Free Practitioner Case Study – June 2017
Dr. Michael Ruscio’s Monthly – Future of Functional Medicine Review Clinical Newsletter
Practical Solutions for Practitioners
In Today’s Issue
Case study
Research
- A review of functional foods for cardiovascular health.
- SIBO breath testing – updates according to the North American consensus.
- Does microbiota composition affect thyroid homeostasis?
- Can sun or UV exposure reduce mortality?
- Do antibacterial personal care products impact the microbiota or metabolism?
Practitioner Question of the Month
Practice Tip
Case Study
*Note: this is a long case study but it does teach us a few valuable lessons.
Patient Info:
- Jill
- Hypothyroid, C. difficile
- Synthroid
- Chief complaints
- Multiple BM through day (2-4, loose/greasy), occasional urgency
- Gas
- Nausea, stomach aches
- Occasional feeling of reflux
- Wakeful
Visit 1 – History and Exam
Jill presents as a very healthy 43 y/o female. She is eating well and does have some life stress but seems to be balanced. She also trains heavily (triathlete), which may be contributing to GI and/or sleep problems.
Her GI complaints started after treatment for C. diff; while her diarrhea was cured by Abx for C. diff, she had residual symptoms ever since. This makes C. diff or SIBO or candida highly suspected.
Nausea, stomach aches, and burning also suggest HP or ulcer. IBD is a remote possibility, with history of AI in her family and likely having autoimmune thyroid herself.
She has not done any other FM treatment and has not checked in with MD for a year+, so overall should be an easy case. Prognosis – good to excellent.
Initial impression:
- Jill likely has dysbiosis post antibiotics. She may also benefit from reduced training volume, at least initially while her GI rebalances.
Visit 2 (a few days later) – Testing and Initial Recommendations
Testing:
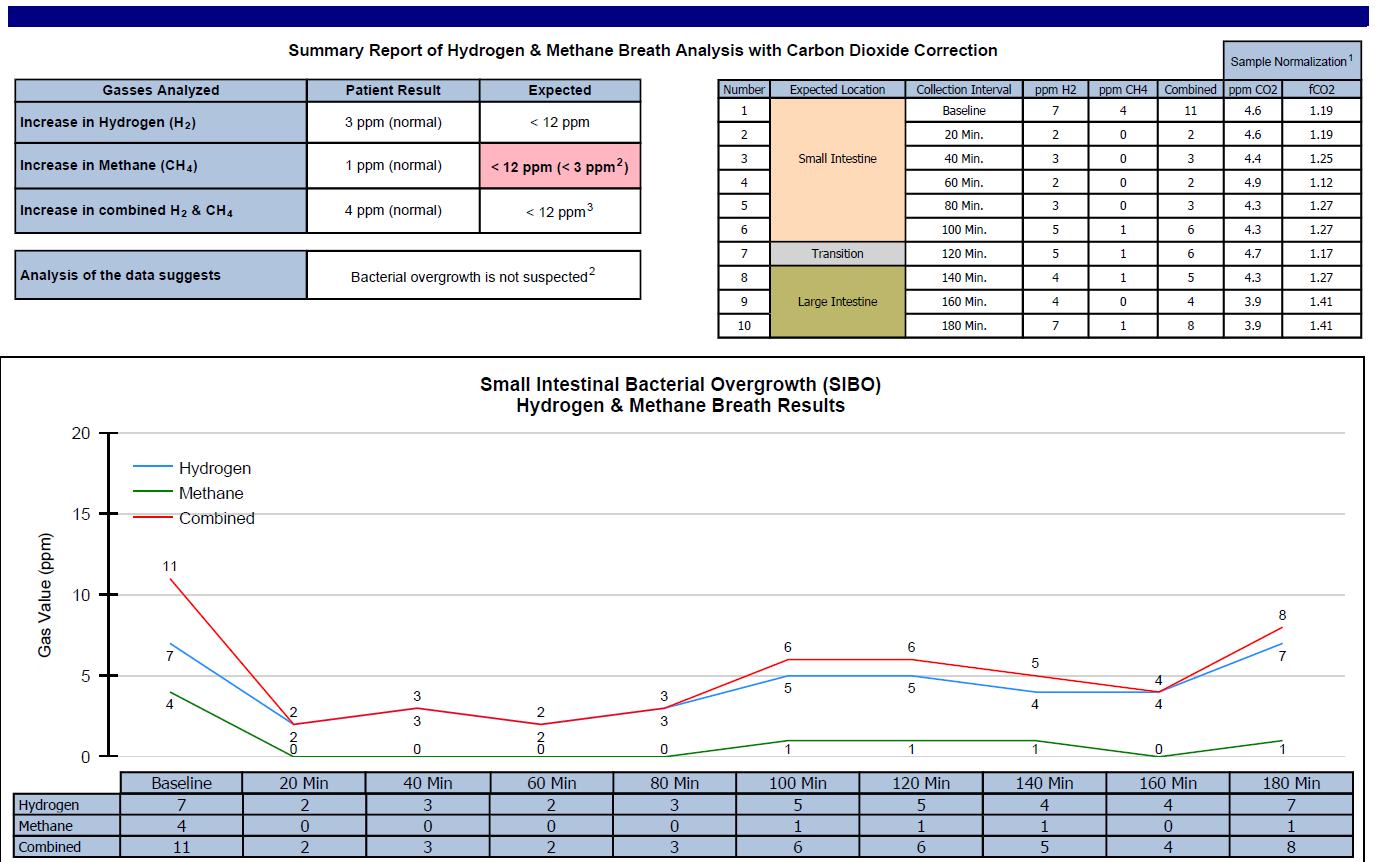
- Aerodiagnostics Glucose SIBO breath test
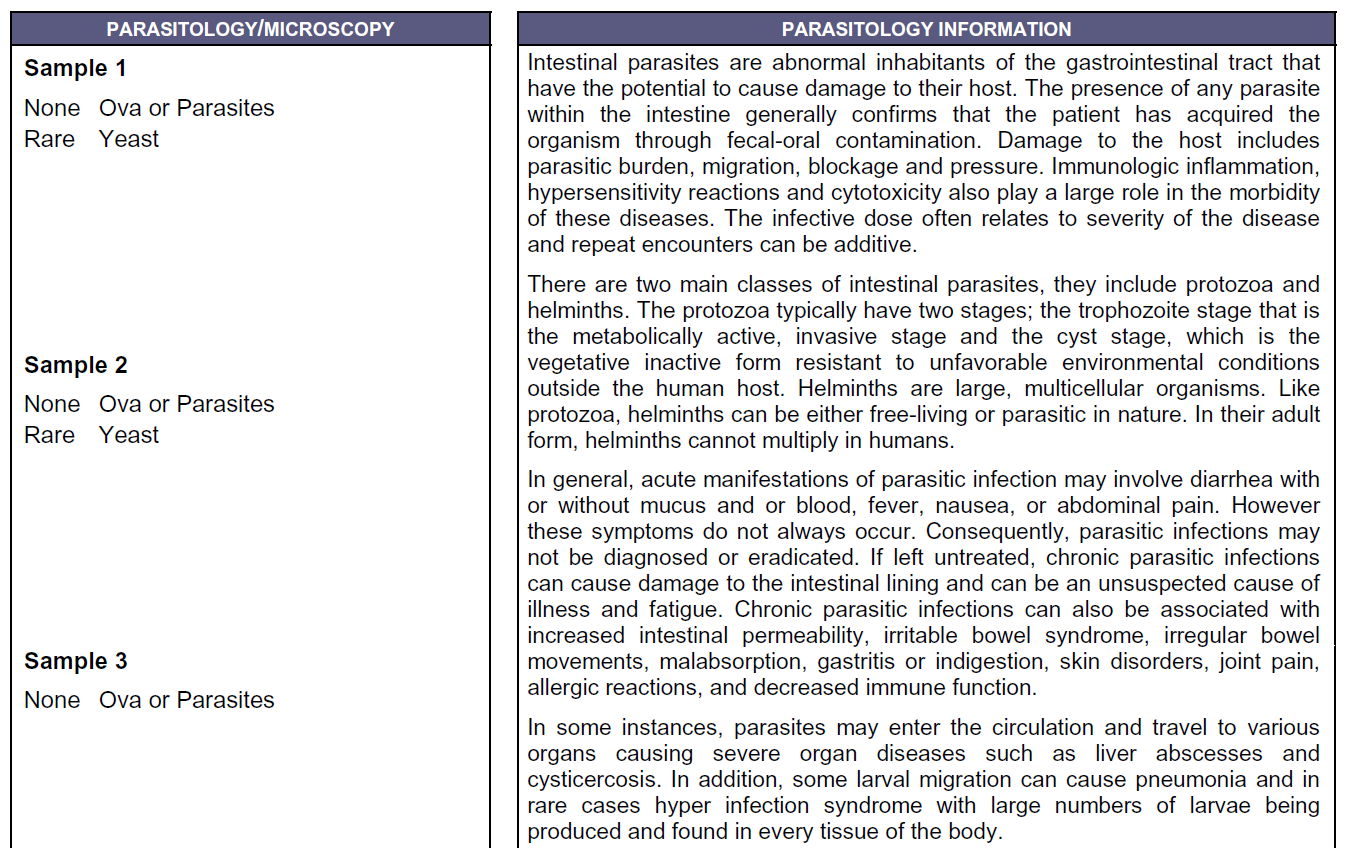
- Doctors Data Comp. Stool w/ Para 3x stool test
- Diagnostechs GI-15 stool/saliva test
- Custom blood panel
- CBC w/ Diff & platelet count
- Metabolic Panel, Comprehensive
- Thyroid-Stimulating Immunoglobulin (TSI)
- Thyroid Autoantibodies (TPO and TGA)
- Vitamin D
- Helicobacter pylori Antibodies, IgA, IgG, IgM
- Helicobacter pylori Urea Breath Test
Testing Rationale:
- SIBO is of course suspected.
