinal infections by bacteria, viruses, or fungi such as COVID-19 or food poisoning [67, 68] • Non-celiac gluten sensitivity, celiac disease [12] • Food allergies or sensitivity/intolerance such as lactose intolerance [57, 59, 69] • Atrophic/autoimmune gastritis [61] • Mold illness [51, 52] • Morning sickness, migraines, or medications [69] • GERD, ulcers, or intestinal obstruction [69] • Seasickness or motion sickness [69] |
Probiotics especially if the nausea is due to GERD [29] Intermittent fasting |
Common Gastrointestinal Disorders and Treatment
If you have been experiencing multiple different GI symptoms for a long time, you may be dealing with one of the most common causes of GI symptoms that I see in the clinic: SIBO, H. pylori infection, IBD, IBS, or leaky gut.
The good news is that the same simple steps can generally be followed to heal your gut, no matter which diagnosis you receive. These steps are:
- Reset your gut with an anti-inflammatory diet, such as a Paleo or low FODMAP diet.
- Support a healthy gut microbiome and digestive system with probiotics, and potentially digestive enzymes.
- Remove any bad bugs causing symptoms with herbal antimicrobials.
Let’s look a bit closer at these conditions and why these treatments work for each of them.
| Condition | Common Symptoms | Research on Treatments |
| SIBO (small intestinal bacterial overgrowth) | • Gas, bloating, constipation, diarrhea, fatigue, brain fog, and abdominal pain. • High prevalence of SIBO in IBS and IBD cases [70, 71]. | Low-FODMAP diet: A large body of research has shown that a low-FODMAP diet improves symptoms of IBS and IBD, which may overlap with SIBO [31, 72, 73]. Probiotics: These help reduce bacterial overgrowth and the high hydrogen concentrations found in SIBO. They also improve the symptoms of SIBO. Digestive enzymes: In SIBO, the digestive system has difficulty digesting certain carbohydrates and sugar. Adding digestive enzymes can help aid digestion and reduce symptoms [22]. Herbal antimicrobials have been found to be as effective as rifaximin and triple antibiotic therapy for SIBO [74]. |
| IBS (irritable bowel syndrome) | • Gas, bloating, constipation, diarrhea, fatigue, brain fog, and abdominal pain. • IBS pain can be in different areas when it presents in the abdomen. | Low-FODMAP diet: to resolve leaky gut and immune response. In typical gastroenterology, IBS is diagnosed when there are chronic GI symptoms with no discernible cause. However, research does show that IBS is related to leaky gut and an improper immune response [75]. Probiotics: To help heal leaky gut as IBS is associated with leaky gut. Fecal tests to rule out infections. |
| IBD (Crohn’s and ulcerative colitis) | • Gas, bloating, constipation, diarrhea, fatigue, brain fog, and abdominal pain. • In IBD, Crohn’s can affect any part of the GI tract, while colitis affects the colon. • The pain of IBD is more often in the right lower quadrant of the abdomen and upper abdomen in Crohn’s while pain is more often in the lower abdomen in ulcerative colitis, in the colon [66]. | Both forms of IBD are inflammatory diseases of the digestive tract, also often related to an improper immune response and leaky gut [46]. Probiotics: To help heal leaky gut as both forms of IBD are associated with leaky gut. Fecal tests to rule out infections. |
| Helicobacter Pylori infection | • Gas, bloating abdominal pain, brain fog, fatigue, and nausea. • Reflux and GERD. • Ulcers. | Probiotics: Multi-strain probiotics can prevent H. pylori infection and help treat infection [76, 77]. Herbal antimicrobials: These improve the elimination rate of the bacteria and peptic ulcer healing compared to regular therapy with berberine [78]. |
Your Gut Support Plan

Living with gastrointestinal symptoms can cause a lot of stress and create worry every time a new symptom pops up. While it is helpful to know what some of the different kinds of gastrointestinal diseases there are, it is also important to remember that leading a gut healthy lifestyle may resolve your symptoms.
