How To Use Leaky Gut Supplements To Target Inflammation
The Connection Between Leaky Gut and Inflammation
- What Is Leaky Gut?|
- What Causes Leaky Gut?|
- How Is It Diagnosed?|
- Leaky Gut Supplements|
- Anti-Inflammatory Supplements|
- Lifestyle Changes|
- Bottom Line|
Many people consider leaky gut syndrome, a common term for when holes form in the lining of the small intestine, a mere digestive disorder. However, leaky gut may be less about digestion and more likely a result of long-term inflammation promoted by chronic illness, excess weight, poor dietary choices 1, extreme exercise (looking at you, marathon runners and triathletes) 2, and too many non-steroidal anti-inflammatory drugs (NSAIDs), such as ibuprofen 3 4. However, leaky gut supplements may be able to help.
As I’ve emphasized in my book, Healthy Gut Healthy You, the digestive system is probably the main source of inflammation in the body 5. Ergo, the best way to treat and prevent leaky gut may be reducing overall inflammation through a combination of supplements, diet, stress reduction techniques, and moderate exercise.
In this article, we’ll explore the most well-researched supplements for leaky gut, including l-glutamine, probiotics, colostrum, zinc, and zeolite. We’ll also look at other supplements and therapies that can reduce the burden of gut inflammation.

What Is Leaky Gut?
Also called intestinal permeability or gut hyper-permeability, leaky gut syndrome is what happens when the tight junctions — membranes that lock the cells lining your small intestine together to keep its contents inside — come loose. As a result, undigested food particles and bacteria can sneak past the intestinal wall and get into the bloodstream, where they don’t belong.
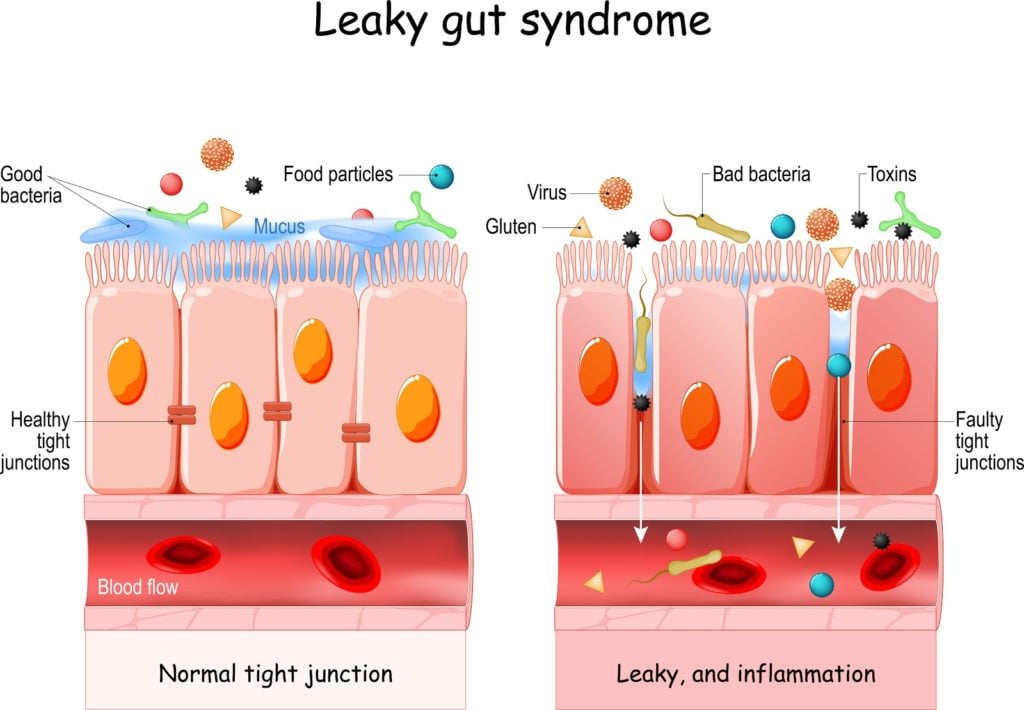
When this happens, foreign molecules in the blood trigger an immune response (inflammation) and an increase in zonulin, a protein thought to guard the small intestine against invasive organisms 6 7. In fact, high levels of zonulin in the small intestine are considered a sign of leaky gut and may be associated with an increased risk of autoimmunity 8.
The longer leaky gut goes on, the more likely it is to contribute to a vicious inflammatory cycle that can affect other organs throughout the body, giving rise to more inflammation and worsening intestinal permeability 9.
What Causes Leaky Gut?
Healthcare professionals have long assumed that leaky gut goes hand-in-hand with digestive issues. But new, high-quality research that analyzed many studies of intestinal permeability found that digestive symptoms were not actually correlated with leaky gut in most adults 10.
