Specific Tests and Tips for Detecting a Brain to Gut Problem
Brain-based therapies for the gut with Dr. Titus Chiu.
Neural pathways that form the brain to gut connections can be damaged as a result of a concussion or other traumatic injury. For some patients whose symptoms don’t fully resolve with gut therapies, new treatments that stimulate neural pathways may be helpful.
Functional neurology is an area of clinical practice that opens a window onto brain-based problems and provides some novel therapies. Today we talk about diagnostic clues for detecting a brain-to-gut problem and we explore electroceuticals, a new category of therapies that stimulate specific neural pathways with electricity.
Gut-brain anatomy
- Insular cortex
- Interoceptive – awareness of what’s happening inside
- Processes what’s happening in the gut
- Processes emotions and compassion
- Processes vestibular sensations
- Vagus nerve
- Pneumogastric nerve, interfaces with parasympathetic control of the heart, lungs, and digestive tract
Hierarchy for treatment approach
- It can be a challenge to decide to start with either the brain or the gut, there are some indicators that might point to looking at the brain first like …
- Concussion history is a major flag to start with brain therapies
- Have you had a concussion? (car accident, whiplash)
- Participated in brain traumatic sports? (football, lacrosse, cheerleading, boxing, etc..)
- Emotional or physical trauma can also indicate that the brain is a good place to start
Testing, Research and Therapy
- Testing:
- A functional neurologist can perform neurological testing
- Also eye movements, balance testing, etc. might be necessary
- Gut testing would range from stool tests, breath tests, blood tests etc.
- Research: Scientific America paper about shock medicine
- Therapy:
- Consider “Electroceutical” type therapies if the issue seems to be emanating from brain trauma
- Eye movements, eye exercises can also be helpful
- If the issue seems to originate from the gut – therapies can range from diet, supplements, belly massage, etc.
- Consider “Electroceutical” type therapies if the issue seems to be emanating from brain trauma
- See a functional neurologist near you. Do your homework, ask questions and look at patient reviews
- Titus’s book Brain Save, includes a self-assessment quiz and treatment plans within the book
- Dr. Titus’s Clinical Practice.
In This Episode
Episode Intro … 00:00:40
The Brain-Gut Connection… 00:09:24
Detecting a Brain-to-Gut Problem… 00:11:56
Sponsored Resources … 00:24:52
Electroceutical Therapies… 00:32:35
Dr. Ruscio Resources … 00:41:36
Functional Neurology Resources… 00:42:36
Episode Wrap-up … 00:49:04

Download this Episode (right click link and ‘Save As’)
Episode Intro
Dr. Michael Ruscio, DC: Hey Everyone, welcome to Dr. Ruscio Radio. This is Dr. Ruscio. Today I am here with Doctor Titus Chiu and we are discussing the brain-gut connection.
This is one of a multi-part series and the way that we’ve released these actually worked out really well because I feel we’ll get the most granular into direct brain imbalances and brain therapies where our lead-in to the conversations thus far has been more about over-stressed, faulty neural pathways that have been facilitated by being sick or potentially chronically ill and lock you in to this pattern of negative thinking.
DrMR: Ashok Gupta described it as a conditioned defense response and how things like meditation and mindfulness can help steer you out of that and repattern you out of that. So, we’re going to go, what I feel will be, a bit further into some of the particulars around brain and give some more direct brain therapies with more of a neurological bent to it.
But yeah, Titus. Welcome to the show and glad to have you here for part three of the brain-gut connection.
Dr. Titus Chiu: Yeah. Very good to be here. Thanks so much for inviting me, Michael.
DrMR: Absolutely. Tell people about your background, just in brief. Your training and then what you’re doing in the clinic now. I know you’ve written a book on this, so obviously you’ve put some time into the matter. The book is called BrainSAVE and you’re in clinical practice. So, get us to speed on who you are, what you’ve done in terms of training, and what you are doing now.
DrTC: Sure. So, my name’s Dr. Titus Chiu and I’m a function neurologist that specializes in post-concussion syndrome.
My whole story began over twenty years ago, when I was in a really bad car accident. It was so bad… I mean, I am really thankful that I’m here. And so, it was so bad I got hit by a car on the way to work and really busted up my body, broke a few ribs, dislocated my shoulder. Thankfully though, it wasn’t a life-threatening injury and I was able to slowly but surely recuperate or recover from that. But then I ended up with a lot of chronic pain and neck pain. And so, luckily at the time, my brother was actually a chiropractor. After three sessions, he treated me and all this chronic pain just disappeared. It was just mind blowing. And so, from that, it was like my whole world shifted. I thought, I need to learn… I just got so curious. I need to learn how to do that and further improve my health and share it with other people.
And so fast forward, I went to chiropractic school. But then along the way, I discovered neurology and I just fell in love with it because it was such a great framework for understanding what makes us tick. And also, as a clinician, because in chiropractic there are a lot of innovative therapies out there. I’m sure you are very much aware of, Michael, that they’re so innovative. A lot of people ask, “Wow, how does that work?”