If you want to start improving your gastrointestinal symptoms, rather than changing everything at once, which makes tracking what is working more difficult, start first with a gut reset and gut support by trying an anti-inflammatory diet with probiotics. I suggest starting with the Paleo diet (removes inflammatory grains, dairy, and legumes) first as it is a bit easier to follow than jumping right into a low-FODMAP diet (and this more restrictive diet may not be necessary). Try this diet with probiotics for four weeks and track your symptoms to note any improvements.
If after four weeks you are still experiencing digestive symptoms, you may want to add in digestive enzymes to aid in digestion and remove any microbes that may be causing issues by taking herbal antimicrobials, again tracking symptoms.
While treating gastrointestinal distress can take a while, taking a stepped approach and recording your progress will help you not only troubleshoot what improves your symptoms, but give you agency over your own health.
We know that treating chronic GI symptoms can be overwhelming. My book, “Healthy Gut, Healthy You,” can help you learn more about gut healing and resolving gastrointestinal symptoms. If you would like a more personalized plan of treatment, please reach out to our clinic.
Dr. Michael Ruscio is a DC, natural health provider, researcher, and clinician. He serves as an Adjunct Professor at the University of Bridgeport and has published numerous papers in scientific journals as well as the book Healthy Gut, Healthy You. He also founded the Ruscio Institute of Functional Health, where he helps patients with a wide range of GI conditions and serves as the Head of Research.➕ References
- Diaz S, Bittar K, Mendez MD. Constipation. In: StatPearls. Treasure Island (FL): StatPearls Publishing; 2021. PMID: 30020663.
- Zhang C, Jiang J, Tian F, Zhao J, Zhang H, Zhai Q, et al. Meta-analysis of randomized controlled trials of the effects of probiotics on functional constipation in adults. Clin Nutr. 2020 Oct;39(10):2960–9. DOI: 10.1016/j.clnu.2020.01.005. PMID: 32005532.
- Miller LE, Ouwehand AC, Ibarra A. Effects of probiotic-containing products on stool frequency and intestinal transit in constipated adults: systematic review and meta-analysis of randomized controlled trials. Ann Gastroenterol. 2017 Sep 21;30(6):629–39. DOI: 10.20524/aog.2017.0192. PMID: 29118557. PMCID: PMC5670282.
- Martínez-Martínez MI, Calabuig-Tolsá R, Cauli O. The effect of probiotics as a treatment for constipation in elderly people: A systematic review. Arch Gerontol Geriatr. 2017 Jul;71:142–9. DOI: 10.1016/j.archger.2017.04.004. PMID: 28467916.
- El-Salhy M, Ystad SO, Mazzawi T, Gundersen D. Dietary fiber in irritable bowel syndrome (Review). Int J Mol Med. 2017 Sep;40(3):607–13. DOI: 10.3892/ijmm.2017.3072. PMID: 28731144. PMCID: PMC5548066.
- Moayyedi P, Quigley EMM, Lacy BE, Lembo AJ, Saito YA, Schiller LR, et al. The effect of fiber supplementation on irritable bowel syndrome: a systematic review and meta-analysis. Am J Gastroenterol. 2014 Sep;109(9):1367–74. DOI: 10.1038/ajg.2014.195. PMID: 25070054.
- Bellini M, Gambaccini D, Salvadori S, Tosetti C, Urbano MT, Costa F, et al. Management of chronic constipation in general practice. Tech Coloproctol. 2014 Jun;18(6):543–9. DOI: 10.1007/s10151-013-1093-9. PMID: 24272606.
- Weir I, Shu Q, Wei N, Wei C, Zhu Y. Efficacy of actinidin-containing kiwifruit extract Zyactinase on constipation: a randomised double-blinded placebo-controlled clinical trial. Asia Pac J Clin Nutr. 2018;27(3):564–71. DOI: 10.6133/apjcn.122017.03. PMID: 29737803.
- Nemeth V, Pfleghaar N. Diarrhea. In: StatPearls. Treasure Island (FL): StatPearls Publishing; 2021. PMID: 28846339.
- Chang J, Leong RW, Wasinger VC, Ip M, Yang M, Phan TG. Impaired intestinal permeability contributes to ongoing bowel symptoms in patients with inflammatory bowel disease and mucosal healing. Gastroenterology. 2017 Sep;153(3):723-731.e1. DOI: 10.1053/j.gastro.2017.05.056. PMID: 28601482.