This research found that the issues most strongly associated with leaky gut are 11:
- Inflammation
- Metabolic issues
- High concentrations of lipids (triglycerides or cholesterol) in the blood
- High blood sugar
- Overweight/obesity
- Metabolic syndrome
- Chronic conditions, such as:
- Liver disease
- Diabetes
- Kidney disease
- Polycystic ovarian syndrome (PCOS)
- Celiac disease and other autoimmune diseases, such as inflammatory bowel disease (IBD)
- Eating a Western diet (low in nutrients but high in sugar, processed ingredients, and alcohol) that supports the wrong kinds of gut bacteria.
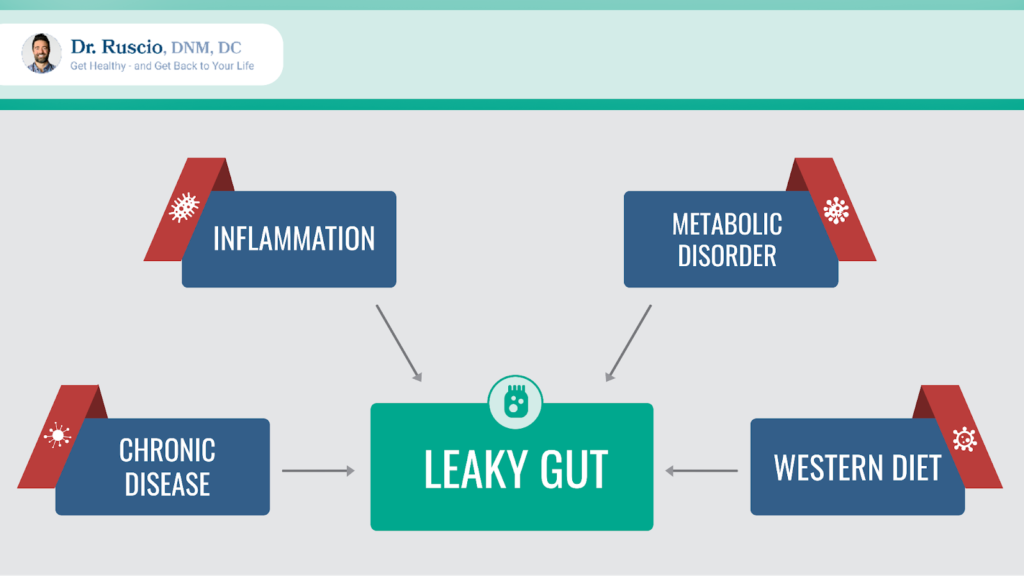
The study also found that, unless you have a diagnosable condition inflaming your GI tract (think IBD, IBS with diarrhea, dysbiosis, disease-related diarrhea, or indigestion), symptoms like bloating, cramping, pain, heartburn, reflux, nausea, and gas are probably not signs of leaky gut 12.
In other words, leaky gut may be a characteristic of chronic disease in general, rather than being specifically linked to gut conditions. However, chronic digestive issues may give rise to chronic inflammation, which is highly correlated with leaky gut 13.
Other studies have found that an overuse of NSAIDs, like ibuprofen 14 15, and very long, intense exercise that raises body temperature to 102.2 F 16 may directly cause leaky gut.
Overall, the above risk factors have an inflammatory effect, which appears to be closely linked to developing leaky gut.
How Do You Know If You Have Leaky Gut?
If you suspect you may be at risk of developing leaky gut, you can ask a healthcare professional about the dual sugar test and serum zonulin test 17. There is no “gold standard” of testing for leaky gut 18 19, but a combination of these two tests could provide clinically useful information.
1. The dual sugar test: Lactulose in your urine signals that your gut is probably leaky.
- This test involves fasting overnight and then drinking a mixture of two types of sugars — often, mannitol and lactulose — before collecting your urine.
- If your intestinal lining is healthy, the mannitol should be absorbed by the small intestine and later appear in your urine.
- The lactulose, which is larger, should stay inside the intestine and never reach the urine.
- The effectiveness of this test is limited by the uncertainty of normal values and a lack of standardization 20. Furthermore, small intestinal bacterial overgrowth (SIBO) may falsify the results 21, so combining this test with serum zonulin may strengthen its conclusions.
2. Serum zonulin: High zonulin may be a good clinical indicator of leaky gut, especially when measured in blood rather than stool 22.
- Zonulin levels also rise with overweight/obesity, high blood pressure, high blood sugar, high triglycerides, high cholesterol, and autoimmunity 23, so it’s harder to be certain that elevated levels specifically indicate leaky gut.
- This is another reason why combining serum zonulin with the dual sugar test may be useful.
Unfortunately, leaky gut testing is time-consuming, imperfect, and expensive, and I don’t recommend it. That said, if you have one or more of the factors that may contribute to leaky gut, you could choose to take simple steps, including certain supplements and lifestyle changes, to lower inflammation and heal your gut lining.