Neurology was such a great way of understanding how and then, in understanding how, I could understand why when things didn’t work, I could create more innovative treatments from there. And so, through that whole process, after I discovered neurology, I actually did a whole post doc in clinical neurology. And along the way, I discovered my passion for teaching. And so, I ended up teaching for the institute that I got board certified in. I also was really into functional medicine and nutrition, so I did a master’s in nutrition. I’m really involved with the Institute for Functional Medicine and a lot of their training in that world.
So, the way I approach brain health is really from this holistic standpoint of what’s happening in a person’s physical brain, in their chemical brain, and in their emotional brain. And what I mean by that… and I will be talking about this, as it relates to the brain-gut axis. But in the physical brain, there are specific brain cells and regions and what we call neural networks that actually control everything: our experiences of our self and the world around us. In particular, there are brain-gut neural networks. There are different areas of the nervous system that perceive our gut, we call the insular cortex. And then there’s control pathways from the insular cortex all the way down to the digestive system, the gut itself. And then obviously, there’s also then the gut-brain connection. So, it’s a bidirectional communication pathway.
So, what I mean by physical brain is specifically those checkpoints that connect with other systems of our body such as the brain-gut axis, the brain-immune axis, so on and so forth.
I really dig your work too, because you are exploring it from the gut outwards… How does the gut impact the thyroid? How does the gut impact the immune? I’m then looking at it through a systems biology framework, but then starting more with the nervous system, because like I said, that’s my passion.
And so, in addition to the physical brain, I then look at the chemical brain, that’s a lot to do with the neuro-chemical milieu that our physical brain structure sit in. So, things that influence that are the actual gut-brain connection, as an example. So, systemic inflammation from digestive issues or hidden infections, et cetera, can impact the nervous system in what I call the chemical brain.
And finally, the emotional brain is really how our belief systems, our mindset, can totally transform how our minds and our brains work. Kind of alluding to the whole meditative practices you guys talked about in the previous podcast. So that’s my approach. It’s really a holistic process and approach that I put together called “Root cause Neurology.”
DrMR: Awesome. Love it. And can you tell people a little bit about the kind of typical patient that you see, because I think that’s helpful just to kind of understand the kind of run-of-the-mill case that you are seeing. Are you seeing a lot of people with head trauma? Or do you have a couple different patient categories that you are seeing predominate your practice population?
DrTC: Yeah. Absolutely. So, the majority of patients I work with definitely have obviously neurological, chronic neurological symptoms. They might be struggling with post-concussion syndrome either months or years after their original head injury. That was actually what I went through and learned how to heal my brain and so that’s a big passion of mine.
In addition, I work with a lot of patients who, probably similar to you, are struggling with gut issues.

But a lot of time… Have you ever, you as a clinician, have you found patients you tried the typical gut healing protocols like diet and supplements, you’ve even run the lab tests like the GI map and whatever, ones you run to get a window on the microbiome…. and because a lot of patients I see, even if they don’t have a concussion, they might have been referred to me from another doc because the typical 5-R program, as an example, didn’t work.
And so, I got really confused when I was trying to figure it all out. I would work with a lot of patients over the years. And I’d try the function medicine protocols. I’d even do the more advanced… the neurological treatments with functional neurology. And this small but really significant portion of my patients wouldn’t get better.
And so I was really confused and what I found when I did a deep dive into their histories, two big patterns: Either number one, they had undiagnosed autoimmunity or number two, they had a history of concussion, and so I worked with a lot of patients who’ve been everywhere, tried everything. They’ve been to great functional medicine practitioners. They’ve tried diets and supplements, but still something is missing and what I found in my experiences, especially when we talk about digestive health, there’s actually an imbalance not just in the gut, but actually in the brain-gut connection. And the best way I can give you all an example. Michael, have you ever heard of that term? Phantom Limb Syndrome?
DrMR: Yes.
The Brain-Gut Connection
DrTC: Yeah. So Phantom Limb Syndrome, for those of you out there who haven’t, it’s this really curious syndrome that Doctor Ramachandran talks deeply about in his TED talk. I highly recommend that. But it’s where people, they lose a limb for whatever reason through trauma or surgery, but they still perceive pain in that limb. And so, it completely flipped the whole idea of what pain was. And a lot of people started looking just not in terms of what’s happening in the limb, but what’s happening in the brain that’s actually perceiving that limb. So I’ve taken that idea and I’ve translated into what I call Phantom gut pain syndrome, where the patients that I’ve seen with chronic gut issues, they’ve run the stool tests, they’ve done the diets, they’ve tried eliminating this, they’ve tried AIP, they’ve tested food sensitivities, they’ve even done SIBO protocols and leaky gut protocols with the herbs and everything.
And yet they’re still having symptoms. And not always, but a lot of times, especially if they’re referred to my practice and I do a workup, I identify a breakdown in the brain-gut connection. And one of the key areas of the brain gut axis… Because I know a lot of people are starting to talk about, the brain-gut connection, which is exciting for me. And I’m really excited when I hear people talk about the gut-brain connection. How digestive imbalances can cause neurological symptoms.