- Michielan A, D’Incà R. Intestinal permeability in inflammatory bowel disease: pathogenesis, clinical evaluation, and therapy of leaky gut. Mediators Inflamm. 2015 Oct 25;2015:628157. DOI: 10.1155/2015/628157. PMID: 26582965. PMCID: PMC4637104.
- Volta U, Bardella MT, Calabrò A, Troncone R, Corazza GR, Study Group for Non-Celiac Gluten Sensitivity. An Italian prospective multicenter survey on patients suspected of having non-celiac gluten sensitivity. BMC Med. 2014 May 23;12(1):85. DOI: 10.1186/1741-7015-12-85. PMID: 24885375. PMCID: PMC4053283.
- Ruscio M. Is SIBO A real condition? Altern Ther Health Med. 2019 Sep;25(5):30–8. PMID: 31550680.
- Mujagic Z, Ludidi S, Keszthelyi D, Hesselink MAM, Kruimel JW, Lenaerts K, et al. Small intestinal permeability is increased in diarrhoea predominant IBS, while alterations in gastroduodenal permeability in all IBS subtypes are largely attributable to confounders. Aliment Pharmacol Ther. 2014 Aug;40(3):288–97. DOI: 10.1111/apt.12829. PMID: 24943095.
- Hempel S, Newberry SJ, Maher AR, Wang Z, Miles JNV, Shanman R, et al. Probiotics for the prevention and treatment of antibiotic-associated diarrhea: a systematic review and meta-analysis. JAMA. 2012 May 9;307(18):1959–69. DOI: 10.1001/jama.2012.3507. PMID: 22570464.
- Zhou Q, Verne ML, Fields JZ, Lefante JJ, Basra S, Salameh H, et al. Randomised placebo-controlled trial of dietary glutamine supplements for postinfectious irritable bowel syndrome. Gut. 2019 Jun;68(6):996–1002. DOI: 10.1136/gutjnl-2017-315136. PMID: 30108163.
- Dumitrascu DL, Baban A, Bancila I, Barboi O, Bataga S, Chira A, et al. Romanian guidelines for nonpharmacological therapy of IBS. J Gastrointestin Liver Dis. 2021 Jun 18;30(2):291–306. DOI: 10.15403/jgld-3581. PMID: 33951120.
- Zhang L, Sizar O, Higginbotham K. Meteorism. In: StatPearls. Treasure Island (FL): StatPearls Publishing; 2021. PMID: 28613601.
- Tuck CJ, Taylor KM, Gibson PR, Barrett JS, Muir JG. Increasing Symptoms in Irritable Bowel Symptoms With Ingestion of Galacto-Oligosaccharides Are Mitigated by α-Galactosidase Treatment. Am J Gastroenterol. 2018 Jan;113(1):124–34. DOI: 10.1038/ajg.2017.245. PMID: 28809383.
- Yuan F, Ni H, Asche CV, Kim M, Walayat S, Ren J. Efficacy of Bifidobacterium infantis 35624 in patients with irritable bowel syndrome: a meta-analysis. Curr Med Res Opin. 2017 Jul;33(7):1191–7. DOI: 10.1080/03007995.2017.1292230. PMID: 28166427.
- Rogha M, Esfahani MZ, Zargarzadeh AH. The efficacy of a synbiotic containing Bacillus Coagulans in treatment of irritable bowel syndrome: a randomized placebo-controlled trial. Gastroenterol Hepatol Bed Bench. 2014;7(3):156–63. PMID: 25120896. PMCID: PMC4129566.
- Spagnuolo R, Cosco C, Mancina RM, Ruggiero G, Garieri P, Cosco V, et al. Beta-glucan, inositol and digestive enzymes improve quality of life of patients with inflammatory bowel disease and irritable bowel syndrome. Eur Rev Med Pharmacol Sci. 2017 Jun;21(2 Suppl):102–7. PMID: 28724171.
- Ciacci C, Franceschi F, Purchiaroni F, Capone P, Buccelletti F, Iacomini P, et al. Effect of beta-glucan, inositol and digestive enzymes in GI symptoms of patients with IBS. Eur Rev Med Pharmacol Sci. 2011 Jun;15(6):637–43. PMID: 21796867.
