Can a Vagus Nerve Massage Really Work?
How a Vagus Nerve Massage Connects to Health and Wellness
- About Vagus Nerve Massages|
- The Vagus Nerve and the Body|
- Improving Vagal Tone|
- Vagus Nerve Interventions|
Improving vagal tone is a popular topic right now, and you may have seen suggestions such as tapping on your chest, gargling salt water, laughter, cold water exposure, massage, and deep breathing. However, not all of these techniques are proven to work.
In this article, we’ll explore the research about vagus nerve massages. You will learn how this technique works, whether it’s effective, who it is safe for, and what you want to look for in a massage therapist qualified to do this type of massage.
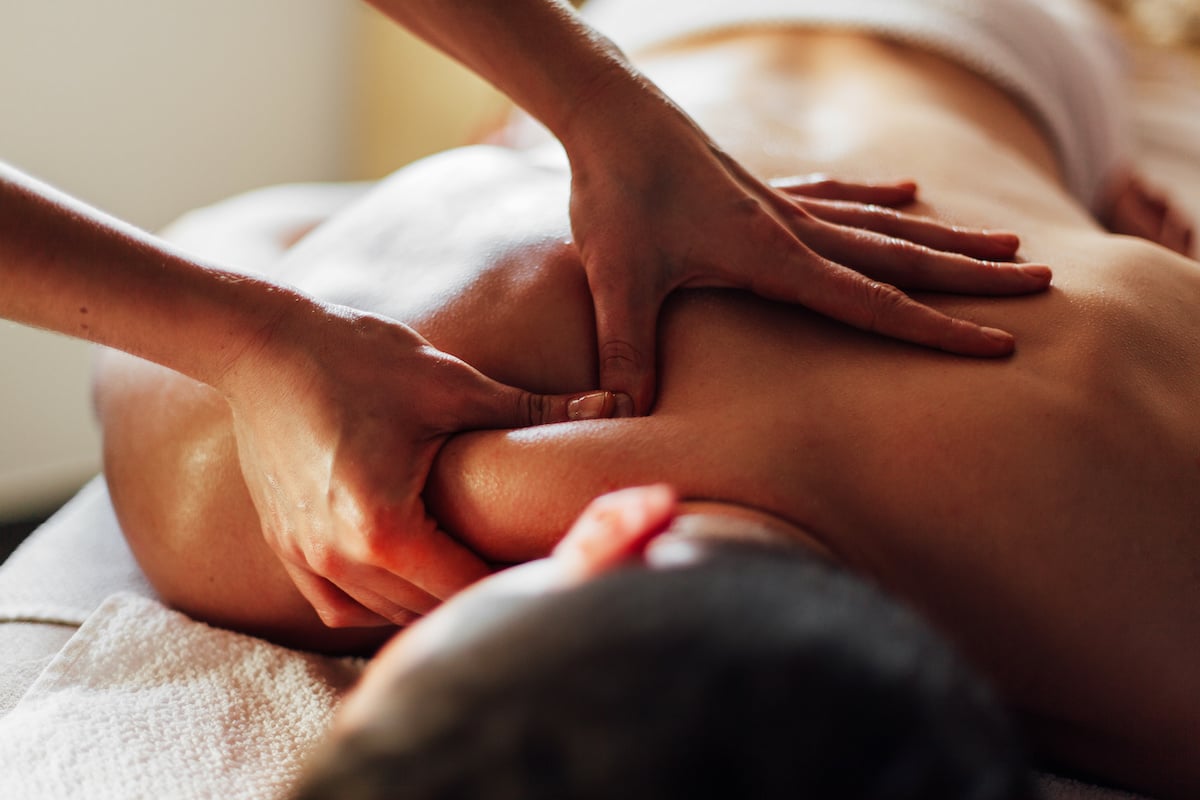
What Is a Vagus Nerve Massage?
Unlike what you might think, a vagus nerve massage doesn’t directly massage the vagus nerve. Rather, it is a massage of areas that are in close proximity to the vagus nerve. Vagus nerve massage is a form of vagus nerve stimulation, which helps improve vagal tone (another term for vagus nerve functioning).
In a vagus nerve massage, moderate pressure is applied to the area between the trapezius and sternocleidomastoid muscles in the neck/shoulder area and at the muscles below the base of the skull, with twisting or stroking motions 1.
The trapezius muscles are at the top of your shoulders and help move the neck and head, as well as move your shoulder blades. The sternocleidomastoid muscles go down the sides of your neck, from the base of your head. They help you rotate your head and keep your head aligned with your spine.