Leaky Gut Supplements
The following supplements have the most high-quality research examining their potential to directly heal leaky gut:
L-glutamine
Multiple studies have found that L-glutamine supplements normalize gut wall integrity in the following types of people:
- Patients with leaky gut and diarrhea-predominant IBS 24
- Active men who exercise hard in the heat 25
- Critically ill patients 26
- Patients on long-term radiation therapy 27
- Patients with HIV/AIDS 28
- Patients with Crohn’s disease 29
Although bone broth hasn’t been clinically researched much, it is a whole-food source for L-glutamine, other amino acids, and minerals that may benefit the gut lining 30. Given its lower concentrations of healing properties, bone broth may also pack a lighter punch than supplements.
Probiotics
A large body of research shows that probiotics may be effective at reducing zonulin and preventing or repairing leaky gut.
- A recent high-quality study found that probiotic supplements reduced serum zonulin, an indicator of leaky gut 31.
- Many recent, high-quality clinical studies found various probiotic microorganisms, such as Bifidobacterium longum, B. animalis, and Lactobacillus rhamnosus, restored intestinal barrier function and reduced intestinal permeability in IBS patients, overweight and obese adults, and colon cancer patients 32 33 34 35 36 37.
- For marathon runners and triathletes, another study found that a probiotic strain called Lactobacillus salivarus, which is native to human intestines, protected against exercise-induced leaky gut 38.
- And if you prefer to get your probiotics from food, another study found that supplementing with kefir improved serum zonulin levels in overweight adults 39. Keep in mind that the probiotics in food come in smaller doses than in supplements and may be less therapeutic.
However, there is some controversy regarding probiotics and leaky gut. A number of other high-quality studies found that probiotics did not regularly improve intestinal permeability 40 41 42 43 44 45 46 47, even when the probiotics helped with SIBO and related symptoms 48 or reduced GI symptoms 49.
Unfortunately, leaky gut research is confounded by a number of factors, primarily the lack of quality ways to measure its occurrence or severity. However, most research points to leaky gut as a result of inflammation—much of which starts in the gut—and probiotics have repeatedly been found to reduce gut inflammation.
So, as long as the probiotics you use are high in quality and contain well-studied strains of good bacteria, taking them along with a healthy diet and other anti-inflammatory lifestyle approaches will likely help reduce inflammation and help to improve the integrity of your gut wall.
Colostrum
Research shows that bovine colostrum (the first milk produced after a calf is born) may improve leaky gut and reduce zonulin levels in competitive athletes 50 51.
Zinc
Low-dose zinc supplementation may improve leaky gut in children with inflamed digestive tracts 52, and zinc carnosine (a mineral-amino acid compound) may increase gut lining strength in active adult men who exercise heavily 53.
Zeolite
Zeolite, a collection of silica-based minerals that naturally come from volcanoes, may improve intestinal wall strength in endurance athletes by reducing zonulin levels 54.
Other Supplements With Anti-Inflammatory Health Benefits
Although the following supplements haven’t been rigorously tested for their direct effects on leaky gut, they have been found in some studies to reduce inflammation and/or support gut healing.
- Vitamin D 55
- Digestive enzymes 56 57 58
- DGL (deglycyrrhizinated licorice root) 59
- Aloe vera 60
- Quercetin 61
- Fish oil 62
- Immunoglobulins 63
- Collagen 64
How To Use Lifestyle Changes To Heal Leaky Gut
Leaky gut is a condition that’s very much influenced by your lifestyle choices. While supplements can play an important role in the healing process, don’t overlook the importance of these lifestyle choices:
- Eat a balanced, nutrient-dense diet low in inflammatory foods, such as the paleo diet. You may need to figure out your best diet by temporarily removing foods that may trigger your immune system, such as gluten, dairy, eggs, FODMAPs, or nuts. Reintroduce these foods one at a time to see if you react to them.
- Limit sugar, and keep carb intake to whole foods like fruits, vegetables, and grains that your digestive system tolerates well.
- Exercise regularly but moderately – don’t overdo it.
- Practice breathing exercises and meditation to reduce stress and support your nervous system.
- If you have a chronic condition, get help from a healthcare professional who is aware of the roles the gut microbiome and digestive health may play in your condition.
The Bottom Line on Leaky Gut and Inflammation
Overall, leaky gut syndrome seems to both result from and contribute to chronic inflammation. To reduce inflammation and thereby lower your risk for leaky gut, I recommend research-backed leaky gut supplements and incorporating lifestyle changes that support your gut health and immune system.
For help with healing leaky gut, schedule an appointment at the Ruscio Institute for Functional Health.
Dr. Michael Ruscio is a DC, natural health provider, researcher, and clinician. He serves as an Adjunct Professor at the University of Bridgeport and has published numerous papers in scientific journals as well as the book Healthy Gut, Healthy You. He also founded the Ruscio Institute of Functional Health, where he helps patients with a wide range of GI conditions and serves as the Head of Research.➕ References
- Leech B, McIntyre E, Steel A, Sibbritt D. Risk factors associated with intestinal permeability in an adult population: A systematic review. Int J Clin Pract. 2019 Oct;73(10):e13385. doi: 10.1111/ijcp.13385. Epub 2019 Jul 5. PMID: 31243854.