- Antunes C, Aleem A, Curtis SA. Gastroesophageal Reflux Disease. In: StatPearls. Treasure Island (FL): StatPearls Publishing; 2021. PMID: 28722967.
- Brown J, Shermetaro C. Laryngopharyngeal Reflux. In: StatPearls. Treasure Island (FL): StatPearls Publishing; 2021. PMID: 30137832.
- Bang CS, Yang YJ, Baik GH. Melatonin for the treatment of gastroesophageal reflux disease; protocol for a systematic review and meta-analysis. Medicine (Baltimore). 2019 Jan;98(4):e14241. DOI: 10.1097/MD.0000000000014241. PMID: 30681611. PMCID: PMC6358381.
- Kandil TS, Mousa AA, El-Gendy AA, Abbas AM. The potential therapeutic effect of melatonin in Gastro-Esophageal Reflux Disease. BMC Gastroenterol. 2010 Jan 18;10:7. DOI: 10.1186/1471-230X-10-7. PMID: 20082715. PMCID: PMC2821302.
- Pereira R de S. Regression of gastroesophageal reflux disease symptoms using dietary supplementation with melatonin, vitamins and aminoacids: comparison with omeprazole. J Pineal Res. 2006 Oct;41(3):195–200. DOI: 10.1111/j.1600-079X.2006.00359.x. PMID: 16948779.
- Cheng J, Ouwehand AC. Gastroesophageal reflux disease and probiotics: A systematic review. Nutrients. 2020 Jan 2;12(1). DOI: 10.3390/nu12010132. PMID: 31906573. PMCID: PMC7019778.
- Abdominal pain: MedlinePlus Medical Encyclopedia [Internet]. [cited 2021 Jul 15]. Available from: https://medlineplus.gov/ency/article/003120.htm
- Marsh A, Eslick EM, Eslick GD. Does a diet low in FODMAPs reduce symptoms associated with functional gastrointestinal disorders? A comprehensive systematic review and meta-analysis. Eur J Nutr. 2016 Apr;55(3):897–906. DOI: 10.1007/s00394-015-0922-1. PMID: 25982757.
- Altobelli E, Del Negro V, Angeletti PM, Latella G. Low-FODMAP Diet Improves Irritable Bowel Syndrome Symptoms: A Meta-Analysis. Nutrients. 2017 Aug 26;9(9). DOI: 10.3390/nu9090940. PMID: 28846594. PMCID: PMC5622700.
- Zhong C, Qu C, Wang B, Liang S, Zeng B. Probiotics for Preventing and Treating Small Intestinal Bacterial Overgrowth: A Meta-Analysis and Systematic Review of Current Evidence. J Clin Gastroenterol. 2017 Apr;51(4):300–11. DOI: 10.1097/MCG.0000000000000814. PMID: 28267052.
- Gudipally PR, Sharma GK. Premenstrual Syndrome. In: StatPearls. Treasure Island (FL): StatPearls Publishing; 2021. PMID: 32809533.
- Kanazawa M, Fukudo S. Effects of fasting therapy on irritable bowel syndrome. Int J Behav Med. 2006;13(3):214–20. DOI: 10.1207/s15327558ijbm1303_4. PMID: 17078771.
- Kurin M, Cooper G. Irritable bowel syndrome with diarrhea: Treatment is a work in progress. Cleve Clin J Med. 2020 Jul 31;87(8):501–11. DOI: 10.3949/ccjm.87a.19011. PMID: 32737051.
- Meleine M, Matricon J. Gender-related differences in irritable bowel syndrome: potential mechanisms of sex hormones. World J Gastroenterol. 2014 Jun 14;20(22):6725–43. DOI: 10.3748/wjg.v20.i22.6725. PMID: 24944465. PMCID: PMC4051914.
- Schnedl WJ, Enko D. Histamine intolerance originates in the gut. Nutrients. 2021 Apr 12;13(4). DOI: 10.3390/nu13041262. PMID: 33921522. PMCID: PMC8069563.