But my passion is looking at how neurological, brain-based imbalances can trigger something like a gut imbalance. And there’s a lot of different reasons for it, but there’s, I’m sure you’re familiar with this… There’s certain studies that they’ve looked at using irritable bowel syndrome, this approach to understand the framework where people have had a rectal distension. They’ll do these experiments where they’ll distend someone’s rectum as if they’re having a bowel movement. And they find that some people with irritable bowel syndrome, if they distend that balloon just a little bit, they have a huge reaction to it. And this goes into this concept called Allodynia. It’s this abnormal hypersensitivity to pain, to stimuli that shouldn’t be painful. But you can think of for example like a bowel movement, that really shouldn’t be painful. And so they did these studies…
Detecting a Brain-to-Gut Problem
DrMR: Not to interrupt, but I want to steer us back to, as fascinating as all this is… I want to try to lead with trying to provide the audience with a hierarchical approach, because one of the things I fear is happening right now is… where to integrate brain-based therapies into the functional medicine model is oftentimes not clear.
And so let me just provide how I’m currently thinking about this and then it would be fantastic if you can then follow with where you’d modify that or if there are certain history remarks like concussion history or other indicators, a clinician or a lay person working with the clinician can use to say, okay, if we see X, Y or Z, we’re going to escalate in the hierarchy where the brain-based therapies belong.
DrTC: That’s such a great question. Yeah, thanks for bringing that up.
DrMR: Hang on, let me just leave with kind of how I’m seeing this because I’d like to juxtapose the hierarchy I have in my mind and then let you refine it or modify it.

So, a couple of things I want to say in response to the comments that you make is, I think these are really insightful for clinicians. The 5-R program, it’s often taught, I don’t agree with it. I think it’s backwards in many regards. And so, we have to be careful first with… I do feel there’s a fair number of clinicians who are struggling because they’re using more of a protocol-based treatment algorithm. They’re either using a traditional 5-R model, which I feel like in many respects is actually backwards, or they’re treating lab tests at the expense of treating a patient.
And there are many things that I’ve harped on about. So, there’s a lot for a clinician to gain just by having a better mastery of the available gut tools and using more of a contemporary algorithm as I’ve written about in Healthy Gut, Healthy You and as we’ve talked about in the show. And my observation has been, for many patients, that will get to the resolution that they’re not able to get to otherwise.
If we go through that step one; step one is doing a better job with gut therapies if you understand plainly. So then step two, then they start to look more so at… Okay, do they need more advanced gut therapies like immunoglobulin therapy or some of these other more esoteric or progressive or novel therapies? Or do they strike me as someone with this conditioned defense response, where their mind is just always on overdrive and they are no longer sick but they think they’re sick, and has to be reconditioned to not think they’re sick? So that’s more of the items I put in the secondary consideration.
Another would be a referral for more brain-based therapies where… Has there been a history of concussion or head trauma? Or maybe even physical, sexual or emotional abuse and they need to see a counselor?
So that’s how I look at this hierarchy. And there’s a final point here then I’ll let you come in. But the other thing that I found to be disheartening for some providers is they go through some poorly executed gut therapies and then they just throw out these, “Well, you can gargle to stimulate the vagus nerve, you can gag yourself.” And I haven’t seen a patient yet, while I’m open, who’s reported benefit from doing that. Now I’m certain it works for some people.
But what I think is happening here is there’s not the right qualification for when to use those therapies in a loose hierarchical structure. So, I’m very curious to hear what the hierarchy you see is, how you’d modify my hierarchy and what kind of early indicators might prompt you to move these brain-based therapies higher up in the hierarchy.
DrTC: Yeah, that’s a great question. And Yeah, I like your approach. You go through this whole three-step process where you start with… It’s like you just clear the space and there is a much more innovative approach to gut therapy and then also looking at then the emotional components which plays a huge role. And then, in terms of your question about then looking at it from a brain-based perspective… One of the simplest things is just doing a history. “Have you had a history of a concussion?”
And then the thing with concussions is that I’ve actually experienced myself, you don’t even need necessary a massive blow to the head, like an actual physical injury to your head to experience post-concussion syndrome. Because what actually triggers concussion, the symptoms afterwards, is an immune excitotoxin response, an inflammatory and an excessive toxin response.
And so, there’s people who have… I have patients I’ve worked with where I ask them, “Have you ever had a concussion?” They say, “I don’t know.” And then I dig a little deeper and then they’ll be like, “Oh yeah, actually, a few years ago…” I’m sure you’ve experienced that a lot of the other clinicians out there. But what I’m speaking to is not just reframing the whole idea of what a concussion is. Because if you actually look at the research, you don’t need a physical trauma. So. number one is really honing in, in your history, as any good clinician will do. Right? 90%, 80% of the answers lie there and so…
DrMR: How do you ask that? So, if it’s a non… Okay the person didn’t get knocked out with a frank concussion. How are you teasing that out with the questions that you’re asking a patient?