- Pires W, Veneroso CE, Wanner SP, Pacheco DAS, Vaz GC, Amorim FT, Tonoli C, Soares DD, Coimbra CC. Association Between Exercise-Induced Hyperthermia and Intestinal Permeability: A Systematic Review. Sports Med. 2017 Jul;47(7):1389-1403. doi: 10.1007/s40279-016-0654-2. PMID: 27943148.
- Bjarnason I, Hayllar J, MacPherson AJ, Russell AS. Side effects of nonsteroidal anti-inflammatory drugs on the small and large intestine in humans. Gastroenterology. 1993 Jun;104(6):1832-47. doi: 10.1016/0016-5085(93)90667-2. PMID: 8500743.
- Mujagic Z, de Vos P, Boekschoten MV, Govers C, Pieters HH, de Wit NJ, Bron PA, Masclee AA, Troost FJ. The effects of Lactobacillus plantarum on small intestinal barrier function and mucosal gene transcription; a randomized double-blind placebo controlled trial. Sci Rep. 2017 Jan 3;7:40128. doi: 10.1038/srep40128. PMID: 28045137; PMCID: PMC5206730.
- https://store.drruscio.com/products/healthy-gut-healthy-you
- Leech B, McIntyre E, Steel A, Sibbritt D. Risk factors associated with intestinal permeability in an adult population: A systematic review. Int J Clin Pract. 2019 Oct;73(10):e13385. doi: 10.1111/ijcp.13385. Epub 2019 Jul 5. PMID: 31243854.
- Ramezani Ahmadi A, Sadeghian M, Alipour M, Ahmadi Taheri S, Rahmani S, Abbasnezhad A. The Effects of Probiotic/Synbiotic on Serum Level of Zonulin as a Biomarker of Intestinal Permeability: A Systematic Review and Meta-Analysis. Iran J Public Health. 2020 Jul;49(7):1222-1231. doi: 10.18502/ijph.v49i7.3575. PMID: 33083288; PMCID: PMC7548501.
- Ramezani Ahmadi A, Sadeghian M, Alipour M, Ahmadi Taheri S, Rahmani S, Abbasnezhad A. The Effects of Probiotic/Synbiotic on Serum Level of Zonulin as a Biomarker of Intestinal Permeability: A Systematic Review and Meta-Analysis. Iran J Public Health. 2020 Jul;49(7):1222-1231. doi: 10.18502/ijph.v49i7.3575. PMID: 33083288; PMCID: PMC7548501.
- Leech B, McIntyre E, Steel A, Sibbritt D. Risk factors associated with intestinal permeability in an adult population: A systematic review. Int J Clin Pract. 2019 Oct;73(10):e13385. doi: 10.1111/ijcp.13385. Epub 2019 Jul 5. PMID: 31243854.
- Leech B, McIntyre E, Steel A, Sibbritt D. Risk factors associated with intestinal permeability in an adult population: A systematic review. Int J Clin Pract. 2019 Oct;73(10):e13385. doi: 10.1111/ijcp.13385. Epub 2019 Jul 5. PMID: 31243854.
- Leech B, McIntyre E, Steel A, Sibbritt D. Risk factors associated with intestinal permeability in an adult population: A systematic review. Int J Clin Pract. 2019 Oct;73(10):e13385. doi: 10.1111/ijcp.13385. Epub 2019 Jul 5. PMID: 31243854.
- Leech B, McIntyre E, Steel A, Sibbritt D. Risk factors associated with intestinal permeability in an adult population: A systematic review. Int J Clin Pract. 2019 Oct;73(10):e13385. doi: 10.1111/ijcp.13385. Epub 2019 Jul 5. PMID: 31243854.
- Leech B, McIntyre E, Steel A, Sibbritt D. Risk factors associated with intestinal permeability in an adult population: A systematic review. Int J Clin Pract. 2019 Oct;73(10):e13385. doi: 10.1111/ijcp.13385. Epub 2019 Jul 5. PMID: 31243854.
- Bjarnason I, Hayllar J, MacPherson AJ, Russell AS. Side effects of nonsteroidal anti-inflammatory drugs on the small and large intestine in humans. Gastroenterology. 1993 Jun;104(6):1832-47. doi: 10.1016/0016-5085(93)90667-2. PMID: 8500743.
- Mujagic Z, de Vos P, Boekschoten MV, Govers C, Pieters HH, de Wit NJ, Bron PA, Masclee AA, Troost FJ. The effects of Lactobacillus plantarum on small intestinal barrier function and mucosal gene transcription; a randomized double-blind placebo controlled trial. Sci Rep. 2017 Jan 3;7:40128. doi: 10.1038/srep40128. PMID: 28045137; PMCID: PMC5206730.