Another form of vagus nerve massage is called carotid sinus massage, which involves pressing lightly with the fingers on the side of the neck where the pulse from the carotid artery can be felt the strongest. CMS is meant to stimulate a receptor in the carotid artery (known as the carotid body) and raise vagal tone. The end goal is to slow a rapid heart rate and improve abnormal heart rhythms 2. It should not be used in people who have cardiovascular disease, and it shouldn’t be done outside a medical setting, without supervision by a doctor, as it could have dangerous side effects.
Does Vagus Nerve Massage Work?
There are not a lot of studies on vagus nerve massage, but the ones we do have show that a massage of the base of the head, neck, and shoulders can improve heart rate variability (the time between heartbeats, used to indirectly measure vagal tone) 1.
You may be wondering where you can find a massage therapy practice that specializes in vagus nerve massage. The good news is that a study comparing designated vagus nerve massage to regular soft shoulder massage found that a standard shoulder massage was just as effective. Both groups had a substantial increase in heart rate variability (HRV) after either kind of massage for 10 minutes, as compared to controls who had no massage and just had rest only 1.
There are some claims that massage of other areas of the body, such as foot massage or massage of the eyes or belly, can also improve vagal tone. However, the research we have really only supports massage of the head, neck, and shoulder areas. This does not mean that massage of other areas proximal to the vagus nerve, such as the eyes or belly, do not work. Rather, it means we do not have enough clinical studies to show that they work yet.
In order to decide if you want to add vagus nerve stimulation to your treatment regimen, it is helpful to know how the vagus nerve affects the body and our well-being.
How the Vagus Nerve Affects the Body

Poor vagus nerve functioning (low vagal tone) has been associated with IBS and IBD as well as heart disease, depression, and autoimmune conditions.
Good functioning of the vagus nerve is important for the gut-brain connection as well as our digestion, heart and breathing regulation, and emotional wellbeing.
Why and how is this one nerve not only important for your digestion but also your mental health, blood pressure, heartbeat, ability to swallow, and your immune system 3?
First, let’s cover what the vagus nerve is. It is the 10th cranial nerve, extending from the brainstem all the way down to the gastrointestinal tract 4. The far reach of this nerve explains why it affects so many parts of the body. It is involved with regulating everything from digestion, to hormone production (such as our stress hormone cortisol,) as well as emotions and our heartbeat and breathing.
Let’s take a more in-depth look at a few of these body systems in relationship to the vagus nerve.
Autonomic Nervous System
The vagus nerve is part of the autonomic nervous system of the body, which helps regulate blood pressure, heart rate, breathing, hormones (endocrine system), and digestion 3 5. This is why a poorly functioning vagus nerve can contribute to symptoms such as irregular heart beat, shallow breathing, and low blood pressure.
The vagus nerve is also part of the parasympathetic nervous system, which operates in opposition to the sympathetic nervous system 6. The parasympathetic system helps us relax and regulate our digestion. The sympathetic nervous system is associated with our fight-or-flight response that helps us respond appropriately to stressful situations and helps redirect oxygen-rich blood flow to where it’s most needed 7.
If our parasympathetic nervous system, regulated by the vagus nerve, isn’t working well, then the sympathetic nervous system may become over-activated and contribute to chronic anxiety, chronic pain, and mood dysregulation.
Brain Function and Mental Health
Have you heard of the gut-brain axis? This is the bi-directional pathway that sends signals from the brain to the gut and vice versa. This is the vagus nerve 5 8.
Not only does this help regulate the digestive system, but it also helps produce neurotransmitters. Neurotransmitters help regulate our moods, with serotonin and dopamine regulating the emotional states of happiness or depression. Proper levels of neurotransmitters are also needed to keep the neural connections required for good long and short-term memory.
Electrical vagal nerve stimulation (VNS) was shown to improve moods and emotional and cognitive function 9. Poor vagal activity may be a contributing factor in neurological conditions such as depression, schizophrenia, and Parkinson’s disease 8.
The gut-brain axis helps regulate the immune system, so good vagal tone is important for immunity and general wellness 10.
Gut Health
Because of the vagus nerve’s role in regulating automatic functions of the body, it is extremely important for gut health. It controls the motor fibers (efferent fibers) of the digestive tract. These motor fibers create and regulate the contractions of the muscles that move food through the digestive tract.
If the vagus nerve is not working properly, you may experience diarrhea, constipation, or bloating often seen in inflammatory bowel disorders 5. Improving vagal tone can help improve IBD symptoms 11 12.