DrTC: Yeah. So, first of all, it’s part of the intake process. So, when I started discovering what a big epidemic concussions are, I just immediately added to our online intake process. So, we have an online intake form. So, it’s just like have you had a history of a concussion? And so, we start there and then when I need…
DrMR: I’m sorry, it’s just a simple… is that the start or is there a couple of questions survey that researchers are using for concussions? I’m just really… Because I know we’re going to have questions we’re going to have. I’m just trying to…
DrTC: Yeah, we’ll get there. So yeah, we’ll get there. Michael.
DrMR: All right.
DrTC: Well the first step is just when patients are filling out the intake process. We literally have it: Have you had a history of concussion? And then when they actually come in, in the history, if they check anything, I asked them, I go deeper into… Okay, when was that? When did this happen? And then I’ll educate them a bit. Have you ever been in a really bad car accident or had whiplash? It’s like you trace it in the history because if… For example, I’ve worked with a lot of patients who develop autoimmunity after a car accident.
It’s just like, how did that happen? Well, it’s simple. It was the whole traumatic brain injury leading to leaky gut and then creating that whole epigenetic response into an autoimmune condition.
And so, by understanding that, then we can kind of tease it apart. Okay, we got to heal the immune response. We got to balance the gut. But then in addition, we’ve got to do things to rehabilitate the brain. So first it’s the online intake process. And then the second thing is just going deeper into the history. Just really asking and listening to your patients. “Okay, have you been in a really bad car accident?” Or even, “Did you have any head trauma or any forceps injury at birth?” So, I really go with all my patients… I go way deep into their history. So, from there, that’s just a really easy way to see if that someone has, at least subjectively, a history of a concussion or something that could be influencing the brain-gut axis.
Then from there, there’s simple neurological tests that you can do to see. For me when I was a clinician, it’s all about pattern recognition. It’s like, okay, the person has digestive issues… Actually, not even just as a clinician, as a neurologist, as a functional neurologist, in the way I’m trained, the gut is what we call an end organ. Meaning that it’s part of this whole communication pathway from the insular cortex all the way down.
So, for example, as you probably know, treating patients with chronic pain in the past. If someone had a knee injury or pain, it might not have been just the knee that wasn’t working. It could have been the muscles or joints, but of course, it could have also been the peripheral nerves, the spinal cord, the cerebellum and sometimes even up into the brain, like I said.
So, I kind of look at it from that approach. I’m like, okay, what’s the brain-gut axis? What are the checkpoints and what are the patterns that are associated with those functions? So, for example, like I talked about before, the insular cortex, that area of our nervous system, its function is to give us what we call interoception. It’s like an awareness of what’s happening inside. And so they found, again, people with IBS that some of them, not all… Some of them its because they had SIBO or some of them they had stuff going actually going on in their gut. But there was a small percentage that’s actually because it was just a perceptual shift in the insular cortex.
And I find that a lot, Michael, a lot of my patients who have, as an example… I’m kind of painting the picture of pattern recognition. So, say you have a patient or say you’re a listener out there who struggles with bloating and gas and abdominal distension and pain. But in addition to that, you have anxiety and you’re kind of sensitive to the world around you and you also, I don’t know how to explain it… It’s really hard for you to create boundaries for yourself. So, when I hear three or two key areas, what I’m going to investigate is, number one, the gut itself. And I do that through an abdominal exam and stool testing and all different types of testing.
But number two, I’ll also then do a neurological exam exploring, what’s happening in the insular cortex. And the way I can do that… The insular cortex, not only processes what’s happening in your gut, like visceral sensations, whether it’s distension or pain, but it also processes emotions and compassion as well as, and this is where it gets really juicy for clinicians, vestibular sensations, meaning the sensations of movement of our head.
So as an example, if a patient comes to me with all the typical gut symptoms that I described, and then on top of that they were kind of empathic, kind of sensitive, almost like an autoimmune patient, maybe. And in addition to that, they had balance issues or vertigo or dizziness. Bam. One of the key areas that I’m going to hone in on is the insular cortex. And the cool thing is, because it’s a bi-directional pathway, the brain, or the insular cortex, talks to the gut. But then the gut talks back to the brain by way of the vagus nerve and all these other neurological connections. So, when you actually do visceral manipulation therapies… There are different protocols that I do related to the ileocecal valve and the hiatal hernia. Even just a simple belly massage that patients up there might be listening to. That not only helps the belly, it also sends a signal and changes what’s happening in the insular cortex.

The reason why I’m bringing this up is because, what I find is that a lot of patients who then, they hear about meditation, they’re, “Oh I should do this meditation practice.” For example, Vipassana Meditation, it’s all about becoming aware of your breath and your internal…. But guess what, a lot of patients with this type of IBS that I’m describing, their insular cortex is already on fire. So, they do more exercise to bring awareness to their internals. It actually sets them off. And so, I’m not saying meditation isn’t good, but it needs to be prescribed for the right patient. So, for example, for me, when I do meditations that bring awareness to my breath, that really calms me down. But I know a lot of patients, for example, patients who I’ve worked with autoimmunity, when they meditate, they’re, “I just can’t do it, I feel more anxious.” And so, they benefit more from either movement meditations like Tai chi or walking meditation because there’s this more somatosensory type of awareness. Does that make sense?