- Southwell BR. Treatment of childhood constipation: a synthesis of systematic reviews and meta-analyses. Expert Rev Gastroenterol Hepatol. 2020 Mar;14(3):163–74. DOI: 10.1080/17474124.2020.1733974. PMID: 32098515.
- Zhao S-R, Ni X-M, Zhang X-A, Tian H. Effect of cognitive behavior therapy combined with exercise intervention on the cognitive bias and coping styles of diarrhea-predominant irritable bowel syndrome patients. World J Clin Cases. 2019 Nov 6;7(21):3446–62. DOI: 10.12998/wjcc.v7.i21.3446. PMID: 31750328. PMCID: PMC6854400.
- Lackner JM, Jaccard J, Keefer L, Brenner DM, Firth RS, Gudleski GD, et al. Improvement in gastrointestinal symptoms after cognitive behavior therapy for refractory irritable bowel syndrome. Gastroenterology. 2018 Jul;155(1):47–57. DOI: 10.1053/j.gastro.2018.03.063. PMID: 29702118. PMCID: PMC6035059.
- Shah K, Ramos-Garcia M, Bhavsar J, Lehrer P. Mind-body treatments of irritable bowel syndrome symptoms: An updated meta-analysis. Behav Res Ther. 2020 May;128:103462. DOI: 10.1016/j.brat.2019.103462. PMID: 32229334.
- Misselwitz B, Pohl D, Frühauf H, Fried M, Vavricka SR, Fox M. Lactose malabsorption and intolerance: pathogenesis, diagnosis and treatment. United European Gastroenterol J. 2013 Jun;1(3):151–9. DOI: 10.1177/2050640613484463. PMID: 24917953. PMCID: PMC4040760.
- Leeds JS, Hopper AD, Sidhu R, Simmonette A, Azadbakht N, Hoggard N, et al. Some patients with irritable bowel syndrome may have exocrine pancreatic insufficiency. Clin Gastroenterol Hepatol. 2010 May;8(5):433–8. DOI: 10.1016/j.cgh.2009.09.032. PMID: 19835990.
- Othman MO, Harb D, Barkin JA. Introduction and practical approach to exocrine pancreatic insufficiency for the practicing clinician. Int J Clin Pract. 2018 Feb 5;72(2). DOI: 10.1111/ijcp.13066. PMID: 29405509. PMCID: PMC5873407.
- Ranasinghe IR, Hsu R. Crohn Disease. In: StatPearls. Treasure Island (FL): StatPearls Publishing; 2021. PMID: 28613792.
- Choi YS, Kim DS, Lee DH, Lee JB, Lee EJ, Lee SD, et al. Clinical characteristics and incidence of perianal diseases in patients with ulcerative colitis. Ann Coloproctol. 2018 Jun 30;34(3):138–43. DOI: 10.3393/ac.2017.06.08. PMID: 29991202. PMCID: PMC6046543.
- Bolshinsky V, Church J. Management of complex anorectal and perianal crohn’s disease. Clin Colon Rectal Surg. 2019 Jul 2;32(4):255–60. DOI: 10.1055/s-0039-1683907. PMID: 31275071. PMCID: PMC6606315.
- Daher R, Yazbeck T, Jaoude JB, Abboud B. Consequences of dysthyroidism on the digestive tract and viscera. World J Gastroenterol. 2009 Jun 21;15(23):2834–8. PMID: 19533804. PMCID: PMC2699000.
- Munjal A, Dedania B, Cash BD. Current and emerging pharmacological approaches for treating diarrhea-predominant irritable bowel syndrome. Expert Opin Pharmacother. 2020 Jan;21(1):63–71. DOI: 10.1080/14656566.2019.1691524. PMID: 31738621.
- Liew W-P-P, Mohd-Redzwan S. Mycotoxin: its impact on gut health and microbiota. Front Cell Infect Microbiol. 2018 Feb 26;8:60. DOI: 10.3389/fcimb.2018.00060. PMID: 29535978. PMCID: PMC5834427.
- Lebrun B, Tardivel C, Félix B, Abysique A, Troadec J-D, Gaigé S, et al. Dysregulation of energy balance by trichothecene mycotoxins: Mechanisms and prospects. Neurotoxicology. 2015 Jul;49:15–27. DOI: 10.1016/j.neuro.2015.04.009. PMID: 25956358.