- The expanded Doctors Data profile provides Lactoferrin and Calprotectin to rule out IBD.
- Since GI imbalance was highly suspected, 2 overlapping stools tests could be justified.
- Reflux, nausea, stomach aches support HP and/or ulcer, so ordering blood and breath testing for HP is important.
- Had not been tested for thyroid AI, so we included in our workup.
Recommendations:
- Consider performing the Whole 30 diet plan, work within the macronutrient ratios from your coach while on this diet.
- Consider taking 1 day off of normal training for restorative training – gentle yoga, stretching, foam rolling, etc.… Listen to our podcast with Ben Greenfield for more on how less is more with endurance training.
- GI:
- Lacto/bifido probiotic blend, S. boulardii, soil based probiotic, and digestive enzymes.
- Caution with the digestive enzymes, if they make you feel worse (nausea, stomach ache, burning) you can discontinue.
Recommendation Rationale:
- The main point here is caution with the enzymes, which contain HCl. If she does have ulcers/gastritis this could make her worse.
- We also addressed overtraining and make basic dietary and probiotics recommendations that can correct dysbiosis.
Visit 3 (day 30) – Lab Interpretation and Treatment Evaluation
Lab interpretation:
- Aerodiagnostics Glucose SIBO breath test – normal
- Doctors Data Comp. Stool w/ Para 3x stool test – Yeast 2x
- Diagnostechs GI-15 stool/saliva test – normal
- Custom blood panel – Alkaline Phos 38-L
- Summary: Yeast
Subjective Assessment:
- Digestive enzymes – are fine
- Has reduced exercise
- Feels removing gluten has been very helpful
- Improved:
- Bowels and urgency, normal stools. Gas (much better). Nausea, stomach aches. Reflux. Insomnia.
- Same/worse:
- N/A
Impression:
- Today Jill is doing so well there is no need for further treatment. We will continue with our current plan and then follow up in 2 months to reevaluate.
Recommendations:
- Maintain previous program
- Follow up in 2 months
Visit 4
Subjective Assessment:
- “Overall I’m feeling great and have no symptoms.”
Impression:
- Jill’s yeast dysbiosis has been remedied by a combination of probiotics, dietary (paleo/Whole30), and lifestyle (less training) recommendations.
Recommendations:
- Continue with current program
- Follow up in 3-12 months to curtail program, or as needed
Dr. Ruscio’s Comments
Jill’s case illustrates 2 very important concepts:
- Treat the person, not the labs.
- Don’t forget there are many GI imbalances that can be remedied without needing lab work.
Yes, we did find yeast, but our initial program was likely enough to correct this. How do I know this? Because all of her symptoms improved. Even if she retested for yeast and it came back positive, but was symptom-free, I would not directly treat the yeast. We could have retested, but together we elected not to.
I didn’t overzealously tell Jill to avoid all carbs (which feed yeast), or follow a candida diet, or that she ‘must retest’… these are all examples of the overkill FM approach. Jill’s case was simple: she had mild dysbiosis in the gut that responded to some simple GI interventions. We didn’t make the problem harder than it had to be. Jill experienced great results, quickly and inexpensively. Not every case is this straightforward, but it’s important not to treat a simple case like a complex case.
I’d like to hear your thoughts or questions regarding any of the above information. Please leave comments or questions below – it might become our next practitioner question of the month.

Like what your reading?
Please share this with a colleague and help us improve functional medicine
Discussion
I care about answering your questions and sharing my knowledge with you. Leave a comment or connect with me on social media asking any health question you may have and I just might incorporate it into our next listener questions podcast episode just for you!