DrMR: It does. And this is a great example because it’s the specifics that I think are really helpful to try to get further granularity on, so that clinicians and patients would know how to navigate the sea of options that they’re confronted with.
Sponsor Resources
Hey, everyone. I’d like to thank one of my favorite probiotic companies for making this podcast possible, Klaire Labs. Again, Klaire is one of my favorite probiotic companies, which I have used personally and in the clinic. They offer a quality formula in each of the three categories of probiotics, most namely their Ther-Biotic Complete, their Saccharomyces boulardii, and their BioSpora. They even offer specific blends, for example, a post antibiotic formula, a woman’s probiotic, and even an infant-focused formula.
You’ve likely heard me discuss recent findings showing that probiotics can improve mood. One study, a high-quality randomized control trial, was using a Klaire Labs formula, Target gb-X, as in gut brain access. Klaire Labs, I highly recommend their probiotic line.
So, as a follow up on that, certainly it’s fairly common practice for me to see gastrointestinal symptoms plus anxiety plus depression and plus a feeling of being uncoordinated. And all of those can tie back to gut. It’s not to say they always tie back to gut.
By the way, I agree with the belly massage. I think that we don’t always have to go to the full Clear Passage/Wurn Protocol…. For our listeners, it’s a highly-developed, research-validated visceral massage and scar tissue breaking protocol. I’ve seen patients who do well with, even in some cases just like you said, a simple at home abdominal massage.
But back to my probe, which is how are you discerning… Okay, with this person we should do low FODMAP plus some probiotics? Give that some time and see if that knocks out all these symptoms. Or do you just do that first and then if they’re not responding, you’re then going to reach the neurological. How are you going to organize this?
DrTC: That’s a great question and so a big part of it, again, it’s just the whole clinical process, just doing a history. What are the key points? When did that start? When did their symptoms start? Did it start… Did their gut issues start after a head injury? Did they develop SIBO after a head injury or was it like, “Oh I was in India, traveling, and I took these antiparasitic drugs and after that, not only did my gut fall apart, but I developed anxiety and my hair is falling out.” So, for me it’s pretty clear. My first line of investigation for the former would be, “Okay, I’m going to do a neurological evaluation, look at how your eyes move.
Because there are objective findings that are very common in a concussion. We can see slight breakdowns in eye movements, as an example.
Then I might do like vestibular testing related to balance, coordination. And then from there I’ll do a challenge. Meaning I’ll do a neurological challenge where I might have them do a specific eye movement to exercise the area of the brain that I think isn’t working.
And guess what Michael? It’s beautiful, and I’m sure you’ve seen this before. The nervous system gives you that instant feedback where, for example, I do an abdominal exam and I find some gut reflexes or pain. I do a neurological exam and I see some eye ocular-motor imbalances. It’s like their eyes aren’t tracking. And balance issues. And then I find this neurological challenge point, which, and it depends… It really depends on what works for patients, but I’ll do a neurological challenge point, maybe like a specific eye exercise, or I might do an adjustment, or I might have them visualize something. So like a neurological challenge.
And I’ll recheck all those things. I’ll recheck the gut reflex, I’ll recheck balance, I’ll recheck the eye movements. If all those things improve, that’s where I’m going to go. That’s where I am going to put the majority of my energy and education for my patient and be like, hey this is a brain-based thing. This is what we need to do.
Whereas in the second case, if it’s like, “Yeah, after that trip to India I had this horrible, food poisoning and diarrhea. I almost died. I’m anxious now and my balance is horrible. Before that I never had any of those issues.” I’m going to start looking at the digestive system. What’s happening in the microbiome? Is there dysbiosis? Are there infections? So, it’s a pretty straightforward clinical approach, but at the end of the day, it’s putting it to the test.
That’s why I love the neurological challenges because I could put it to the test. They might not be completely resolved for those symptoms, but I can do a simple neurological challenge in a matter of 10 minutes, know that, at least as a first step, this is a good direction to go. And in addition, I probably would then add on a stool test or a breath test or something to explore the gut itself.
Whereas in the second example, I would start probably with a deep dive and do it a cleansing protocol with the gut, run some lab tests and then, if from there… And maybe give them foundational eye exercise or neurological stuff at home, but things that they can do on their own. And then, just see how they respond.
The point of that is, you know as a clinician, it’s all hypothesis. But it’s not like a guess out of thin air. It’s basic science and research and really listening to your patients. And just like you, your clinical experiences throughout the years, we come up with an educated hypothesis and then we put it to the test.
DrMR: Yep. That’s beautifully said, I couldn’t agree with you more.
I just want to quickly repeat a story I told in the podcast probably a year to a year and a half ago, at least, about the late John Donofrio who’s the former…
DrTC: John Donofrio, yeah.