- Mazzawi T, El-Salhy M. Changes in duodenal enteroendocrine cells in patients with irritable bowel syndrome following dietary guidance. Exp Biol Med (Maywood). 2017 Jul;242(13):1355–62. DOI: 10.1177/1535370217699537. PMID: 28737477. PMCID: PMC5528200.
- Mazzawi T, Hausken T, Gundersen D, El-Salhy M. Dietary guidance normalizes large intestinal endocrine cell densities in patients with irritable bowel syndrome. Eur J Clin Nutr. 2016 Feb;70(2):175–81. DOI: 10.1038/ejcn.2015.191. PMID: 26603880. PMCID: PMC4744244.
- Löhr JM, Panic N, Vujasinovic M, Verbeke CS. The ageing pancreas: a systematic review of the evidence and analysis of the consequences. J Intern Med. 2018 May;283(5):446–60. DOI: 10.1111/joim.12745. PMID: 29474746.
- Ghoshal UC. Antibiotic treatment for small intestinal bacterial overgrowth: Is a cocktail better than a single? United European Gastroenterol J. 2021 May 5; DOI: 10.1002/ueg2.12075. PMID: 33951351. PMCID: PMC8280792.
- Dieterich W, Zopf Y. Gluten and FODMAPS-Sense of a Restriction/When Is Restriction Necessary? Nutrients. 2019 Aug 20;11(8). DOI: 10.3390/nu11081957. PMID: 31434299. PMCID: PMC6723650.
- Gibson PR, Shepherd SJ. Evidence-based dietary management of functional gastrointestinal symptoms: The FODMAP approach. J Gastroenterol Hepatol. 2010 Feb;25(2):252–8. DOI: 10.1111/j.1440-1746.2009.06149.x. PMID: 20136989.
- Deng Y, Misselwitz B, Dai N, Fox M. Lactose intolerance in adults: biological mechanism and dietary management. Nutrients. 2015 Sep 18;7(9):8020–35. DOI: 10.3390/nu7095380. PMID: 26393648. PMCID: PMC4586575.
- Zhu Y, Zheng X, Cong Y, Chu H, Fried M, Dai N, et al. Bloating and distention in irritable bowel syndrome: the role of gas production and visceral sensation after lactose ingestion in a population with lactase deficiency. Am J Gastroenterol. 2013 Sep;108(9):1516–25. DOI: 10.1038/ajg.2013.198. PMID: 23917444.
- Annibale B, Esposito G, Lahner E. A current clinical overview of atrophic gastritis. Expert Rev Gastroenterol Hepatol. 2020 Feb;14(2):93–102. DOI: 10.1080/17474124.2020.1718491. PMID: 31951768.
- Carabotti M, Lahner E, Esposito G, Sacchi MC, Severi C, Annibale B. Upper gastrointestinal symptoms in autoimmune gastritis: A cross-sectional study. Medicine (Baltimore). 2017 Jan;96(1):e5784. DOI: 10.1097/MD.0000000000005784. PMID: 28072728. PMCID: PMC5228688.
- Chubineh S, Birk J. Proton pump inhibitors: the good, the bad, and the unwanted. South Med J. 2012 Nov;105(11):613–8. DOI: 10.1097/SMJ.0b013e31826efbea. PMID: 23128806.
- Rodriguez-Castro KI, Franceschi M, Noto A, Miraglia C, Nouvenne A, Leandro G, et al. Clinical manifestations of chronic atrophic gastritis. Acta Biomed. 2018 Dec 17;89(8-S):88–92. DOI: 10.23750/abm.v89i8-S.7921. PMID: 30561424. PMCID: PMC6502219.
- Campbell R, Kilty SJ, Hutton B, Bonaparte JP. The Role of Helicobacter pylori in Laryngopharyngeal Reflux. Otolaryngol Head Neck Surg. 2017 Feb;156(2):255–62. DOI: 10.1177/0194599816676052. PMID: 27803078.