- Pires W, Veneroso CE, Wanner SP, Pacheco DAS, Vaz GC, Amorim FT, Tonoli C, Soares DD, Coimbra CC. Association Between Exercise-Induced Hyperthermia and Intestinal Permeability: A Systematic Review. Sports Med. 2017 Jul;47(7):1389-1403. doi: 10.1007/s40279-016-0654-2. PMID: 27943148.
- Leech B, McIntyre E, Steel A, Sibbritt D. Risk factors associated with intestinal permeability in an adult population: A systematic review. Int J Clin Pract. 2019 Oct;73(10):e13385. doi: 10.1111/ijcp.13385. Epub 2019 Jul 5. PMID: 31243854.
- Leech B, McIntyre E, Steel A, Sibbritt D. Risk factors associated with intestinal permeability in an adult population: A systematic review. Int J Clin Pract. 2019 Oct;73(10):e13385. doi: 10.1111/ijcp.13385. Epub 2019 Jul 5. PMID: 31243854.
- Camilleri M. Leaky gut: mechanisms, measurement and clinical implications in humans. Gut. 2019 Aug;68(8):1516-1526. doi: 10.1136/gutjnl-2019-318427. Epub 2019 May 10. PMID: 31076401; PMCID: PMC6790068.
- Camilleri M. Leaky gut: mechanisms, measurement and clinical implications in humans. Gut. 2019 Aug;68(8):1516-1526. doi: 10.1136/gutjnl-2019-318427. Epub 2019 May 10. PMID: 31076401; PMCID: PMC6790068.
- Rumessen JJ. Strategier ved udredning af malassimilation. En kritisk status [Strategies for investigating non-assimilation. A critical status]. Ugeskr Laeger. 1997 Apr 14;159(16):2356-63. Danish. PMID: 9163110.
- Ramezani Ahmadi A, Sadeghian M, Alipour M, Ahmadi Taheri S, Rahmani S, Abbasnezhad A. The Effects of Probiotic/Synbiotic on Serum Level of Zonulin as a Biomarker of Intestinal Permeability: A Systematic Review and Meta-Analysis. Iran J Public Health. 2020 Jul;49(7):1222-1231. doi: 10.18502/ijph.v49i7.3575. PMID: 33083288; PMCID: PMC7548501.
- Ohlsson B, Orho-Melander M, Nilsson PM. Higher Levels of Serum Zonulin May Rather Be Associated with Increased Risk of Obesity and Hyperlipidemia, Than with Gastrointestinal Symptoms or Disease Manifestations. Int J Mol Sci. 2017 Mar 8;18(3):582. doi: 10.3390/ijms18030582. PMID: 28282855; PMCID: PMC5372598.
- Zhou Q, Verne ML, Fields JZ, Lefante JJ, Basra S, Salameh H, Verne GN. Randomised placebo-controlled trial of dietary glutamine supplements for postinfectious irritable bowel syndrome. Gut. 2019 Jun;68(6):996-1002. doi: 10.1136/gutjnl-2017-315136. Epub 2018 Aug 14. PMID: 30108163.
- Pugh JN, Sage S, Hutson M, Doran DA, Fleming SC, Highton J, Morton JP, Close GL. Glutamine supplementation reduces markers of intestinal permeability during running in the heat in a dose-dependent manner. Eur J Appl Physiol. 2017 Dec;117(12):2569-2577. doi: 10.1007/s00421-017-3744-4. Epub 2017 Oct 20. PMID: 29058112; PMCID: PMC5694515.
- Mottaghi A, Yeganeh MZ, Golzarand M, Jambarsang S, Mirmiran P. Efficacy of glutamine-enriched enteral feeding formulae in critically ill patients: a systematic review and meta-analysis of randomized controlled trials. Asia Pac J Clin Nutr. 2016;25(3):504-12. doi: 10.6133/apjcn.092015.24. PMID: 27440684.
- Yao D, Zheng L, Wang J, Guo M, Yin J, Li Y. Perioperative Alanyl-Glutamine-Supplemented Parenteral Nutrition in Chronic Radiation Enteritis Patients With Surgical Intestinal Obstruction: A Prospective, Randomized, Controlled Study. Nutr Clin Pract. 2016 Apr;31(2):250-6. doi: 10.1177/0884533615591601. Epub 2015 Jun 15. PMID: 26078286.
- Leite RD, Lima NL, Leite CA, Farhat CK, Guerrant RL, Lima AA. Improvement of intestinal permeability with alanyl-glutamine in HIV patients: a randomized, double blinded, placebo-controlled clinical trial. Arq Gastroenterol. 2013 Jan-Mar;50(1):56-63. doi: 10.1590/s0004-28032013000100011. PMID: 23657308.