DrMR: He was a mentor to me in my younger years and I traveled with him lecturing at various spots around the country when I was still a student. It was quite an honor to be extended that invitation. What was amazing about working with him and talking about functional medicine, as he was talking about neurology, was watching how he would take people from the audience who had known vestibular disorders. I mean he’d make a display of what this looks like. It’s an educational conference for clinicians and one of the things you can do is with someone with a vestibular disorder, they put their feet together, they close their eyes and they will literally fall over. And we got to have one person standing on each side. Usually I was one of the guys there helping catch someone.
DrTC: Catch them, yeah.
DrMR: …literally fall. You would then be able to go through an assessment, make an adjustment and/or use a laser, and a couple minutes later, that person would be able to repeat the same test and not fall over. So, I mean, that really opened my eyes to the power of neurology. So, I just want to throw that out there for the audience that if some of this sounds unfamiliar to you, I’ve seen the results firsthand with my own eyes.
DrTC: Yeah, Dr Donofrio he was just a living legend, totally. Thanks for sharing that story. And that’s kind of giving a context for our listeners. So that’s how I approach it.
Electroceutical Therapies
One thing I do want to touch on that you mentioned earlier, because on blogs and in certain books people talk about, ‘Oh, activate the vagus; You can gargle.” Kind of like what you mentioned before. And then not see any changes. It could be several things. Whenever I think about its either, number one, “Yeah, it’s not the brain gut axis.” Or it’s not the brain stem pathway that needs it. It might be the insular cortex. Or maybe the brain is really not involved in that case. Maybe the brain, any brain symptoms are as a consequence of gut dysfunction, first and foremost. Right?
But the other reason why something might not work like that is because the intensity wasn’t strong enough. And this is something that is so exciting to me these days. It’s this concept of electroceuticals. Which I think is like the future of medicine.

You’re probably familiar with the term pharmaceuticals, which is drug-based treatments. And then nutraceuticals, using concentrated nutrients found in nature, but then putting into a jam-packed supplement, right? What I’m talking about are electroceuticals, where there are ways of gently and not invasively activating the brain and, for example, the brain-gut axis using electricity. And so, I do this a lot in my practice.
As an example or an analogy, and I’m sure a lot of clinicians, and maybe even you, Michael… I love nutrition. It’s not only as a clinician but as a foodie. And I also know that sometimes diet alone will not cut it. We might need nutraceuticals, we might even need more powerful herbs and maybe sometimes it’s some situations, medications. So, I kind of see that as the spectrum, right? You have food as medicine, but then in deeper imbalances we might have to resort to immunotherapy or medications, stuff we kind of alluded to earlier.
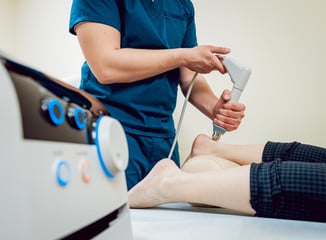
That’s the same thing when it comes to brain-based therapies. We can rub the belly, which will activate the vagus nerve and the nucleus tractus solitarius and the insular cortex. But that might not be enough. So, in my practice if I think that’s the case, if there’s a deeper neural network imbalance, I actually use these noninvasive… They’re like medical devices that send pulses of electric energy along cranial nerve pathways or peripheral neural pathways.
So as an example, kind of riffing off of what you’re talking about with Dr Donofrio, I had a patient who I am a hundred… She just came to the office just recently. I’m 110% sure that a lot of her symptoms both digestive, emotional as well as her pain sensitivity is the insular cortex. And so, I did a Romberg’s. And for those of you out there who aren’t clinicians, I had her stand up, put her feet together and look straight ahead, because I’m looking at her balance. And she was okay. But then when I had her close her eyes, she nearly fell over. She closed her eyes and the tables, right to her left, she fell into the left. And if it wasn’t for the table she would have fallen on the floor. You weren’t there to help us, Michael, that would have been great.
But anyways, so she almost fell. I already had a hypothesis in my mind after the intake and the history. I had a feeling there was something going on in the insular cortex. Because she had a lot of wandering pain issues, not only in her gut but also throughout her body. And she had a lot of anxiety. And so, I just put it to the test. I was just thinking, okay, because in her… well, I won’t go too in depth with her history out of privacy issues. But yeah, I had a feeling that there was definitely some type of trauma early on related to the brain. So then, I would formulate this hypothesis. I had her stand up, put her feet together into this Romberg’s. She was okay. Close your eyes and she almost fell over.
And so, okay, this is huge. Because then we had a window, we had something to work with. So then, I had her take this electroceutical device that I use. It’s these headphones that she wears along her ear. It doesn’t sit in her ear. It sits right in front of her ear. And then I had it hooked up to this application. It’s just a simple iPhone application and it pulses these frequencies of sound. But these type of headphones are actually bone conducting. So, the majority of the signal is not auditory. It’s actually vibration and it… What it does is it triggers the cranial nerve pathway. We call the trigeminal nerve as well as the vestibulocochlear nerve. And so, that is the direct window into, guess where? The brainstem. The nucleus tractus solitarius. And all these different areas relate to the brain-gut connection.