- CCFA C& CF of A. THE FACTS ABOUT Inflammatory Bowel Diseases [Internet]. THE FACTS ABOUT Inflammatory Bowel Diseases. 2014 [cited 2021 Jul 7]. Available from: https://www.crohnscolitisfoundation.org/sites/default/files/2019-02/Updated%20IBD%20Factbook.pdf
- Zhong W, Shahbaz O, Teskey G, Beever A, Kachour N, Venketaraman V, et al. Mechanisms of nausea and vomiting: current knowledge and recent advances in intracellular emetic signaling systems. Int J Mol Sci. 2021 May 28;22(11). DOI: 10.3390/ijms22115797. PMID: 34071460. PMCID: PMC8198651.
- Basics of COVID-19 | CDC [Internet]. [cited 2021 Jul 15]. Available from: https://www.cdc.gov/coronavirus/2019-ncov/your-health/about-covid-19/basics-covid-19.html
- Nausea and vomiting – adults: MedlinePlus Medical Encyclopedia [Internet]. [cited 2021 Jul 15]. Available from: https://medlineplus.gov/ency/article/003117.htm
- Chen B, Kim JJ-W, Zhang Y, Du L, Dai N. Prevalence and predictors of small intestinal bacterial overgrowth in irritable bowel syndrome: a systematic review and meta-analysis. J Gastroenterol. 2018 Jul;53(7):807–18. DOI: 10.1007/s00535-018-1476-9. PMID: 29761234.
- Shah A, Morrison M, Burger D, Martin N, Rich J, Jones M, et al. Systematic review with meta-analysis: the prevalence of small intestinal bacterial overgrowth in inflammatory bowel disease. Aliment Pharmacol Ther. 2019 Mar;49(6):624–35. DOI: 10.1111/apt.15133. PMID: 30735254.
- Staudacher HM, Whelan K. The low FODMAP diet: recent advances in understanding its mechanisms and efficacy in IBS. Gut. 2017 Aug;66(8):1517–27. DOI: 10.1136/gutjnl-2017-313750. PMID: 28592442.
- Schumann D, Klose P, Lauche R, Dobos G, Langhorst J, Cramer H. Low fermentable, oligo-, di-, mono-saccharides and polyol diet in the treatment of irritable bowel syndrome: A systematic review and meta-analysis. Nutrition. 2018 Jan;45:24–31. DOI: 10.1016/j.nut.2017.07.004. PMID: 29129233.
- Chedid V, Dhalla S, Clarke JO, Roland BC, Dunbar KB, Koh J, et al. Herbal therapy is equivalent to rifaximin for the treatment of small intestinal bacterial overgrowth. Glob Adv Health Med. 2014 May;3(3):16–24. DOI: 10.7453/gahmj.2014.019. PMID: 24891990. PMCID: PMC4030608.
- Camilleri M, Gorman H. Intestinal permeability and irritable bowel syndrome. Neurogastroenterol Motil. 2007 Jul;19(7):545–52. DOI: 10.1111/j.1365-2982.2007.00925.x. PMID: 17593135.
- Koga Y, Ohtsu T, Kimura K, Asami Y. Probiotic L. gasseri strain (LG21) for the upper gastrointestinal tract acting through improvement of indigenous microbiota. BMJ Open Gastroenterol. 2019 Aug 12;6(1):e000314. DOI: 10.1136/bmjgast-2019-000314. PMID: 31523442. PMCID: PMC6711431.
- Shi X, Zhang J, Mo L, Shi J, Qin M, Huang X. Efficacy and safety of probiotics in eradicating Helicobacter pylori: A network meta-analysis. Medicine (Baltimore). 2019 Apr;98(15):e15180. DOI: 10.1097/MD.0000000000015180. PMID: 30985706. PMCID: PMC6485819.
- Hu Q, Peng Z, Li L, Zou X, Xu L, Gong J, et al. The Efficacy of Berberine-Containing Quadruple Therapy on Helicobacter Pylori Eradication in China: A Systematic Review and Meta-Analysis of Randomized Clinical Trials. Front Pharmacol. 2019;10:1694. DOI: 10.3389/fphar.2019.01694. PMID: 32116685. PMCID: PMC7010642.










Discussion
I care about answering your questions and sharing my knowledge with you. Leave a comment or connect with me on social media asking any health question you may have and I just might incorporate it into our next listener questions podcast episode just for you!