Practitioner Case Study – October 2019
Dr. Michael Ruscio’s Monthly – Future of Functional Medicine Review Clinical Newsletter
Practical Solutions for Practitioners
In Today’s Issue
Case study
Research
- Ileocecal Valve & SIBO: Dr. Ruscio’s Mini-review
- Lead and cadmium exposure, higher thyroid antibodies and thyroid dysfunction in Chinese women
- Mast cells at the crossroads of microbiota and IBD
- Rapid-fire Research – ultra concise summaries of noteworthy studies
- Perspective: Fundamental Limitations of the Randomized Controlled Trial Method in Nutritional Research: The Example of Probiotics
- Serum Thyroglobulin-A Sensitive Biomarker of Iodine Nutrition Status and Affected by Thyroid Abnormalities and Disease in Adult Populations
![]()
Case Study
GI Retesting Looked Worse In A Case Where Symptoms Cleared, & Blood Markers Improved After Clearing GI Symptoms
Patient Info:
- Radul, 32y/o, Male
- Previous Dx
- High blood pressure
- Rx
- n/a
- Chief complaints
- Gas – flatulence + belching
- Bloating
- Stomach pain
- Insomnia (trouble falling asleep)
- Skin inflammation
Visit 1 (day 1) – History and Exam:
Initial impression
- Radul presents as a generally healthy 32yo male who has a good diet (AIP) and lifestyle.
- Dx/Rx:
- Dx: High blood pressure
- Rx: n/a
- Previous testing:
- n/a
- Onset:
- Has a history of antibiotic use, constipation, and hemorrhoids. His symptoms started when going vegetarian and under lots of stress. They responded very well to Autoimmune Protocol (AIP) but he still has some lingering problems.
- Family history
- High blood pressure
- Prior Treatments:
- Less exercise and more sleep/meditation help.
- Amino acids – made him bloated.
- Probiotics – helped but may bloat him.
- Paleo/AIP helped a lot.
- Notes/DDx
- Stomach pain may indicate ulcer – monitor the use of HCl.
- Radul is also eager to dial in his carbs (amount, type) for GI symptoms and for body comp. This will be easier to elucidate after addressing any GI imbalances.
- I anticipate typical imbalance (SIBO/dysbiosis) will be found and he will respond well to treatment.
- Prognosis
- Good to excellent
Previous diets:
- Paleo/AIP – helpful, though some symptoms remain
- Vegetarian – made it worse
- Some foods bloat him
Visit 2 (a few days later) – Testing and Initial Recommendations
Testing
- Tests ordered
- CBC w/ differential, CMP, lipid panel
- TSH, Free T4
- Aerodiagnostics Lactulose SIBO breath test
- Doctors Data Comprehensive Stool Analysis w/Parasitology x3
- Optional: Diagnostechs GI:15 stool/saliva test
- Rationale
- Standard GI workup for SIBO and dysbiosis. 2 stool tests likely not needed, this case study was from a few years ago when I was recommending more testing
- Standard blood chem workup, no suspicions, just a general check.
Recommendations
- Diet:
- Try eating more carbs before bed and see if this helps with sleep. If this doesn’t help try eating fewer carbs before bed and see if this helps.
- Perform modified fast.
- Next, continue with AIP reintroduction and start on a low FODMAP diet.
- After a few weeks on whole foods, try the semi-elemental diet using the modified fast instructions as a guide.
- NRT: Vitamin D, Magnesium
- Adrenal: Plant-based adrenal support
- GI: Lacto-bifido probiotic, boulardii, Digestive Enzymes
- Note: After a couple of weeks, add in Betaine HCl and see how you feel.
- Follow Up: Schedule once all labs are in.
- Rationale
- Will experiment with various carb intakes impact on sleep
- Move from AIP to low FODMAP – might be better for GI
- Will start with probios + enzymes and HCl, then layer in higher dose HCl to evaluate the impact
Visit 3 – Lab Interpretation and Treatment Evaluation
Subjective Assessment:
- Better overall, but still not perfect.