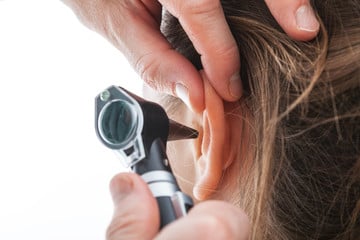
So, I had that pulsing in her left ear because some of my other exam findings. And I had her, this is literally one second later… I’m like, okay, stand up, put these on. I press play on the electroceutical device. Stand there. And she closed her eyes. She did not waver at all. Her mom was in the room, she’s like, “What?” But to me as a clinician, and you know this, it’s like when you nailed it, you’re just, “Yes! This person’s life is going to dramatically change with some simple things that she can do.”
But I can almost guarantee you, because there’s… For example, when we talk about gagging or gargling, That activates a different cranial nerve pathway, which is the cranial nerve 10, the vagus nerve.
Whereas this auditory-vibratory pathway activated both the trigeminal as well as the vestibulocochlear nerves. So, we can get so specific as to which parts of the brainstem and the brain-gut axis we want to activate. And if I had just sat her in a chair and spun her around to the left, which is a natural way of activating this nerve, just like if I had her gargle or had another patient gargle, it might have not had a dramatic effect, because the dosing wasn’t enough.
Just like if you say, “Hey, go eat some broccoli.” And this person has Parkinson’s. “Eat some blueberries.” Maybe over the course of 50, 60 years it’ll do its trick. But right now, there’s other things we can do like nutraceuticals to increase the dosage in a safe way. It’s the same thing for brain-based therapies. So, I incorporate a lot of electroceutical therapies in my practice. I can activate the trigeminal nerve to help people with chronic neck pain and jaw pain and headaches. I can activate the vagus nerve to help people with chronic digestive issues or who are stuck in that fight or flight response or who have insomnia. I can activate the vestibulocochlear nerve for people who might have had a concussion and feel dizzy and have vertigo and motion sickness. You know, as a clinician, we have to personalize it and we have to make it so specific. Not just, “Okay, why don’t you try eating some broccoli and sipping on some green tea.”
Now that’s a foundational approach that we definitely need. But in addition, for deeper imbalances, there are technologies that are safe. There’s a lot of research looking into the electroceuticals.
And one last thing about this… I just want to make a note, because I know your passion is all about the gut and, outside of that, the autoimmune/immune system. I highly recommend, there’s actually the Scientific American article out there. It’s not, obviously, the most scientific journal, but it’s a great way for people, clinicians as well as patients out there listening… There’s, I’m pretty sure it’s like a shock therapy or shock medicine. But it’s all about electromedicine. And the exciting thing is, because just like the gut is connected to everything, the brain is connected to everything. And a lot of these electroceuticals that they’re using to target these nerve pathways, they’re using it to activate cytokine release. And you’re looking to decrease inflammation. They’re actually using it, some of these studies and researchers, are looking at using this type of therapy for rheumatoid arthritis, because it’s an inflammatory autoimmune condition. But by harnessing the power of our nervous system to then help regulate everything. It’s a super exciting field and I’m so excited to be a part of it and also just continue to learn about research.
DrMR: Yeah. I mean these things are fascinating. Those experiences early in my career were supremely eye-opening.
View Dr. Ruscio’s Additional Resources
Functional Neurology Resources
And that begs the question, if people are trying to get help in this area, obviously there’s your office. And I’ll ask you for whatever website here in a moment. But outside of that, if they’re trying to find someone locally who can do these assessments, do you have a particular body people go through? And/or how much of this can they get from your book?
DrTC: So yeah, that’s a great question. There are a lot of functional neurologists out there. And this is our… Almost every functional neurologists I’ve met, just like Dr Donofrio, we’re like total passionate nerds. A lot of people dive into the specifics of this. If you just Google functional neurologist, and then you, if you’re in the Midwest, your city. You’re going to come up with some people. Now I don’t know them personally necessarily, but that’s a good place to start. Whether they use electroceuticals or not, I’m not sure. You just have to ask.
In terms of, in my book, I actually go through at the end of the book, actually even before the end of the book, in chapter, I believe it’s five, there are what I call the Top Five BrainSAVE Neural Networks. And it’s pretty cool.
It’s like a little quiz you can take to identify, for example, if you have symptoms… If you’ve had a concussion, but even if you haven’t, it’s the same kind of idea. It’s looking at which areas of your nervous system might be contributing to your symptoms. So, for example, I mentioned the vestibular system, there’s a little quiz in there that you can take. Okay, do you have motion sickness? And is it, none, mild, moderate, severe? And you grade it. And then do you have symptoms when you’re reading a screen? Mild, moderate, severe? And you just add it all up. It’ll give you an idea of which areas of your nervous system might be playing a part in your gut dysfunction or your concussion symptoms.
DrMR: That’s great.