Simple Ways to Improve Vagal Tone
In general, many things that are good for your overall health also seem to have a beneficial impact on vagal tone. Here are a few simple techniques, including but not limited to vagus nerve massages, that you can incorporate into your life.
In order to know if any of the interventions below are working, track your emotional and physical symptoms. If you have a device, such as an Oura Ring or Whoop Band, that tracks your heart rate variability (HRV) you can also note if your HRV improves (gets higher) over time.
Massage
Any form of moderate massage to the neck and shoulders can help improve the functioning of your vagus nerve. A painful form of massage may not be a great choice because muscle pain may trigger the sympathetic nervous system, causing a “fight or flight” response.
If you are new to massage, stick to moderate pressure, relaxing and sessions are about 10 minutes, on the neck and shoulder area.
The research only studied one session of massage, but long-term improvement of HRV is seen with regular vagus nerve work. Regular massages seem to be the most beneficial to vagal tone 1.
Deep Breathing
You can also improve vagal tone at home through deep diaphragmatic breathing exercises or mindfulness meditation. In fact, deep breathing was shown to improve heart rate variability, and thus blood pressure, in people with prehypertension 13.
The simplest form of this is to sit comfortably, with your eyes open and a soft gaze on the floor. Deeper breaths are best for regulating the vagus nerve 14, so at first try just breathing in for five counts, and out for five. You can also make the exhale a few seconds longer than the inhale for even more vagal nerve stimulation.
If you are new to deep breathing, extremely long breaths or breath holds can feel scary to some people and trigger a fear response. To avoid this, start with just breathing in and out, from the belly, for 10 minutes. Then, you can add other breathing patterns if you’re comfortable.
Diet, Exercise, and Cold Therapy
Adding massage or deep breathing into your life are great ways to improve your health. There are other ways to improve your vagal tone, such as through diet, exercise, and cold water therapy.
An inflammatory diet taxes the gastrointestinal system and can aggravate the parasympathetic nervous system via the gut-brain axis 4 15. A diet that removes inflammatory foods such as grains and dairy may help improve vagal tone 16.
While any kind of exercise is helpful to the nervous system, high intensity interval training (HIIT) has been shown to create the most improvement in HRV 17. Adding two sessions of HIIT training per week is an easy and accessible way to improve vagal tone. Sometimes people assume more is better on the exercise front, but too much HIIT training, such as 5-7 days a week, can decrease HRV.
If you want to make your exercise even more effective at improving your HRV, make the last 10-20 seconds of your post-workout shower as cold as you can handle it for cold water therapy. Cold water immersion helps with muscle recovery as well as improving HRV and increasing parasympathetic nervous system activity 18.
Implementing Vagus Nerve Interventions
Maintaining good functioning of the vagus nerve is important for your wellbeing. If you struggle with anxiety and/or have gastrointestinal symptoms or IBD such as Crohns or colitis, improving vagal tone can be a great addition to your treatment plan.
Adding in a massage of the neck and shoulders once a week is a simple intervention, as regular massage significantly improves HRV, and thus vagal tone.
If you are really struggling with more severe gastrointestinal and emotional symptoms, you may want to consider creating a good foundation of health with an anti-inflammatory vagus nerve diet. Decreasing inflammation in the gut can help support the gut-brain axis- the vagus nerve.
Rather than trying multiple interventions all at one time, try one for a month and track how you feel. If you have a way to track your HRV, see if it improves over the month.
If you would like help finding which vagus nerve massage or other vagus nerve interventions are best for you and what other interventions might benefit your wellness, reach out to us at the clinic to become a patient.
Dr. Michael Ruscio is a DC, natural health provider, researcher, and clinician. He serves as an Adjunct Professor at the University of Bridgeport and has published numerous papers in scientific journals as well as the book Healthy Gut, Healthy You. He also founded the Ruscio Institute of Functional Health, where he helps patients with a wide range of GI conditions and serves as the Head of Research.➕ References
- Meier M, Unternaehrer E, Dimitroff SJ, Benz ABE, Bentele UU, Schorpp SM, et al. Standardized massage interventions as protocols for the induction of psychophysiological relaxation in the laboratory: a block randomized, controlled trial. Sci Rep. 2020 Sep 8;10(1):14774. DOI: 10.1038/s41598-020-71173-w. PMID: 32901072. PMCID: PMC7479151.
- Niehues LJ, Klovenski V. Vagal Maneuver. In: StatPearls. Treasure Island (FL): StatPearls Publishing; 2021. PMID: 31855402.