- Benjamin J, Makharia G, Ahuja V, Anand Rajan KD, Kalaivani M, Gupta SD, Joshi YK. Glutamine and whey protein improve intestinal permeability and morphology in patients with Crohn’s disease: a randomized controlled trial. Dig Dis Sci. 2012 Apr;57(4):1000-12. doi: 10.1007/s10620-011-1947-9. Epub 2011 Oct 26. PMID: 22038507.
- https://drruscio.com/bone-broth-diet/
- Ramezani Ahmadi A, Sadeghian M, Alipour M, Ahmadi Taheri S, Rahmani S, Abbasnezhad A. The Effects of Probiotic/Synbiotic on Serum Level of Zonulin as a Biomarker of Intestinal Permeability: A Systematic Review and Meta-Analysis. Iran J Public Health. 2020 Jul;49(7):1222-1231. doi: 10.18502/ijph.v49i7.3575. PMID: 33083288; PMCID: PMC7548501.
- Bonfrate L, Di Palo DM, Celano G, Albert A, Vitellio P, De Angelis M, Gobbetti M, Portincasa P. Effects of Bifidobacterium longum BB536 and Lactobacillus rhamnosus HN001 in IBS patients. Eur J Clin Invest. 2020 Mar;50(3):e13201. doi: 10.1111/eci.13201. Epub 2020 Feb 12. PMID: 31960952.
- Francavilla R, Miniello V, Magistà AM, De Canio A, Bucci N, Gagliardi F, Lionetti E, Castellaneta S, Polimeno L, Peccarisi L, Indrio F, Cavallo L. A randomized controlled trial of Lactobacillus GG in children with functional abdominal pain. Pediatrics. 2010 Dec;126(6):e1445-52. doi: 10.1542/peds.2010-0467. Epub 2010 Nov 15. PMID: 21078735.
- Stenman LK, Lehtinen MJ, Meland N, Christensen JE, Yeung N, Saarinen MT, Courtney M, Burcelin R, Lähdeaho ML, Linros J, Apter D, Scheinin M, Kloster Smerud H, Rissanen A, Lahtinen S. Probiotic With or Without Fiber Controls Body Fat Mass, Associated With Serum Zonulin, in Overweight and Obese Adults-Randomized Controlled Trial. EBioMedicine. 2016 Nov;13:190-200. doi: 10.1016/j.ebiom.2016.10.036. Epub 2016 Oct 26. PMID: 27810310; PMCID: PMC5264483.
- Liu Z, Qin H, Yang Z, Xia Y, Liu W, Yang J, Jiang Y, Zhang H, Yang Z, Wang Y, Zheng Q. Randomised clinical trial: the effects of perioperative probiotic treatment on barrier function and post-operative infectious complications in colorectal cancer surgery – a double-blind study. Aliment Pharmacol Ther. 2011 Jan;33(1):50-63. doi: 10.1111/j.1365-2036.2010.04492.x. Epub 2010 Oct 25. PMID: 21083585.
- Liu ZH, Huang MJ, Zhang XW, Wang L, Huang NQ, Peng H, Lan P, Peng JS, Yang Z, Xia Y, Liu WJ, Yang J, Qin HL, Wang JP. The effects of perioperative probiotic treatment on serum zonulin concentration and subsequent postoperative infectious complications after colorectal cancer surgery: a double-center and double-blind randomized clinical trial. Am J Clin Nutr. 2013 Jan;97(1):117-26. doi: 10.3945/ajcn.112.040949. Epub 2012 Dec 12. PMID: 23235200.
- Krumbeck JA, Rasmussen HE, Hutkins RW, Clarke J, Shawron K, Keshavarzian A, Walter J. Probiotic Bifidobacterium strains and galactooligosaccharides improve intestinal barrier function in obese adults but show no synergism when used together as synbiotics. Microbiome. 2018 Jun 28;6(1):121. doi: 10.1186/s40168-018-0494-4. PMID: 29954454; PMCID: PMC6022452.
- Axelrod CL, Brennan CJ, Cresci G, Paul D, Hull M, Fealy CE, Kirwan JP. UCC118 supplementation reduces exercise-induced gastrointestinal permeability and remodels the gut microbiome in healthy humans. Physiol Rep. 2019 Nov;7(22):e14276. doi: 10.14814/phy2.14276. PMID: 31758610; PMCID: PMC6874782.
- Pražnikar ZJ, Kenig S, Vardjan T, Bizjak MČ, Petelin A. Effects of kefir or milk supplementation on zonulin in overweight subjects. J Dairy Sci. 2020 May;103(5):3961-3970. doi: 10.3168/jds.2019-17696. Epub 2020 Mar 12. PMID: 32171508.
- Reddy VS, Patole SK, Rao S. Role of probiotics in short bowel syndrome in infants and children–a systematic review. Nutrients. 2013 Mar 5;5(3):679-99. doi: 10.3390/nu5030679. PMID: 23462584; PMCID: PMC3705313.