- Lacto/bifido probiotic, boulardii, and adrenal supplement all helpful.
- Betaine HCl upset stomach – even 1 cap
- Did not try elemental yet, will try next
- Improved:
- Sleep (eating carbohydrates before bed helped)
- GI Symptoms (low FODMAP and lower-carb have helped)
- Same:
- n/a
- Worse:
- n/a
Lab interpretation:
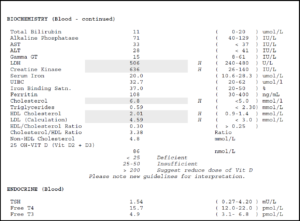
- Outside Labs:
- Cholesterol 6.8-H, HDL 2.01-H, LDL 4.59-H
- Creatinine 118-H, Gamma GT 506-H, Creatine Kinase 636-H
- Platelets 139-L, Lymphocytes 3.4-H
- TSH and Free T4 within normal limits
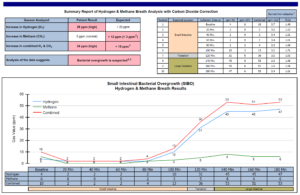
- Aerodiagnostics SIBO breath test:
- H2 10, CH4 3
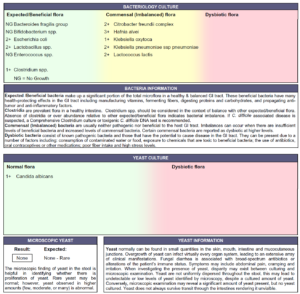
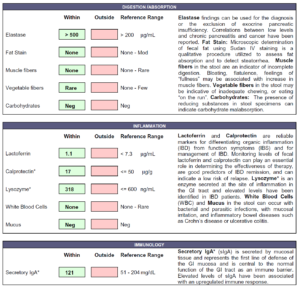
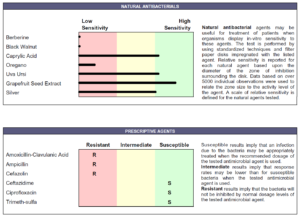
- Doctors Data:
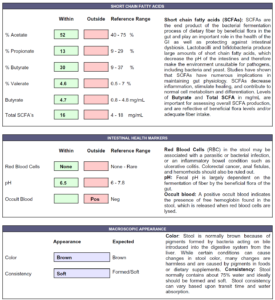
- Numerous commensal overgrowths, 1+ Candida albicans, occult blood.
- All IBD/functional markers within normal limits.
Impression:
- Radul is improving from diet and program – more treatment may not be needed. It was helpful to increase carbs, decrease FODMAPs and initial program. But betaine HCl aggravated the stomach. Decided on an aggressive approach; starting herbal antibiotics base with liver support and antioxidants.
- Potential mild distal mixed SIBO (NOTE: I no longer would classify this as such*)… Potential (platelet ddx); free radical damage, infection (viral, rickettsia, bacteria)
- Radul most likely has minor GI imbalance (potential SIBO, Candida) which will respond well to standard therapy. Since he is young and generally healthy the low platelets are likely from oxidative stress or are inconsequential but will retest after completing GI work.
Recommendations
Continue:
- Probiotics, digestive enzymes, adrenal support, vitamin D, magnesium
New:
- GI: Herbal antibiotics base protocol, liver/gallbladder support
- NRT: Immune/liver support supplement
- Discontinue betaine HCl
Follow up: 4-5 weeks
Visit 4
Subjective Assessment:
- Semi-elemental diet – was constipated and slightly bloated, but helpful after, bloating is decreased. Felt very hungry on the modified bone broth fast. He has noticed some high FODMAP foods bother him.