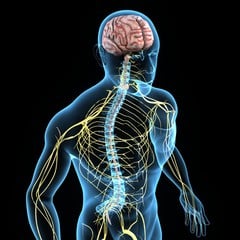
DrTC: Yeah. Then they have a little map, a brain map, of what’s going on in the nervous system. Even if they don’t have a concussion, a lot of people I know have these slight and imbalances that could be impeding their quality of life. And so, from there at the end of the book, I have a six-week plan that then talks about… Week three of the six-week plan is all about using brain-based therapies to start rehabilitating and exercising those areas. So that’s a good start.
One of my passions, my deepest passion… I love working with patients, but my deepest passion is education and teaching people how to take control of their own health. I think we share a very similar approach to that. And so, I’m always in the process of creating new resources because when I had a concussion, even though I was in the functional neurology community, there wasn’t that much out there at the time.
And so, I had to go to seminars. I had to read, research on my own, articles and books and drawing from eastern practices, meditative practices, functional neurology, all this stuff.
And so, my point is, I’m really passionate about creating resources that are really accessible for people, so then they can at least get the whole healing process started. So yeah, if people are more interested, they could go to my website brainsave.com and there’s… I’m always posting, I have a blog on there, and I always… Whenever I create more resources, I’m always talking about different ways and things that people can do to take control of their own brain health.
DrMR: Awesome. I love it. So, there you have it folks. You can search for a neurologist near you. You can check out Dr Titus’ book BrainSAVE. Check out his office. And I guess quickly, on the functional neurologist… I’m assuming that’s your springboard, but then you want to read up on them a little bit, see what they have on their website, check out some of their reviews and do a little bit of due diligence and not just blindly say any functional neurologists is going to be great. You know, obviously there’s going to be, I’m assuming variability with who’s…
DrTC: Yeah.
DrMR: Yeah okay.
DrTC: Absolutely. Yeah. Reach out to anyone. If you find people in your area or in your city, just reach out to them, shoot them an email and give them a call. Tell them what you’re hoping to achieve and see if it’ll be a good fit. But I really think function neurology is this kind of hidden gem in the world. It’s such a beautiful marriage of the functional medicine approach and the gut healing approach and then looking at the brain and how all that fits together. So, yeah, I highly recommend if you guys have been struggling with a concussion or chronic symptoms that you can’t figure out, it could be part of a brain-based issue.
DrMR: Awesome. Well I think you’ve done a great job fielding this topic and admittedly it was a challenge to try to find someone who didn’t seem, if I’m being fully candid here, didn’t seem to have just drank in the entire bottle of neurology Kool-aid. Because some just seemed like it was all neurology all the time.
DrTC: Oh no, yeah.
DrMR: And that ability to look at these things in a bit more nuanced of a light was challenging. And again, I’m sure there’s a lot of great people out there doing this, but sometimes it’s harder to find those people on the Internet than you would initially have thought. So, it was a bit of a challenge.

But I’m glad that we landed on your name because I think you’ve done an excellent job of laying this out, helping people to understand the context of where this fits in the hierarchy, some key indicators that would increase the probability that they need direct brain therapies. And then pointing them towards some great resources, like your book, to get started if they didn’t have the resources to go right to a doctor and they wanted to have a low hurdle on-ramp. So overall this has been fantastic, Titus. I really appreciate it.
DrTC: Yeah, absolutely. Michael. Yeah, it’s, at the end of the day for me it’s about the patients. It’s about our health. It’s like if spinning in a chair and listening to Bon Jovi will do the trick, then do it! If a hardcore gut healing protocol will improve your life and make huge changes. That’s what it’s all about.
DrMR: Yup. And you’re located in Berkeley, correct?
DrTC: Yeah.
DrMR: Okay. Just for people who are trying to figure out regionality.
Episode Wrap Up
Cool. Well anything you want to leave people with as we close?
DrTC: Yeah, that’s really it. When it comes to your health, it’s really, it’s such a personal matter. I even, I tell a lot of my patients, it doesn’t even matter what I say. I can have ideas and theories, but at the end of the day, it’s what really sticks and works with you. And I really encourage everyone out there, if you are struggling with health issues, don’t give up. There are answers out there. It might not be from me. It might not be from other sources, but there definitely are answers out there.
And yeah, I really appreciate you inviting me. I mean, we got to hang out. We’re pretty close, so we should do a dinner sometime and just continue to geek out.
DrMR: Yeah, we’ll make it happen.
DrTC: Thank you so much, Michael.
DrMR: Thank you Titus. Take care.
Dr. Michael Ruscio is a DC, natural health provider, researcher, and clinician. He serves as an Adjunct Professor at the University of Bridgeport and has published numerous papers in scientific journals as well as the book Healthy Gut, Healthy You. He also founded the Ruscio Institute of Functional Health, where he helps patients with a wide range of GI conditions and serves as the Head of Research.




Discussion
I care about answering your questions and sharing my knowledge with you. Leave a comment or connect with me on social media asking any health question you may have and I just might incorporate it into our next listener questions podcast episode just for you!