- Shing CM, Peake JM, Lim CL, Briskey D, Walsh NP, Fortes MB, Ahuja KD, Vitetta L. Effects of probiotics supplementation on gastrointestinal permeability, inflammation and exercise performance in the heat. Eur J Appl Physiol. 2014 Jan;114(1):93-103. doi: 10.1007/s00421-013-2748-y. Epub 2013 Oct 23. PMID: 24150782.
- Ferolla SM, Couto CA, Costa-Silva L, Armiliato GN, Pereira CA, Martins FS, Ferrari Mde L, Vilela EG, Torres HO, Cunha AS, Ferrari TC. Beneficial Effect of Synbiotic Supplementation on Hepatic Steatosis and Anthropometric Parameters, But Not on Gut Permeability in a Population with Nonalcoholic Steatohepatitis. Nutrients. 2016 Jun 28;8(7):397. doi: 10.3390/nu8070397. PMID: 27367724; PMCID: PMC4963873.
- de Roos NM, van Hemert S, Rovers JMP, Smits MG, Witteman BJM. The effects of a multispecies probiotic on migraine and markers of intestinal permeability-results of a randomized placebo-controlled study. Eur J Clin Nutr. 2017 Dec;71(12):1455-1462. doi: 10.1038/ejcn.2017.57. Epub 2017 May 24. PMID: 28537581.
- Stadlbauer V, Leber B, Lemesch S, Trajanoski S, Bashir M, Horvath A, Tawdrous M, Stojakovic T, Fauler G, Fickert P, Högenauer C, Klymiuk I, Stiegler P, Lamprecht M, Pieber TR, Tripolt NJ, Sourij H. Lactobacillus casei Shirota Supplementation Does Not Restore Gut Microbiota Composition and Gut Barrier in Metabolic Syndrome: A Randomized Pilot Study. PLoS One. 2015 Oct 28;10(10):e0141399. doi: 10.1371/journal.pone.0141399. PMID: 26509793; PMCID: PMC4625062.
- Wilms E, Gerritsen J, Smidt H, Besseling-van der Vaart I, Rijkers GT, Garcia Fuentes AR, Masclee AA, Troost FJ. Effects of Supplementation of the Synbiotic Ecologic® 825/FOS P6 on Intestinal Barrier Function in Healthy Humans: A Randomized Controlled Trial. PLoS One. 2016 Dec 9;11(12):e0167775. doi: 10.1371/journal.pone.0167775. PMID: 27936169; PMCID: PMC5147956.
- Leber B, Tripolt NJ, Blattl D, Eder M, Wascher TC, Pieber TR, Stauber R, Sourij H, Oettl K, Stadlbauer V. The influence of probiotic supplementation on gut permeability in patients with metabolic syndrome: an open label, randomized pilot study. Eur J Clin Nutr. 2012 Oct;66(10):1110-5. doi: 10.1038/ejcn.2012.103. Epub 2012 Aug 8. PMID: 22872030.
- Smecuol E, Hwang HJ, Sugai E, Corso L, Cherñavsky AC, Bellavite FP, González A, Vodánovich F, Moreno ML, Vázquez H, Lozano G, Niveloni S, Mazure R, Meddings J, Mauriño E, Bai JC. Exploratory, randomized, double-blind, placebo-controlled study on the effects of Bifidobacterium infantis natren life start strain super strain in active celiac disease. J Clin Gastroenterol. 2013 Feb;47(2):139-47. doi: 10.1097/MCG.0b013e31827759ac. PMID: 23314670.
- Kwak DS, Jun DW, Seo JG, Chung WS, Park SE, Lee KN, Khalid-Saeed W, Lee HL, Lee OY, Yoon BC, Choi HS. Short-term probiotic therapy alleviates small intestinal bacterial overgrowth, but does not improve intestinal permeability in chronic liver disease. Eur J Gastroenterol Hepatol. 2014 Dec;26(12):1353-9. doi: 10.1097/MEG.0000000000000214. PMID: 25244414.
- Pugh JN, Sparks AS, Doran DA, Fleming SC, Langan-Evans C, Kirk B, Fearn R, Morton JP, Close GL. Four weeks of probiotic supplementation reduces GI symptoms during a marathon race. Eur J Appl Physiol. 2019 Jul;119(7):1491-1501. doi: 10.1007/s00421-019-04136-3. Epub 2019 Apr 13. PMID: 30982100; PMCID: PMC6570661.
- Hałasa M, Maciejewska D, Baśkiewicz-Hałasa M, Machaliński B, Safranow K, Stachowska E. Oral Supplementation with Bovine Colostrum Decreases Intestinal Permeability and Stool Concentrations of Zonulin in Athletes. Nutrients. 2017 Apr 8;9(4):370. doi: 10.3390/nu9040370. PMID: 28397754; PMCID: PMC5409709.