- Improved:
- Bloating, gas, GI discomfort
- Sleep
- Same:
- Fatigue
- Worse:
- n/a
Impression:
- Radul continues to improve with the addition of herbal antibiotics. The semi-elemental diet also seems helpful. Today ending herbals, starting melatonin, and will have him continue the foundational program, then f/u in 1-2 months and decide on retesting, program curtails and/or additional treatment.
Recommendations:
- Continue:
- Probiotics, digestive enzymes, adrenal support, vitamin D, magnesium
- New:
- Diet: Consider using a semi-elemental diet as a method to increase calorie intake as well as for meal replacement for intermittent fasting.
- NRT: melatonin, as needed
- Discontinue:
- Liver/gallbladder support, immune/liver support, herbal antibiotics
- Follow Up: 4-8 weeks
Visit 5
Subjective Assessment:
- Feeling much better. It’s been months since the last food reaction. Melatonin is helping with sleep. FODMAP reintroduction had some limitations.
- Improved:
- Bloating, gas, GI discomfort
- Sleep (still occasional insomnia)
- Fatigue
- Same:
- n/a
- Worse:
- n/a
Impression:
- Radul is going great and has maintained all previous improvements. Sleep is not perfect, however. Will start on Pregnenolone/DHEA now for additional energy support, and will retest and then follow up. Will start the program and plan to curtail at follow up.
Tests Ordered:
- CBC w/ differential, CMP, lipid panel
- TSH, Free T4
- Doctors Data Comprehensive Stool Analysis w/Parasitology x3
Recommendations:
- Continue:
- Probiotics, digestive enzymes, adrenal support, vitamin D, magnesium
- New:
- Adrenal: Pregnenolone/DHEA (1-3 months)
- Sleep: Try up to 12 mg of Melatonin for nights when it’s hard to sleep. If something stronger is needed, try OTC Unisom.
- Follow Up: 1-3 months, after re-testing has been performed.
Visit 6
Subjective Assessment:
- Still feeling well and doing great overall. Certain carbs can aggravate the gut.
- Improved:
- Bloating, gas, GI discomfort
- Sleep
- Fatigue
- Same:
- n/a
- Worse:
- n/a
Lab interpretation:
- Outside Labs:
- Mostly normalized. Normalization of: platelets, creatinine, creatinine kinase, GGT
- Abnormal/High: Lymphocytes, Total cholesterol, LDL, LDL/HDL ratio 4.6 (average: 4.4)
- Doctors Data:
- Less commensal dysbiosis, but now has 1 dysbiotic bacteria present.
- 1+ Candida albicans now cleared.
Impression:
- Today’s labs show GI that might have worsened, but hard to say. Blood labs have mostly normalized other than lymphocytes, total cholesterol, LDL, but LDL/HDL ratio is good (4.3).
- Radul has maintained improvements and is sleeping even better now with mindfulness practice. Today will start on Selenium and CoQ10 as cardio prevention (Radul is concerned due to family history). Will work to curtail the program.
Recommendations:
- Continue:
- Adrenal support, vitamin D, magnesium
- New:
- Experiment with lacto/bifido probiotic and boulardii on/off as needed.
- Cardio health: Selenium, CoQ10
- Discontinue:
- Pregnenolone/DHEA, melatonin, digestive enzymes.
- Follow Up: 2-4 months
Dr. Ruscio’s Comments
- Simple case of treating dysbiosis.
- Doctors Data GI labs might have been considered worse (he went from no dysbiotic organisms positive to 1 positive at retest even though symptoms improve. This showcases caution with treating labs only.
- Bloodwork imbalanced mostly cleared after GI work, mostly a bit of noise remained on lipid panel that was not concerning in aggregate
I’d like to hear your thoughts or questions regarding any of the above information. Please leave comments or questions below – it might become our next practitioner question of the month.

Like what you’re reading?
Please share this with a colleague and help us improve functional medicine












Discussion
I care about answering your questions and sharing my knowledge with you. Leave a comment or connect with me on social media asking any health question you may have and I just might incorporate it into our next listener questions podcast episode just for you!