- Yuan H, Silberstein SD. Vagus nerve and vagus nerve stimulation, a comprehensive review: part I. Headache. 2016 Jan;56(1):71–8. DOI: 10.1111/head.12647. PMID: 26364692.
- Kenny BJ, Bordoni B. Neuroanatomy, cranial nerve 10 (vagus nerve). In: StatPearls. Treasure Island (FL): StatPearls Publishing; 2018. PMID: 30725856.
- Breit S, Kupferberg A, Rogler G, Hasler G. Vagus Nerve as Modulator of the Brain-Gut Axis in Psychiatric and Inflammatory Disorders. Front Psychiatry. 2018 Mar 13;9:44. DOI: 10.3389/fpsyt.2018.00044. PMID: 29593576. PMCID: PMC5859128.
- Tindle J, Tadi P. Neuroanatomy, parasympathetic nervous system. In: StatPearls. Treasure Island (FL): StatPearls Publishing; 2021. PMID: 31985934.
- Alshak MN, M Das J. Neuroanatomy, sympathetic nervous system. In: StatPearls. Treasure Island (FL): StatPearls Publishing; 2021. PMID: 31194352.
- Arneth BM. Gut-brain axis biochemical signalling from the gastrointestinal tract to the central nervous system: gut dysbiosis and altered brain function. Postgrad Med J. 2018 Aug;94(1114):446–52. DOI: 10.1136/postgradmedj-2017-135424. PMID: 30026389.
- Howland RH. Vagus Nerve Stimulation. Curr Behav Neurosci Rep. 2014 Jun;1(2):64–73. DOI: 10.1007/s40473-014-0010-5. PMID: 24834378. PMCID: PMC4017164.
- Jacobson A, Yang D, Vella M, Chiu IM. The intestinal neuro-immune axis: crosstalk between neurons, immune cells, and microbes. Mucosal Immunol. 2021 May;14(3):555–65. DOI: 10.1038/s41385-020-00368-1. PMID: 33542493. PMCID: PMC8075967.
- Mogilevski T, Burgell R, Aziz Q, Gibson PR. Review article: the role of the autonomic nervous system in the pathogenesis and therapy of IBD. Aliment Pharmacol Ther. 2019 Oct;50(7):720–37. DOI: 10.1111/apt.15433. PMID: 31418887.
- Bonaz B, Sinniger V, Pellissier S. Therapeutic potential of vagus nerve stimulation for inflammatory bowel diseases. Front Neurosci. 2021 Mar 22;15:650971. DOI: 10.3389/fnins.2021.650971. PMID: 33828455. PMCID: PMC8019822.
- Lin G, Xiang Q, Fu X, Wang S, Wang S, Chen S, et al. Heart rate variability biofeedback decreases blood pressure in prehypertensive subjects by improving autonomic function and baroreflex. J Altern Complement Med. 2012 Feb;18(2):143–52. DOI: 10.1089/acm.2010.0607. PMID: 22339103.
- Lin IM, Tai LY, Fan SY. Breathing at a rate of 5.5 breaths per minute with equal inhalation-to-exhalation ratio increases heart rate variability. Int J Psychophysiol. 2014 Mar;91(3):206–11. DOI: 10.1016/j.ijpsycho.2013.12.006. PMID: 24380741.
- Liu Q, Wang EM, Yan XJ, Chen SL. Autonomic functioning in irritable bowel syndrome measured by heart rate variability: a meta-analysis. J Dig Dis. 2013 Dec;14(12):638–46. DOI: 10.1111/1751-2980.12092. PMID: 23927739.
- Charlebois A, Rosenfeld G, Bressler B. The impact of dietary interventions on the symptoms of inflammatory bowel disease: A systematic review. Crit Rev Food Sci Nutr. 2016 Jun 10;56(8):1370–8. DOI: 10.1080/10408398.2012.760515. PMID: 25569442.
- Guiraud T, Labrunee M, Gaucher-Cazalis K, Despas F, Meyer P, Bosquet L, et al. High-intensity interval exercise improves vagal tone and decreases arrhythmias in chronic heart failure. Med Sci Sports Exerc. 2013 Oct;45(10):1861–7. DOI: 10.1249/MSS.0b013e3182967559. PMID: 23591293.
- Yuen AWC, Sander JW. Can natural ways to stimulate the vagus nerve improve seizure control? Epilepsy Behav. 2017 Feb;67:105–10. DOI: 10.1016/j.yebeh.2016.10.039. PMID: 28152451.

Discussion
I care about answering your questions and sharing my knowledge with you. Leave a comment or connect with me on social media asking any health question you may have and I just might incorporate it into our next listener questions podcast episode just for you!