- Davison G, Marchbank T, March DS, Thatcher R, Playford RJ. Zinc carnosine works with bovine colostrum in truncating heavy exercise-induced increase in gut permeability in healthy volunteers. Am J Clin Nutr. 2016 Aug;104(2):526-36. doi: 10.3945/ajcn.116.134403. Epub 2016 Jun 29. PMID: 27357095.
- Tran CD, Hawkes J, Graham RD, Kitchen JL, Symonds EL, Davidson GP, Butler RN. Zinc-fortified oral rehydration solution improved intestinal permeability and small intestinal mucosal recovery. Clin Pediatr (Phila). 2015 Jun;54(7):676-82. doi: 10.1177/0009922814562665. Epub 2014 Dec 16. PMID: 25520366.
- Davison G, Marchbank T, March DS, Thatcher R, Playford RJ. Zinc carnosine works with bovine colostrum in truncating heavy exercise-induced increase in gut permeability in healthy volunteers. Am J Clin Nutr. 2016 Aug;104(2):526-36. doi: 10.3945/ajcn.116.134403. Epub 2016 Jun 29. PMID: 27357095.
- Lamprecht M, Bogner S, Steinbauer K, Schuetz B, Greilberger JF, Leber B, Wagner B, Zinser E, Petek T, Wallner-Liebmann S, Oberwinkler T, Bachl N, Schippinger G. Effects of zeolite supplementation on parameters of intestinal barrier integrity, inflammation, redoxbiology and performance in aerobically trained subjects. J Int Soc Sports Nutr. 2015 Oct 20;12:40. doi: 10.1186/s12970-015-0101-z. PMID: 26500463; PMCID: PMC4617723.
- Luthold RV, Fernandes GR, Franco-de-Moraes AC, Folchetti LG, Ferreira SR. Gut microbiota interactions with the immunomodulatory role of vitamin D in normal individuals. Metabolism. 2017 Apr;69:76-86. doi: 10.1016/j.metabol.2017.01.007. Epub 2017 Jan 13. PMID: 28285654.
- Weir I, Shu Q, Wei N, Wei C, Zhu Y. Efficacy of actinidin-containing kiwifruit extract Zyactinase on constipation: a randomised double-blinded placebo-controlled clinical trial. Asia Pac J Clin Nutr. 2018;27(3):564-571. doi: 10.6133/apjcn.122017.03. PMID: 29737803.
- Spagnuolo R, Cosco C, Mancina RM, Ruggiero G, Garieri P, Cosco V, Doldo P. Beta-glucan, inositol and digestive enzymes improve quality of life of patients with inflammatory bowel disease and irritable bowel syndrome. Eur Rev Med Pharmacol Sci. 2017 Jun;21(2 Suppl):102-107. PMID: 28724171.
- Ciacci C, Franceschi F, Purchiaroni F, Capone P, Buccelletti F, Iacomini P, Ranaudo A, Andreozzi P, Tondi P, Gentiloni Silveri N, Gasbarrini A, Gasbarrini G. Effect of beta-glucan, inositol and digestive enzymes in GI symptoms of patients with IBS. Eur Rev Med Pharmacol Sci. 2011 Jun;15(6):637-43. PMID: 21796867.
- Aly AM, Al-Alousi L, Salem HA. Licorice: a possible anti-inflammatory and anti-ulcer drug. AAPS PharmSciTech. 2005 Sep 20;6(1):E74-82. doi: 10.1208/pt060113. PMID: 16353966; PMCID: PMC2750414.
- https://www.nccih.nih.gov/health/aloe-vera
- Suzuki T, Hara H. Quercetin enhances intestinal barrier function through the assembly of zonula [corrected] occludens-2, occludin, and claudin-1 and the expression of claudin-4 in Caco-2 cells. J Nutr. 2009 May;139(5):965-74. doi: 10.3945/jn.108.100867. Epub 2009 Mar 18. PMID: 19297429.
- Glenn JO, Wischmeyer PE. Enteral fish oil in critical illness: perspectives and systematic review. Curr Opin Clin Nutr Metab Care. 2014 Mar;17(2):116-23. doi: 10.1097/MCO.0000000000000039. PMID: 24500437.
- Weinstock, L. and Jasion, V. (2014) Serum-Derived Bovine Immunoglobulin/Protein Isolate Therapy for Patients with Refractory Irritable Bowel Syndrome. Open Journal of Gastroenterology, 4, 329-334. doi: 10.4236/ojgas.2014.410047.
- Chen Q, Chen O, Martins IM, Hou H, Zhao X, Blumberg JB, Li B. Collagen peptides ameliorate intestinal epithelial barrier dysfunction in immunostimulatory Caco-2 cell monolayers via enhancing tight junctions. Food Funct. 2017 Mar 22;8(3):1144-1151. doi: 10.1039/c6fo01347c. PMID: 28174772.

Discussion
I care about answering your questions and sharing my knowledge with you. Leave a comment or connect with me on social media asking any health question you may have and I just might incorporate it into our next listener questions podcast episode just for you!